Signs Your Milk Supply Is Decreasing—and How to Get It Back Up
It’s no secret that babies need a lot of calories and nutrition to fuel their growing little bodies. If you’re breastfeeding, you’re probably paying close attention to your breast milk production—and you may even be concerned about low milk supply. “I took my little one to the doctor and found out he’s not gaining enough weight,” says The Bump community member blessedinthewest. “He’s 3.5 weeks old, and he’s only gained 5 ounces in the last two weeks. Doc said it was due to low milk supply. This is so discouraging.”
But what are some surefire signs your milk supply is decreasing? And how can you increase your milk supply? Ahead, experts walk us through the signs of and reasons for low milk supply—and how to increase your breast milk supply quickly and efficiently.
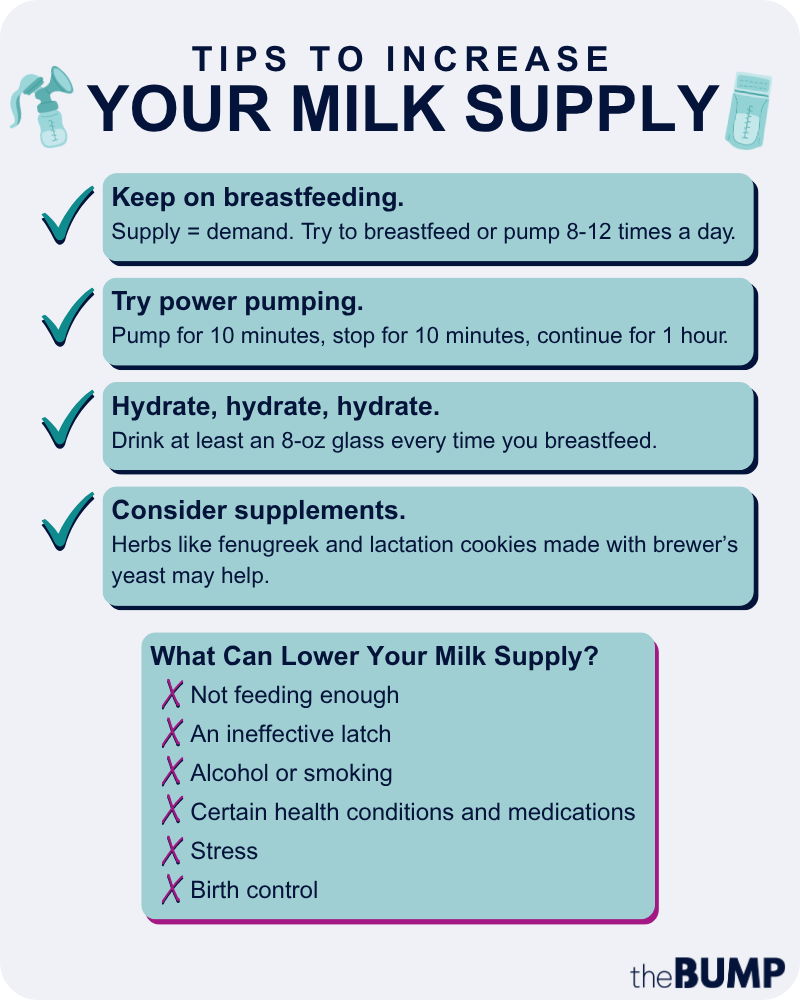
- Signs your milk supply is decreasing include baby not gaining weight, baby not making enough wet or poopy diapers, and baby getting fussy and hungry even after feedings.
- You may have low milk supply if baby isn’t feeding enough. It can also be caused by an ineffective latch, and sometimes certain health issues or medications.
- The best way to increase milk supply is to breastfeed or pump regularly. It’s also important to stay hydrated.
There are a few signs that point to low milk supply—but it’s important to keep in mind that these don’t automatically mean your milk supply is decreasing. It’s important to work with a lactation consultant to figure out the issue. “One of the most common reasons that moms stop breastfeeding is because of perceived low milk supply,” notes Jacque Ordner, IBCLC, RN, a lactation consultant, registered nurse and medical advisor at Motif Medical. “Many of the symptoms associated with low milk supply may actually be symptoms of poor milk transfer. It’s essential to work with an experienced IBCLC if you think your milk supply might be decreasing.”
That said, here are a few potential signs, according to experts:
Baby’s having weight gain issues
If baby’s not steadily gaining weight after they’re about 2 weeks old, there might be a low milk supply issue, says Delmar Bauta, a lactation specialist, traditional midwife and full-spectrum doula. “Normal weight gain is .5 to 1 ounce per day for the first four months. We want baby to double their birth weight by 4 to 6 months and triple it by one year.”
Baby’s not making enough wet or poopy diapers
If baby’s making fewer than six to eight wet diapers in a 24-hour period after their first week of life, that could be a red flag, says Bauta. Not peeing enough could also be a sign baby is dehydrated, which is another potential sign of low milk supply.
Baby’s fussy or hungry after feedings
If baby is fussy after eating “and doesn’t seem satisfied or fall asleep from nursing like they used to,” it might be due to low milk supply, says Nicole Peluso, IBCLC, manager of lactation services and education at Lactation Link by Aeroflow Breastpumps. And while cluster feeding is pretty normal in babies, it could also signal that baby’s trying to bring your milk production back up, says Danielle Downs Spradlin, IBCLC, owner of Oasis Lactation Services in Greater Minneapolis. “There often aren’t overt signs that the milk production is down, only the infant’s response to the decrease,” she adds. “Fortunately, increased nursing stimulates more milk production.” If cluster feeding lasts more than a couple of days, that could be a milk supply issue, says Melanie Kondrat, IBCLC, owner of Dragonfly Lactation in Knoxville, Tennessee. “Most babies feed every two to three hours or more frequently when growing rapidly or hitting a developmental milestone,” she adds.
Your pumping output is decreasing
“For parents who are exclusively pumping or pumping for most of baby’s milk, they may see a decrease in how much milk they’re collecting,” notes Spradlin. “This might not be decreasing milk production at all though—it could be a pump in need of service!” Make sure to have your lactation consultant check out your pump.
It’s natural to panic if you think baby’s not getting enough milk—and, trust us, we know that panic doesn’t mix well with those wild postpartum hormones! Take a deep breath and relax, because although low milk supply may seem like a mystery, it’s one you can usually solve. Here are the most common causes of low milk supply:
Not feeding enough
Many experts agree that not emptying your breasts completely or frequently enough is a common cause of low milk supply. “Human milk is produced to match the demand for it,” says Bauta. That’s why for the first few weeks, you should breastfeed or pump 8 to 12 times a day, or around every two or three hours, adds Peluso.
Supplementing with a bottle
Again, your body is built to produce as much milk as baby needs—so when baby breastfeeds often, your body understands there’s a high demand for milk and ramps up production. That’s why it might be wise to avoid supplementing with formula while you want to maintain your milk supply, says Peluso. If you’re introducing bottles of breast milk instead of nursing at the breast, it’s a good idea to still keep pumping while baby bottle feeds. Otherwise, if you skip the session entirely, your body will be tricked into thinking baby needs less milk and start to shrink the supply.
An ineffective latch
Sometimes, the problem isn’t with how often baby’s breastfeeding but how they’re feeding at the breast. A poor latch can play a role in low milk supply, says Peluso. When baby has a good latch, more milk comes out, and more milk is made.
Drinking alcohol or smoking
Both of these things can decrease milk supply. Generally, it’s advised to limit alcohol while breastfeeding and avoid smoking altogether.
Health issues or medications
It’s common for a mom’s breast milk supply to take a (temporary) dip if she’s sick with a cold or the flu. But other health conditions, like polycystic ovary syndrome (PCOS) or thyroid issues, can have a more lasting impact on breast milk production, as can prior breast surgery. Certain medications can also affect milk supply, like a combined contraceptive pill or a decongestant. Before taking any medications that may impact milk supply, be sure to consult your doctor first.
Rest assured that a decrease in breast milk supply is not a permanent problem. There are a lot of natural ways to increase milk supply and stimulate your milk ducts so they produce more breast milk. And the really good news is that most of these strategies are pretty simple to incorporate into your day-to-day routine.
Keep on breastfeeding
Suffice it to say: Supply meets demand. And so the more you breastfeed, the more milk you’ll produce. “The number-one priority for building and maintaining a good milk supply is frequent and effective breast stimulation,” says Peluso. “That means breastfeeding or pumping 8 to 12 times in 24 hours. Everything else is secondary.” Adds Spradlin: “Many people think they need to put their baby on a tight schedule, but every medical organization in the US and globally recommends cue-based feeding. Some cultures encourage babies to nurse multiple times each hour, especially for babies who are only a few weeks old. This is a great strategy for babies with tiny tummies.”
Pump to increase milk supply
Pumping to increase milk supply can be done by using your pump (hospital-grade double pumps work best) for every missed feeding or anytime baby gets a supplemental bottle of breast milk or formula. It’s also a good idea to express any leftover milk after each feed. Another option is power pumping one to three times daily to simulate cluster feeding, Kondrat says. “This looks like pumping for 10 minutes, stopping for 10 minutes and continuing this cycle for one hour.”
Drink plenty of water
You should also drink a ton of water to keep your supply in good shape. It makes sense that your body can’t produce ample milk if you’re dehydrated, so try downing an 8-ounce glass each time you breastfeed, plus a few more throughout the day.
Eat foods to help with breast milk supply
Wondering if you can eat certain foods to increase milk supply? Actually, it’s possible! There are several foods (and drinks) that have anecdotally been said to help get your milk flowing. And of course, these foods can be used in addition to other ways to increase milk supply, like pumping and taking supplements (just talk to your doctor first!). Here are some of the best foods to increase milk supply:
- Oatmeal. You can’t go wrong with oatmeal, since it’s both delicious and filling. “Quick oats, regular oats, steel-cut oats—oatmeal in all forms is said to increase milk supply,” says Leigh Anne O’Connor, IBCLC, a board-certified lactation consultant based in New York City. “People of some cultures even blend oats with water, then strain the oats from the water and use the remaining milky water as a supply-boosting drink.”
- Flaxseed. Thanks to their omega content, flax seeds are among the best foods to increase milk supply.
- Pumpkin. Fall might be the season of milk production for you, as research has shown that consumption of pumpkin is correlated with an uptick in supply.
- Fennel. Eat it raw, sautéed or roasted, and reap the rewards. Fennel has been shown to increase milk supply.
Additionally, Mayo Clinic advises breastfeeding moms fuel milk production with protein-rich foods, like lean meat, eggs, dairy, beans, lentils and seafood low in mercury.
Consider supplements to increase milk supply
Several herbs and supplements are considered to be effective galactagogues, and many moms have seen tangible results using them to increase milk supply. Many of these are the active ingredients in lactation cookies, teas and supplements.
- Fenugreek. “Fenugreek is probably the most common of the herbs to increase milk supply, and works well for many moms,” says Stephanie Nguyen, RN, IBCLC, founder of Modern Milk. “There are also supplement blends that contain multiple supplements in one pill. I prefer these because you may respond to one supplement and not another, so it’s best to try multiple supplements at once.”
- Blessed thistle. This is another galactagogic herb that lactation consultants often recommend in tandem with fenugreek. It’s often found in the supplement blend pills and in lactation tea as well.
- Alfalfa. Alfalfa has long been used by nursing mothers as an effective herb for increasing milk supply, and it boasts lots of other health benefits too. Alfalfa can be consumed in its plant form, in a pill or even as a tea.
- Brewer’s yeast. Typically sold in powdered form and admittedly not the tastiest ingredient on the planet, brewer’s yeast is most often used to make beer and wine. However, it has been considered effective at increasing milk supply, and is often one of the main ingredients in those super-popular lactation cookies. It’s packed with iron, protein and B vitamins, and is generally considered safe to consume.
Note that it’s important to talk to your physician before taking any herbs or supplements to increase milk supply. And if you’re given the go-ahead, know that once you reach a point where your supply is where you want it, you should stop use.
Increase your water intake, take fenugreek, increase your nursing sessions and pump after each nursing session. This worked for me.
Frequently Asked Questions
Why is my milk supply dropping?
The top cause of low milk supply is not feeding baby enough, say experts. If you want to maintain your milk supply, it’s best to feed baby on demand, following their cues. Also ask your lactation consultant to check your latch—a poor latch can contribute to dropping milk supply. Drinking alcohol, smoking, health issues and certain medications can also contribute to low milk supply.
How often should I breastfeed or pump to increase milk supply?
As a general rule, you should breastfeed or pump 8 to 12 times a day, or around every two to three hours while trying to get a steady supply. If you’re exclusively pumping, you’ll need to pump eight times a day for 15 to 20 minutes per session, says Ordner. If you’re both pumping and nursing, “the amount of pumping will vary depending on how far postpartum you are and how often and how well baby’s nursing,” she says. You can also try power pumping a couple of times a day, says Kondrat: Pump for 10 minutes, stop for 10 minutes and continue the cycle for an hour.
When does milk supply regulate?
For most moms, milk supply usually regulates around 4 to 6 weeks, says Peluso. You start your milk supply journey by producing colostrum for the first few days after birth, then you begin to produce transitional milk around days three to five and “continue to increase your milk volume for the first few weeks postpartum,” she says. After a few weeks, your body starts producing mature milk.
Can antibiotics decrease milk supply?
Most antibiotics are considered safe for breastfeeding, but some can affect your milk supply by interfering with milk-producing hormones, says Peluso. Another concern is that “antibiotics kill good and bad bacteria alike. This puts Mom and baby at risk for yeast infections and other gastrointestinal problems,” she says. Make sure to talk to your healthcare provider about alternative options, and consider taking pre- and probiotics and eating foods such as yogurt, kefir and kimchi “to help rebalance your microbiome after antibiotics,” she says.
Does milk supply drop when sick?
Yes, milk supply can temporarily drop when you’re sick, experts say. “This is because the body’s fighting off an infection and must redirect its resources,” notes Peluso. Try to stay hydrated and continue to breastfeed or pump to the best of your ability. Most moms find that their milk supply recovers after illness, she adds.
Can birth control decrease milk supply?
Yes, hormonal birth control can decrease milk supply for some new moms, says Peluso. The best practice is to wait six to eight weeks postpartum to start birth control again. “This allows your body to establish your milk supply first,” she says. Progestin-only birth control decreases your milk supply less than estrogen-based, but can still have an effect, she adds.
Can stress reduce milk supply?
Stress, fatigue and even grief can all lower milk supply, experts say. “It’s important to take care of yourself, especially when you’re recovering from birth and breastfeeding,” says Peluso. “Ask for help and prioritize what you need to stay hydrated, nourished and rested in order to set yourself up for breastfeeding success.”
Does caffeine decrease milk supply?
“Caffeine isn’t known to directly cause a dip in milk production, but excessive caffeine intake can make baby fussy and irritable,” says Ordner. “A fussy baby may not nurse as well, which can lead to a decrease in milk supply.” The general consensus on caffeine while breastfeeding is to keep it to 200 to 300 milligrams per day, according to La Leche League International.
Does alcohol decrease milk supply?
Yes, especially in larger amounts. “Alcohol can decrease milk supply by suppressing the let-down reflex and slowing milk flow,” says Ordner. “Studies show that babies drink significantly less milk when mom has consumed alcohol. Regular alcohol consumption can also lead to reduced prolactin levels, which causes a decrease in milk supply.”
Does beer increase milk supply?
While beer itself isn’t a galactagogue, the brewer’s yeast used to make beer (which is an ingredient in many lactation cookies) can be considered one, says Kondrat. However, you’d need to drink a lot of beer—which isn’t safe while you’re breastfeeding—to have any effect on milk supply, adds Peluso. In the past, she says, people brewed medicinal beers that were sometimes used as galactagogues, but “modern beer isn’t medicinal.”
Do Oreos increase milk supply?
Sorry—there’s no evidence that Oreos can help up your milk supply, says Peluso. And while there’s no need to avoid any foods while breastfeeding, it’s best to consume Oreos in moderation to avoid major blood sugar spikes. “Large blood sugar spikes, caused by sugary foods like Oreos, can lead to reduced milk production,” says Ordner, adding that this can especially affect moms with diabetes, insulin resistance and PCOS.
Does exercise affect milk supply?
There’s no evidence that moderate exercise affects milk supply in any way, says Peluso. While postpartum exercise is healthy, make sure to ease into it slowly, she adds—talk to your healthcare provider at your 6-week postpartum visit about being cleared for exercise.
Signs your milk supply is decreasing can often overlap with signs baby’s not feeding effectively. So it’s important to work with a lactation consultant to get to the root of the issue—and make sure both you and baby are happy.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Delmar Bauta is a lactation specialist, traditional midwife and full-spectrum doula with over 25 years of experience. They serve an international community of clients who seek the skills and knowledge to fully exercise their autonomy in reproductive and parenting choices.
Danielle Downs Spradlin, IBCLC, CLC, BRMT, NOMAS, is the owner of Oasis Lactation Services in Greater Minneapolis.
Melanie Kondrat, IBCLC, is the owner of Dragonfly Lactation in Knoxville, Tennessee.
Stephanie Nguyen, RN, IBCLC, is a board-certified lactation consultant and founder of Modern Milk, a breastfeeding clinic and prenatal-postnatal education center in Scottsdale, Arizona. Previously she has also worked as a postpartum, labor and delivery nurse. She received her master of science degree in nursing from the University of Cincinnati.
Leigh Anne O’Connor, IBCLC, BA, is a board-certified lactation consultant based in New York City. She has over 20 years of experience and has previously served as the president on the Board of the New York Lactation Consultant Association. She earned her bachelor of arts in communication from UNC-Greensboro, was accredited as a La Leche League Leader in 1997 and was board certified as an IBCLC in 2002.
Jacque Ordner, IBCLC, BSN, RN, RLC, is a lactation consultant, registered nurse and medical advisor at Motif Medical.
Nicole Peluso, IBCLC, CD, CAHPE, is the manager of lactation services and education at Lactation Link by Aeroflow Breastpumps. She is also a parenting educator certified by Attachment Parenting International, and a birth and postpartum doula trained at the National Midwifery Institute.
Drugs and Lactation Database, Alcohol, July 2023
La Leche League International, Will Caffeine Affect My Baby?, June 2021
Mayo Clinic, Breastfeeding Nutrition: Tips for Moms, April 2022
Plos One, Use and Experiences of Galactagogues While Breastfeeding Among Australian Women, July 2021
Veterinary Medicine International, Pharmacological Overview of Galactogogues, 2014
Real-parent perspectives:
- blessedinthewest, The Bump community member
- angeltex, The Bump community member
Learn how we ensure the accuracy of our content through our editorial and medical review process.
Target Baby Registry
Free $100+ Value Welcome KitFree $100+ Value Welcome Kit
15% Completion Discount15% Completion Discount
Free 1-Year ReturnsFree 1-Year Returns
20+ Exclusive 20% Off
Deals For Mom & Baby20+ Exclusive 20% Off Deals For Mom & Baby1:1 Concierge With
Baby Gear Specialists1:1 Concierge With Baby Gear Specialists

*Subject to availability and Retailer's terms.
We earn commissions from these links.