8 Breastfeeding Positions to Make Nursing Easier
Just because breastfeeding is natural doesn’t mean it’s second nature. Sometimes it takes time, practice and a whole lot of trial and error to get into a breastfeeding groove. Patience and persistence may be called for—right from day one. A newborn often wants to breastfeed soon after birth, so you want to have baby right there next to you, ready to drink up your colostrum—that’s the nutrient-packed early milk you express after delivering. While you’re in the hospital, take full advantage of the nurses and lactation consultants who can help you and baby perfect the breastfeeding latch and find the best newborn breastfeeding positions for you both.
“Baby’s latch depends on many factors, such as the size of your breasts and your own comfort level,” says Natasha K. Sriraman, MD, associate professor of pediatrics at Children’s Hospital of the King’s Daughter in Norfolk, Virginia. “The goal is to have baby’s mouth wide open, chin dropped and touching your breast, tongue down, with their lips flanged—not puckered in—on the areola.” Luckily, you can achieve the ideal latch in many different breastfeeding positions, so experiment and find the one (or ones) you like the most. Read on to learn about some of the best breastfeeding positions out there to make nursing easier, how to perfect them and which holds to use in various circumstances.
First off, there’s no right or wrong way to go about breastfeeding baby: “The only right type of breastfeeding position is a comfortable one that works best for Mom and baby,” Sriraman says. So feel free to try one or all of these breastfeeding positions—and keep in mind that what might work for you today can change down the road as baby grows and you both get more comfortable with the whole feeding thing.
Laid-back breastfeeding
“Many moms and babies love the laid-back breastfeeding position because it’s so natural for baby and relaxing for mom,” says Stephanie Nguyen, RN, MSN, IBCLC, a board-certified lactation consultant in Scottsdale, Arizona, and founder of Modern Milk. To do this one, you recline back about 45 degrees wherever you like to nurse—on the couch, in bed, on a recliner—and baby lies face down on top of your breast with their arms hugging your breast on both sides.
Football hold
Of the breastfeeding positions, football hold nursing—also sometimes called a clutch hold—is often the first moms learn. With football hold breastfeeding, baby is tucked under your arm off to the side (yep, like a football) and held with one arm while you support your breast with the other arm. If you’re holding baby on the right side, baby will latch onto your right breast while you support it with your left hand.
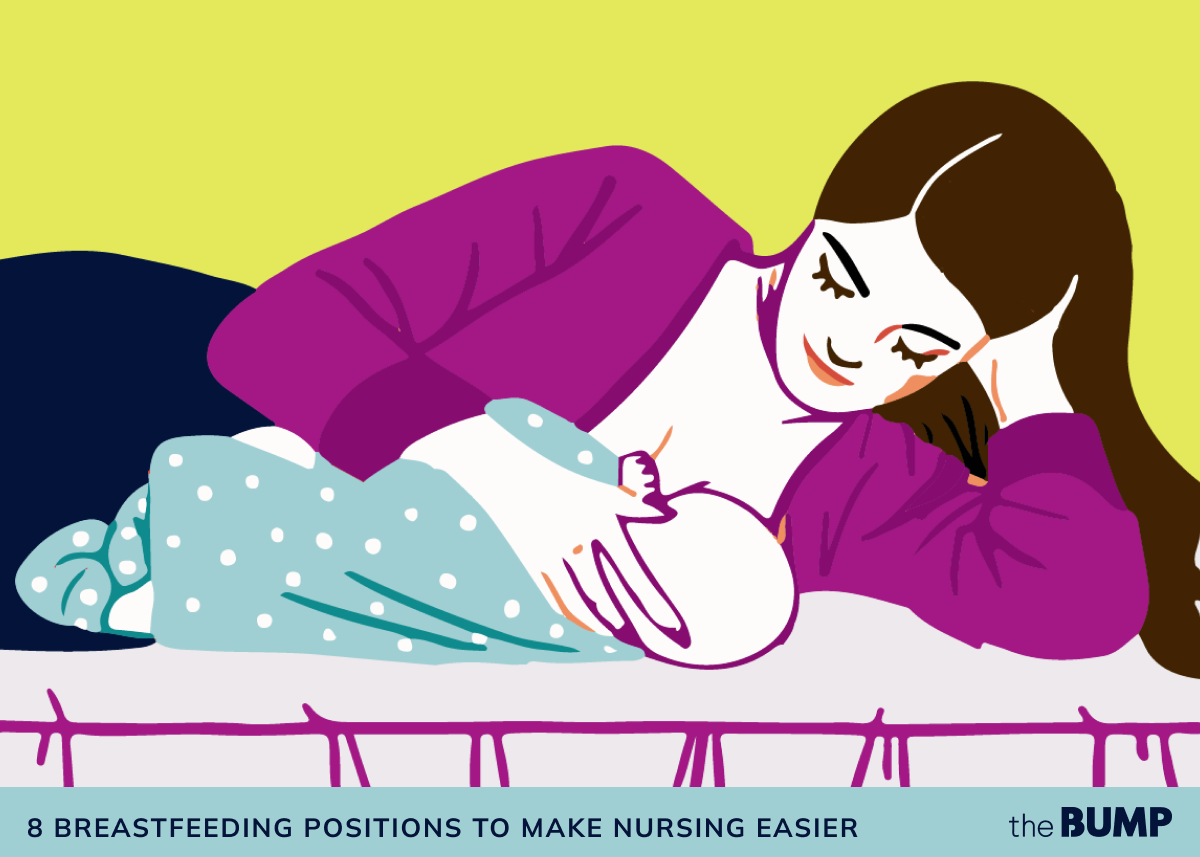
Side-lying position
For the side-lying breastfeeding position, lie down on your side with baby facing you. (You can put a breastfeeding pillow or a roll-up towel behind baby to support their back.) Baby nurses from the breast that’s resting on the bed. “Some moms may find it easiest to latch baby while sitting up and then slowly lie down until they get the hang of this position,” Nguyen says.
Cross-cradle hold
“Out of all the breastfeeding positions, this is the one most moms prefer because baby is draped across your body and you can easily see what they’re doing when latching,” Nguyen says. It’s also the easiest nursing-in-public position. To use the cross-cradle position, bring baby across your body, tummy to tummy, so if baby is nursing on your left side, you hold baby—supporting their neck—with your right arm and support the breast with your left hand. Lots of moms use a breastfeeding pillow when nursing in this position, since it can make it even easier and more comfortable. FYI: This is also a favorite position for bottle-feeding.
Cradle hold
This type of hold is very similar to the cross-cradle, but in this one you support baby with the arm on the same side as the breast they’re feeding from, not the opposite arm. This is one of the popular breastfeeding positions during the first few weeks of nursing, when you’re getting comfortable with your new job. Like with cross-cradle, a breastfeeding pillow can help lift baby and support your elbows.
Upright breastfeeding
For the upright breastfeeding position, sometimes called the koala or upright football hold, have baby sit upright, facing you and straddling your knee. You’ll support baby with the arm on the same side as baby is feeding and support your breast with the opposite hand, like in the football hold.
Positions for breastfeeding twins
If you have twins, your hands will certainly be full. “Simultaneous breastfeeding can be difficult and stressful,” Sriraman says. “When you’re just starting out, try breastfeeding each baby separately before trying to attempt two at time.” When you’re ready to nurse in tandem, try these positions for breastfeeding twins:
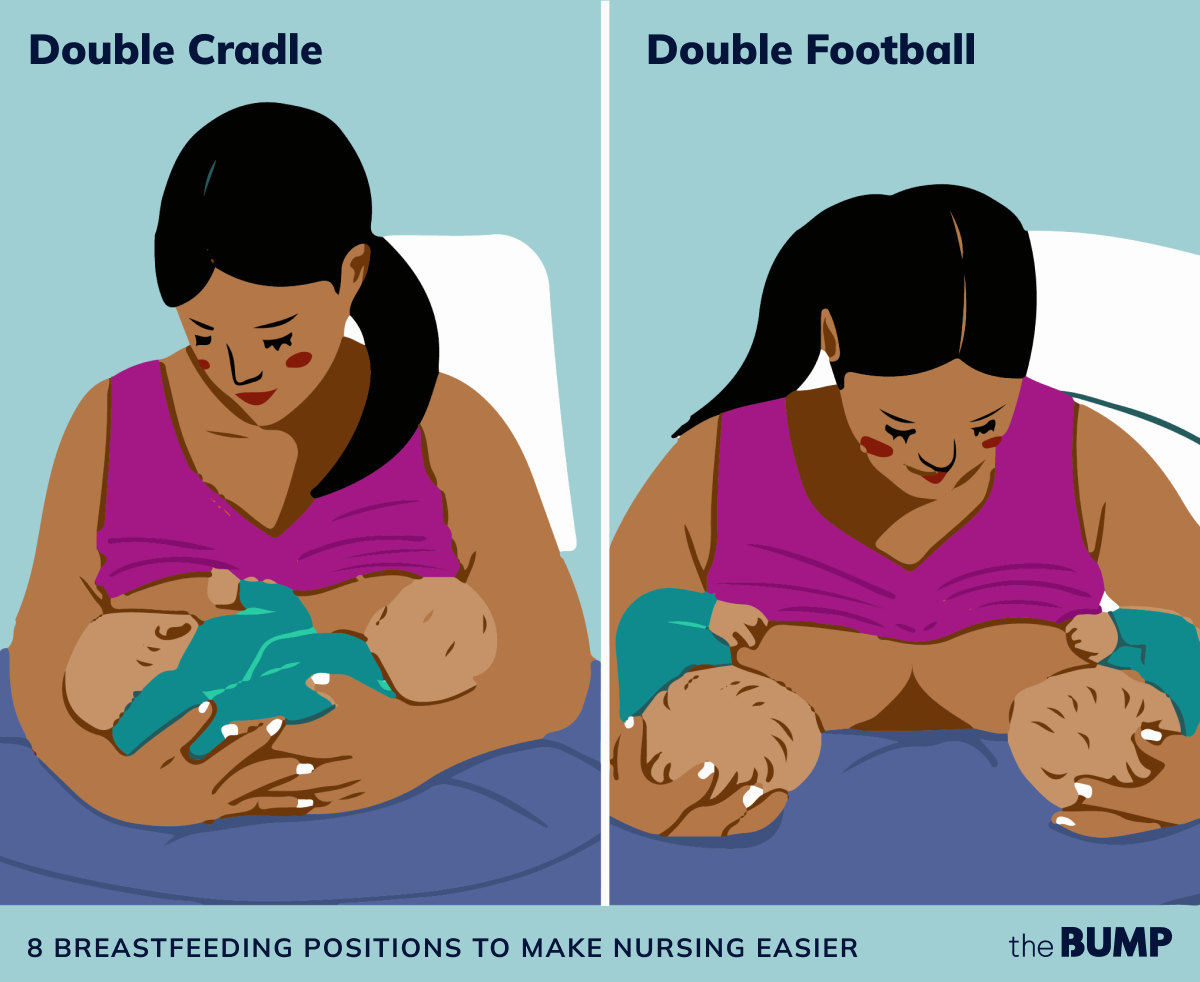
- Double-cradle hold. This breastfeeding position allows moms of multiples to nurse in tandem, often with a breastfeeding pillow under both babies. Each baby lays in the crook of each elbow, criss-crossing each other in your lap.
- Double-football hold. In this hold, your babies’ bodies rest on pillows along your sides and under your arms. You can also hold one baby in a cradle and one in the football breastfeeding position.
Different moms and new parents are going to find that different breastfeeding positions work best for them. But when you’re facing a common breastfeeding issue—whether it’s dealing with large breasts or nursing baby with reflux—certain breastfeeding holds can be better than others. Here, a few of the challenges many breastfeeding moms face, and the best breastfeeding positions to use.
Breastfeeding positions for large breasts
“Moms with large breasts often have difficulty supporting their breast during a feed and worry that the breast will smother baby during the feed,” says Sahira Long, MD, a lactation consultant and medical director of the Children’s Health Center at Anacostia, part of Children’s National Health System in Washington, DC. Many moms with large breasts find it easier to nurse in the side-lying breastfeeding position, so they can use the bed mattress to support the weight of their breast while getting a good view of baby’s latch, Long says. Another favorite breastfeeding position is the football hold nursing position. It can provide a better view of baby’s sucking, but remember to hold your breast throughout the nursing session to keep from putting a lot of weight on baby’s chin.
Best breastfeeding position for sore nipples
It’s common to feel some discomfort when you’re just starting out as your breasts get used to the process of nursing. “But there’s really no one breastfeeding position that’s best for sore nipples,” Long says. “Rather, it’s often advised that moms try to rotate between breastfeeding positions when their nipples are sore to avoid putting a lot of pressure from baby’s mouth on the same location.” When breastfeeding, many moms feel a pinching sensation that lasts only a few seconds—but if that pinch doesn’t go away immediately, or if your nipples continue to be sore three weeks after baby’s birth, there could be a problem with baby’s latch. It’s best to see a lactation specialist to have the latch evaluated, Long says.
Breastfeeding positions after C-section
When recovering from a C-section, it’s important to find a breastfeeding position that doesn’t put a lot of pressure on your surgical scar—otherwise, you can irritate the incision site and worsen your pain, Long says. Two best breastfeeding positions for moms who have had a C-section? The football hold (there’s less rubbing on the incision) and the side-lying position (so you can rest your tired body while baby feeds).
Breastfeeding positions for babies with reflux
For babies with reflux, upright or semi-upright positions are best, like the koala hold or laid-back breastfeeding position, since gravity will help with digestion, Sriraman says. “If baby’s reluctant to nurse because of reflux, try standing or walking while breastfeeding,” Nguyen says. “The gentle movements can help calm baby and encourage eating.” It’s also important to keep baby upright for 15 to 20 minutes after a feeding, either holding them over your shoulder or upright in an infant carrier. “After a feeding, it’s best to avoid seats or swings that place baby at a 45-degree angle,” Nguyen says. “This position actually puts pressure on the esophageal sphincter, making reflux worse.” If reflux is interfering with baby’s eating and gaining weight, make sure to follow up with your pediatrician.
Breastfeeding position to reduce gas
Babies can get gassy for different reasons. One culprit could actually be your own diet: Some foods may irritate baby’s digestive system if they have a food sensitivity (in which case, switching breastfeeding positions isn’t going to do much). Another cause is when baby takes in a lot of air during feedings. “This air has to be released in one direction or another. If baby doesn’t burp, they’ll likely become gassy,” Long says. Good news: This can be remedied with the proper breastfeeding positions, including upright or semi-upright positions, like the laid-back breastfeeding position. “Because milk isn’t flowing downward with gravity into baby’s mouth, they can control the milk flow better in this position, which helps avoid gas,” Nguyen says. If baby is experiencing a lot of painful gas, check on their latch. “If they’re gulping or taking in lots of air while nursing, they’re going to be gassy, no matter what position you feed in,” she says.
Now that you’ve zeroed in on the best breastfeeding positions for you and baby, you’ve got to learn how to do it on both sides. Here, some tips to help you get adjusted.
How to make the switch
If baby doesn’t break their latch by themselves, help by gently sliding your finger into the corner of their mouth, between their jaws. Baby will open their mouth, breaking suction and freeing your nipple. “Once baby has had a satisfactory nursing session on the first side, it’s a good idea to take a minute to burp them before offering the other side,” says Kathleen F. McCue, DNP, FNP-BC, IBCLC-RLC, a nurse practitioner and lactation consultant in Bethesda, Maryland.
When to change sides
“There’s no set amount of time that makes up a normal nursing session, but seeing active suck-swallow patterns from baby will let you know that they’re still receiving milk,” McCue says. Once that active pattern has stopped, you can move over to the second side. Most babies need to nurse from both sides to get enough milk. However, some babies will only need to eat from one side at a feeding. “Either option is normal as long as baby’s gaining weight, producing both wet and poopy diapers, and doesn’t flat-out refuse breast number two,” McCue says.
What if baby prefers one breast?
“Many women have one breast that has a faster flow of milk, which can make baby favor that side,” McCue says. Also, if you’re more comfortable nursing your newborn in, say, the cross-cradle hold and feeding from your left breast, baby may start to prefer that as well. “In most cases, there’s nothing that needs to be done about the preference. But if baby begins to refuse a side, you’ll need to focus on maintaining the milk supply in that breast via hand-expression or pumping, McCue says. You’ll also need to try gentle strategies to bring baby back to the other breast. One way is to offer your (full) neglected breast when baby is lightly sleeping or just waking up, or when they’re in the sling and you’re moving around.
Nursing isn’t a one-and-done process. It can take time for both you and baby to get adjusted to the different breastfeeding positions. Plus, problems can come up right from the start, or any time along the way. Here are a few more helpful tips to get you over any challenges.
- Find a support system. If you want even more guidance on best breastfeeding positions and solutions to nursing problems, looking for a local lactation consultant or breastfeeding-friendly pediatrician is a great place to start. “Mother-to-mother groups like La Leche League can provide excellent support for a new mom and help her feel more comfortable with normal breastfeeding behaviors,” McCue says. One thing to remember is that breastfeeding advice varies greatly, so if you aren’t getting the answers you need, don’t get defeated. Just move on and try getting another opinion.
- Get a nursing pillow. “A breastfeeding pillow can be helpful when nursing in cross-cradle hold or football hold,” Nguyen says. The best nursing pillows support baby and give your tired arms a break. (When nursing in the football hold, it’s actually best to turn the pillow to your side.) Some brands have a firm top and a strap that can secure the pillow around your waist. Avoid a soft sleeping or sofa pillow, which can put baby at risk of suffocation.
- Use a nipple cream. A poor latch is often to blame for many a sore nipple, so to truly fix the problem, you’ll want to start by working on that latch. But to soothe already-sore nipples, try a nipple cream. Look for ones that are safe to be in baby’s mouth and contain no allergens or additives, so it’s safe for your skin too.
- Try a nipple shield. Nipple shields are flexible silicone covers that fit over the nipple and areola and can help baby if they’re having trouble latching. To work effectively, nipple shields need to be sized properly for both your nipple as well as baby’s mouth, and they need to be attached so they draw in a lot of your breast. Since baby may get less milk if the shields are used incorrectly, it’s best to talk with a lactation consultant so they can help get you set up and make sure you’re using them the right way.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Sahira Long, MD, is a pediatrician and lactation consultant and serves as medical director of the Children’s Health Center at Anacostia, part of Children’s National Health System in Washington, DC. She earned her medical degree from George Washington University School of Medicine and Health Sciences.
Kathleen F. McCue, DNP, FNP-BC, IBCLC-RLC, is a nurse practitioner and lactation consultant in Bethesda, Maryland. She has helped more than 5,000 moms achieve a positive breastfeeding experience.
Stephanie Nguyen, RN, MSN, WHNP-C, IBCLC, is a registered nurse and board-certified lactation consultant in Scottsdale, Arizona. She’s also the founder of Modern Milk, a community wellness center that offers lactation support.
Natasha K. Sriraman, MD, MPH, FAAP, FABM, is a pediatrician at Children’s Hospital of the King’s Daughter in Norfolk, Virginia. In addition to seeing patients, she is an associate professor of pediatrics at Eastern Virginia Medical School. She received her medical degree from St. George’s University School of Medicine.
National Childbirth Trust, Skin-to-Skin Contact and Breastfeeding Right After Birth, March 2019
Learn how we ensure the accuracy of our content through our editorial and medical review process.
Target Baby Registry
Free $100+ Value Welcome KitFree $100+ Value Welcome Kit
15% Completion Discount15% Completion Discount
Free 1-Year ReturnsFree 1-Year Returns
20+ Exclusive 20% Off
Deals For Mom & Baby20+ Exclusive 20% Off Deals For Mom & Baby1:1 Concierge With
Baby Gear Specialists1:1 Concierge With Baby Gear Specialists

*Subject to availability and Retailer's terms.
We earn commissions from these links.