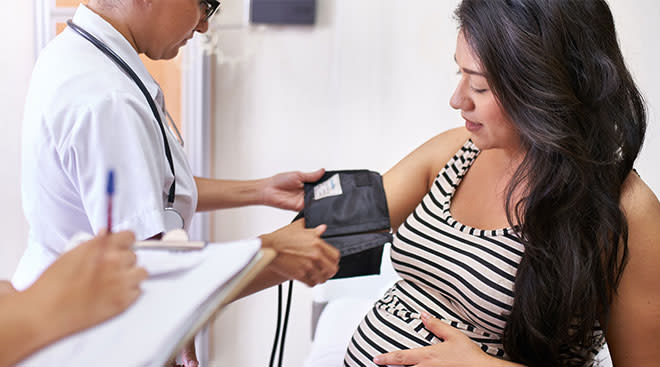
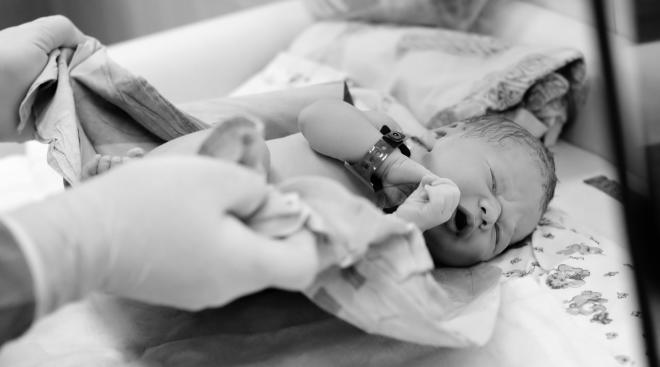
Why COVID Vaccines and Boosters Are Critical for Black Birthing People
It’s been nearly two years since the novel coronavirus outbreak was declared a global pandemic. None of us could have imagined how drastically our lives would change. Fortunately, one thing that has stayed the same is the miracle of pregnancy and birth, which continue to happen each day. As an ob-gyn, one of my most rewarding responsibilities is to help guide patients to a safe and healthy birth experience and baby. This journey has always involved protecting against infections that could prove harmful to a developing little one, including safe and effective vaccines against diseases such as measles, rubella and pertussis. While developed under urgent circumstances, the COVID-19 vaccines are no less safe, effective or important in achieving our most important goal: a safe pregnancy and healthy baby.
Let’s better understand these vaccines, dispel misinformation and understand the urgency for birthing persons, particularly African-Americans, to get both vaccinated and boosted. The pandemic is still very present in communities of color, and it’s far from over.
The conversation around COVID vaccines and boosters is particularly important for birthing people, as, according to the Centers for Disease Control and Prevention (CDC), those who are pregnant are more likely to become severely ill from COVID than non-pregnant people. While the overall risk is still low, birthing individuals are at increased risk for hospitalization, intensive care, the need of a ventilator to breathe and even possible death. They’re also at increased risk of poor pregnancy outcomes, including preterm birth and stillbirth, and potentially other pregnancy complications.
Moreover, we’re still learning about the potential long-term effects of COVID that some individuals experience. “Long COVID,” as it’s called, can last four or more weeks after the initial infection and result in significant long-term physical and psychological issues. Black birthing persons in the United States are already at higher risk of maternal death; we do not need to add potential negative outcomes due to COVID-19 as well.
Early in the pandemic, we identified individuals at high risk for severe disease and illness, including those over 65 year old, those with underlying medical conditions or with a compromised immune system. As the pandemic progressed, we realized that individuals from certain ethnic and racial minorities were also found to be disproportionately impacted—not solely due to medical conditions, but also due to systemic and structural inequalities, as well as social determinants of health (where people live, eat, work and play) that drive poor health outcomes. Specifically, African-American communities were, and continue to be, one of the hardest hit by COVID-19.
African-Americans remain disproportionately impacted by COVID-19. While Black people now have similar rates of infections to white people, the rate of severe disease continues to significantly outpace that of white populations: According to the CDC, the rate of COVID hospitalization is two and a half times higher for African-Americans, and the rate of death is nearly twice as high. This is particularly concerning for Black pregnant people, as COVID-19 infection is associated with increased risk of serious obstetric complications and maternal mortality. Moreover, according to a 2021 report, COVID-19 has lowered overall life expectancies in the Black community: The life expectancy of Non-Hispanic Black women has now dropped 2.3 years, compared to a decrease of 0.7 years for non-Hispanic white females.
Black birthing individuals remain one of the lowest populations of vaccinated individuals. This may be due to a mistrust of the healthcare system based on current and historical realities of unethical and poor medical treatment, but we must also recognize that vaccination and boosters are life-saving for both mother and baby.
Spoiler alert: Vaccines and boosters are safe, effective and free, regardless of insurance or immigration status. They’re now available at your local pharmacy, through vaccines.gov or at your local health department. Moreover, COVID-19 vaccination and boosters are recommended for pregnant persons, those who have recently been pregnant and those who are lactating to protect against severe disease. Due to the risks of COVID infection for this population, medical organizations such as the American College of Obstetricians and Gynecologists (ACOG) and the Society of Maternal-Fetal Medicine (SMFM) recommended vaccination in pregnant persons in July 2021. The CDC issued its official recommendation in August; additional groups, including the National Medical Association (NMA), reaffirmed this support in December 2021, given the worsening trends with the delta and omicron variants and low vaccination rate in this population. Current recommendations are for COVID vaccination as well as a vaccine booster shot, when appropriate, for maximal immunity.
Studies have found that COVID-19 mRNA vaccines are effective in pregnant persons and help lower the risk of COVID infection, similar to the general population. The estimated vaccine effectiveness after the second dose was found to be 96 percent for any confirmed infection, 97 percent for cases with documented symptoms and 89 percent for COVID-related hospitalization. Despite the normal physiological changes that tend to make pregnant people more at risk for infection and viruses (including COVID-19), the mRNA vaccines are effective and recommended to protect pregnant patients from illness.
Vaccines are not only effective, but they’re also considered safe for pregnant people. A recent study showed that COVID-19 vaccines do not affect male or female fertility—rather, it’s coronavirus infection that may temporarily impact male fertility. While potential impacts on birthing people weren’t specifically studied in the initial clinical trials, real-world data and subsequent and ongoing research all support the efficacy and safety of vaccination for birthing persons. A study found no indication of an increased risk for miscarriage prior to 20 weeks among individuals who received an mRNA COVID-19 vaccine just before or during early pregnancy. COVID-19 vaccines cannot cause COVID-19 infection in anyone, including a pregnant person or their baby.
In fact, studies have revealed that mRNA COVID-19 vaccines administered during pregnancy may help protect babies against COVID infection. When you receive the vaccine, your body produces antibodies against COVID-19. In pregnant people, those antibodies have also been found in their baby’s umbilical cord blood—meaning the parent’s protective antibodies were passed to baby, thereby protecting them against infection as well. Similarly, recent reports have shown that breastfeeding people who have received mRNA COVID-19 vaccines have antibodies in their breast milk, which are passed to their nursing babies and could help protect them against COVID infection.
COVID vaccine safety continues to be a top priority for all. Vaccine safety registries are an important way in which we continue to monitor for safety and side effects. Currently there is a V-safe pregnancy registry for pregnant women who have received the vaccine. It’s easy to enroll in from your phone and allows for the collection of information from persons who were pregnant or became pregnant after receiving the vaccine.
Are masks still necessary?
Yes! Mask requirements vary by city and county, but the CDC recommends that those who are not up-to-date with their vaccines and those with a weakened immune system should wear a mask when in a public indoor space. Even if you’ve been vaccinated, to maximize your protection and lower the chance of spreading COVID-19 to others, the CDC still recommends wearing a mask indoors, especially if you’re in an area of high transmission. Check with your local health department or the CDC website for the most current information regarding mask-wearing in your area.
Mitigation strategies that we’ve always used to reduce the spread of the virus—social distancing, mask-wearing and hand-washing—are even more important now due to the rise of more contagious variants. A well-fitting, high-grade mask such as a surgical, N95 or KN95 mask is the most protective type of covering. A recent study found that using a face mask or respirator in indoor public settings was associated with lower odds of contracting COVID, with N95 and KN95 respirators offering the highest protection, followed by surgical masks. Cloth masks by themselves are no longer considered adequate protection. Mask wearing must remain a mainstay of our overall fight against the coronavirus.
There are currently two types of tests available: the molecular tests (PCR) and the rapid antigen tests. While the PCR test is the most accurate and remains the gold standard for testing for COVID, home antigen testing kits are an important tool in the overall fight against the virus. These tests are most accurate when an individual is experiencing symptoms and their viral load is high.
Having these kits on hand is especially useful during cold and flu season, because many of the symptoms of these common viruses overlap with those of COVID-19, including fever, chills, cough, fatigue, headache, congestion, nausea and diarrhea. (Note: If you’ve lost your sense of taste or smell, it’s assumed to be COVID until proven otherwise.) If you’re not sure whether your symptoms could be COVID-19, don’t just assume it’s a regular cold or allergies—please test! The government is now providing free at-home testing kits, and is requiring commercial insurance companies and health plans to reimburse the cost of eight at-home tests per month for each covered individual.
Understanding what to do if you test positive or have a confirmed exposure is critical to reducing the potential spread to others. Visit the CDC website to get the latest recommendations for quarantine and isolation. Most importantly, check in with your health care provider for guidance based on your specific situation.
If you’re feeling overwhelmed by the stressors of this pandemic, you’re not alone. This is a difficult time for all of us—but we are all in this together. A key to managing these feelings is knowing the facts behind how to best protect yourself and your unborn child. Getting your vaccination and booster is your first line of defense. After all, they protect two lives, not just one! Next, ensure that you continue to follow those important risk-reducing strategies, which include wearing a mask, social distancing and washing your hands. Make sure to lean on your partner, family and friends for support as well. Self-care is so important in pregnancy, but particularly in the midst of a global pandemic. You may also need to seek professional help to see you through these challenging times—and that’s okay too! Give yourself the grace and kindness you’ve been trying to give others during this difficult time.
It’s normal to have questions and concerns about the use of any medication or treatment in pregnancy, and COVID vaccines are no exception. Talk it over with your OB, midwife or a health professional you trust, and visit CDC.gov for the latest, reliable information about the virus and what you need to do to keep yourself safe. Vaccinating and boosting yourself is not only important for yourself and your growing baby, but also for the community at large. The more individuals who remain unvaccinated, the more likely another variant, potentially one more infectious or aggressive, will develop. Let’s work together to keep our pregnancies and each other safe and put an end to this pandemic!
About the expert:
Rachel Villanueva, MD, FACOG, is a board-certified ob-gyn, women’s health expert and advocate for reproductive justice, health equity and disease prevention. She is the current president of the National Medical Association, the nation’s oldest and largest professional organization representing African-American physicians. She also serves as a Clinical Assistant Professor of Obstetrics and Gynecology at the NYU Grossman School of Medicine. Additionally, Villanueva is an ACOG fellow and serves on the Health Equity Subcommittee of the District 2 Safe Motherhood Initiative. She earned her medical degree, cum laude, from the Yale School of Medicine.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Navigate forward to interact with the calendar and select a date. Press the question mark key to get the keyboard shortcuts for changing dates.