What All Moms-to-Be Should Know About COVID in Pregnancy
Just as COVID has evolved since it first emerged in the US in January of 2020, so has experts’ understanding of the virus. And while there are still some unknowns, the only thing that seems more contagious than COVID itself is the spread of information—and misinformation. While it’s nerve-wracking for everyone, that’s especially true for pregnant people who need to keep themselves and their babies safe. Want to sort the facts from the fiction? Here is everything you need to know about COVID in pregnancy, straight from medical experts.
The 2019 novel coronavirus, known as COVID-19 or COVID, is a member of the coronavirus family, explains G. Thomas Ruiz, MD, ob-gyn lead at MemorialCare Orange Coast Medical Center in Fountain Valley, California. There are six other known coronaviruses, four of which cause a common cold, and two of which have caused more dangerous infections in the past: SARS (Severe Acute Respiratory Syndrome) in 2002 to 2003, and MERS (Middle East Respiratory Syndrome) in 2012.
COVID is contagious and spreads easily from person to person, explains Andres Romero, MD, an infectious disease specialist and medical director at AHMC Seton Medical Center in Daly City, California. While, in theory, it could infect someone if they touch a surface with the virus on it and then touch their face without proper hand hygiene, it’s much more likely to spread through air droplets that contain the virus, according to the Centers for Disease Control and Prevention (CDC).
What to know about COVID variants
Viruses are continuously changing and mutating, resulting in variants. The CDC explains it as branches growing on a tree. While the branches all grow from the same tree, each is slightly different. The bad news is that some variants make it easier for viruses to spread or make them more resistant to the vaccines and treatments being used against them, the org notes. At this point in time, the most prevalent strains are slight variants of Omicron, a more transmissible but potentially less severe strain, that was first discovered in November of 2021.
Research suggests that pregnant people aren’t necessarily more likely to contract the virus than a nonpregnant person, Ruiz says. However, the CDC emphasizes that they’re at an increased risk of severe illness if they do contract the virus.
What COVID might mean for Mom
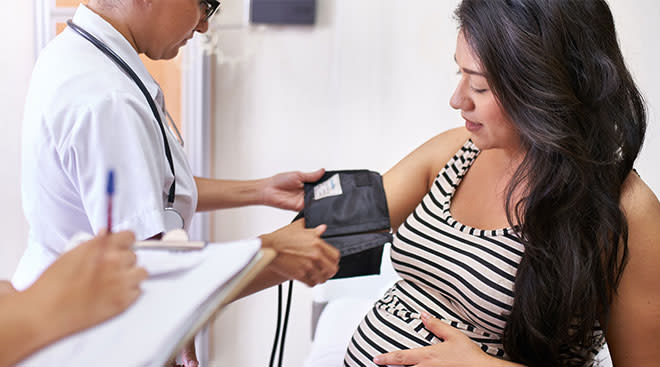
Overall, the risk of COVID-19 to pregnant women across the board is considered low, according to the Mayo Clinic. But that doesn’t mean you shouldn’t take specific precautions. “We know that COVID [can be] particularly problematic for pregnant people,” says Geeta K. Swamy, MD, a maternal-fetal medicine specialist at Duke Health in Durham, North Carolina. “Pregnant women are at a higher risk for complications, including hospitalization, requiring a ventilator for breathing and even death during pregnancy.” Additionally, she says the risk of death from COVID for a pregnant person can stretch into the first few weeks of the postpartum period. Finally, pregnant people with COVID are also at an increased risk of preterm birth and stillbirth, according to the CDC.
It’s still difficult for researchers to quantify exactly how much the risk of severe disease increases during pregnancy. But one 2021 study found that COVID-19 in pregnancy was associated with “consistent and substantial increases” in maternal death, severe maternal morbidity (health problems directly related to pregnancy and childbirth) and neonatal complications.
What COVID might mean for baby
Aside from the risk of preterm birth and stillbirth, contracting COVID in pregnancy doesn’t seem to pose a major risk to babies in-utero. “We aren’t seeing significant concerns where Mom is transmitting the virus to the baby, which is called vertical transmission,” says Swamy. This is not to say it never happens; some studies have proven there are instances where babies born to COVID-positive mothers tested positive themselves. Still, this seems to be the exception, not the rule. Moreover, there have been case reports of infants born to COVID-positive mothers that tested negative for the virus but had virus-specific antibodies.
According to Swamy, there’s nothing to suggest that COVID symptoms present any differently in pregnant people than anyone else. “Most [cases] start out similar to a common cold,” she says, “with a runny nose, cough, fever, body aches and headache.” Ruiz notes that some patients have also presented with fatigue, sore throat and shortness of breath.
Without a test, it’s difficult to discern whether someone with any of these symptoms has been infected with COVID, but this is especially true for expecting moms. “Pregnant people may already be feeling many of these symptoms outside of COVID,” explains Swamy, “such as being tired, having a stuffy nose or a headache.” Because of this, it’s important for pregnant people to monitor their symptoms closely and to call their doctor if symptoms last for more than a day or two, or if there was any known exposure to the virus.
If you have a known exposure to COVID, keep in mind that you may not experience symptoms right away. This is because the incubation period—meaning the time between catching the virus and when symptoms set in—is between one to 14 days, and an average of five days, according to Romero.
If you’re experiencing any symptoms of COVID during pregnancy, it’s important to call your doctor for advice on next steps. “Testing is especially recommended for those who are sick with fever, cough or difficulty breathing, and who have been in close contact with a person known to have coronavirus, or live in or have recently traveled from an area with ongoing spread,” Ruiz says.
There are two categories of COVID tests, according to the CDC: Viral and antibody. Whether you’re pregnant or not, there’s no difference in methodology for these tests.
Viral COVID tests are the most common, as they are used to determine whether or not someone is currently infected with the virus. They come in many forms such as PCR (polymerase chain reaction) laboratory tests, rapid antigen tests and at-home tests (which can be either rapid antigen tests that offer quick results or PCR tests that you send to a lab for results). Generally, PCR tests are considered the gold standard for accuracy, according to the Cleveland Clinic. It may take some time to get results from a PCR test though. Regardless of the test type, they all require a sample from either the nose (which is most common) or the mouth.
Antibody tests, on the other hand, are used to determine whether or not there are COVID antibodies in your blood, not to diagnose a current infection. The presence of COVID antibodies indicates that you contracted the virus at some point in the past. While these tests can be useful in some cases, Swamy notes that they’re not reliable in predicting whether a person will be infected with the virus in the future because people with antibodies can still get infected or reinfected with the virus.
According to Ruiz, mild cases are thought to last about two weeks, though more severe cases could last longer. “Fortunately, the vast majority of cases are mild,” he says, and can be treated in the comfort of your home.
Risk for severe illness aside, getting COVID during pregnancy can feel particularly rough because your options for over-the-counter medicines are limited. “At home, supportive or symptomatic treatment of COVID is okay with things like Tylenol,” says Swamy, but anything beyond that should be approved by your doctor.
Beyond over-the-counter medications, to date, the FDA has authorized the use of three antiviral medications for adults: Paxlovid (an oral tablet), Lagevrio (an oral tablet) and Veklury (intravenous infusions). Of these, the American College of Obstetricians and Gynecologists (ACOG) recommends Paxlovid as the preferred treatment option for pregnant people. Studies are still trying to determine how these medications can affect pregnancy and fetal development, but a November 2022 study from researchers at Johns Hopkins found that Paxlovid was safe to use to reduce the risk of severe COVID-19 infections during pregnancy. The CDC notes the medication should be started within five days of developing symptoms
Ultimately, it’s important to check in with your doctor about the infection’s severity and your options for treating COVID during pregnancy. If at-home treatment isn’t working and a pregnant patient is on the decline, Swarmy says that hospitalization may be necessary. But Alexa Mieses Malchuk, MD, MPH, an assistant professor at the University of North Carolina’s School of Medicine and a practicing family physician, emphasizes that “prevention is the best defense against COVID.”
Pregnant women can receive one of three approved COVID vaccines: Pfizer-BioNTech, Moderna or Novavax. While there was a fourth vaccine from Johnson & Johnson’s Janssen, the CDC notes the vaccine is no longer available in the US, as all government stock expired in May 2023. In September 2023, the FDA also approved updated Pfizer-BioNTech and Moderna vaccines, designed for stronger protection against the COVID variants currently circulating.
Wondering what the deal is with boosters for COVID vaccines? The CDC recommends everyone over the age of 5 receive one dose of any of the three updated vaccines (none are preferred over the other). Mieses Malchuk also encourages moms to get boosted as soon as they’re eligible. To learn more about each vaccine (including Johnson & Johnson’s Janssen), its ingredients, how it teaches the body to create an immune response and when to get your booster shot, visit the CDC website.
Should pregnant people get the COVID vaccine?
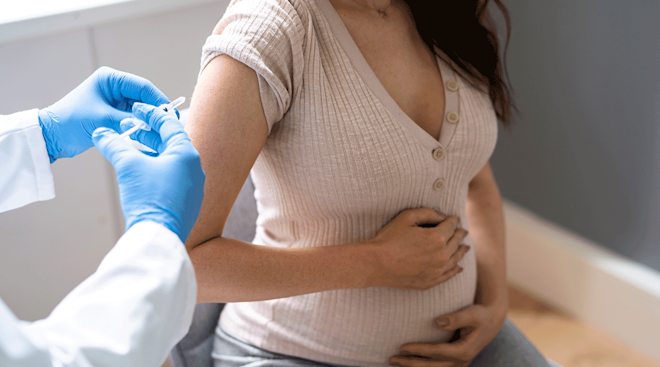
The best way to protect yourself from COVID is by getting vaccinated, both with the manufacturer’s regular dose(s) as well as recommended boosters. “The CDC, ACOG, American Society for Reproductive Medicine and the American Academy of Pediatrics all strongly recommend vaccination against COVID in all adults,” says Swamy. Given the increased risk for severe illness, hospitalization and death, this is especially true for pregnant women.
The CDC says all cumulative data and evidence suggest that the vaccine is effective and safe for Mom and baby. And while no vaccine offers 100 percent protection from a virus, the COVID vaccine does provide significant protection from serious illness, hospitalizations and death in pregnant women who are COVID-positive, Mieses Malchuk says.
Mieses Malchuk says there’s no evidence that there are any vaccine side effects specific to pregnant women. According to the CDC, the most common side effects include pain, redness and swelling at the injection site, as well as fatigue, headache, chills, muscle aches, fever and headache. You may feel uncomfortable, but these side effects are usually mild and should be gone within 24 to 48 hours.
Swamy stresses that there are no concerns for the developing baby or the pregnant pearson themselves in terms of the vaccine’s safety. In fact, getting vaccinated helps protect baby, since it significantly reduces Mom’s risk of complications like preterm birth and stillbirth. “The more severely ill Mom is, the more likely the pregnancy can be affected,” says Mieses Malchuk, “so the vaccine protects Mom and baby.” Also, studies have shown that moms who are vaccinated pass those antibodies to their babies in-utero as well as through their breast milk after birth.
Can the COVID vaccine affect future pregnancy?
There are a lot of rumors about the vaccine’s effect on fertility, but that’s all they are—rumors. “There’s no research whatsoever to suggest or support that the vaccine impacts your ability to get or stay pregnant in the future,” says Mieses Malchuk. The CDC also recommends the vaccine for women who are actively trying to conceive or plan to start trying in the near future.
Again, the most important step a person can take to protect themselves and her baby is to get the COVID vaccine during pregnancy (this includes booster shots). Beyond that, Romero stresses the importance of avoiding exposure to the virus in general. That means avoiding crowded indoor spaces, if possible, not touching your face with your hands and washing your hands frequently with soap and water for at least 20 seconds, he says. Regular use of alcohol-based hand sanitizer is also helpful in killing off any germs. You can also wear a well-fitted, multi-layer mask indoors when in public settings. The org and ACOG both note to wear a mask when:
- At high risk for severe illness from COVID (like during pregnancy)
- Taking public transportation or in travel hubs, like the airport or train station
- At a health care facility, such as a hospital (particularly during cold and flu season)
- When caring for someone with COVID
- When recovering from COVID
Of course, aside from these circumstances, the CDC notes pregnant people should continue to wear a mask whenever they wish.
Finally, be careful where you’re getting your information, Ruiz cautions. Make sure the recommendations you’re following are coming from a doctor or medical professional, the CDC or your local public health office. “There’s a lot of misinformation spread through social media, which may try to sell you unproven cures or treatments, or materials that won’t protect you from getting the illness,” Ruiz says. “Above all, stay calm, stay informed (from reliable sources) and stay prepared by exercising precautions.”
Between a pregnant person’s increased risk of severe illness from COVID, how easily the virus is transmitted and the very weak immune systems of newborns, the vast majorities of hospitals and birthing centers have implemented policies on what is and isn’t allowed in labor and delivery, postpartum recovery and neonatal intensive care units (NICU). Of course, every facility is different, so specific policies will vary, but some of the guidelines the CDC and ACOG recommend include:
-
If you’ve tested positive for COVID, you should notify your doctor or midwife of your infection; they will then alert your hospital/birthing center so that all members of your care team and infection control personnel are prepared.
-
If you’re symptomatic, you should be tested for COVID; it’s recommended that asymptomatic patients are tested as well.
-
Personnel should be wearing personal protective equipment around anyone who is COVID-positive; masks should be worn at all times around all patients.
-
Your visitors should be limited to people who are essential to your well-being and care (emotional support persons). They should be screened for COVID symptoms and shouldn’t be allowed into labor and delivery if they have any symptoms.
-
If you’re COVID-positive, you and baby will be isolated from healthy moms and babies in postpartum care. (Swamy notes that if you are COVID-positive and doing well, you shouldn’t have to isolate and separate from your baby.)
Again, these are guidelines, not absolute rules, so your personal experience will depend on what policies your hospital or birthing center have put in place. The good news is that “according to the CDC, the risk of Mom passing COVID on to baby is low,” says Mieses Malchuk. “But it’s not impossible.”
While staying together after birth has many benefits to both Mom and baby, she acknowledges that parents may have different levels of risk tolerance. “If Mom chooses to stay with her newborn, she should still wear a mask and practice all of the other infection control measures we know can lower COVID transmission risk.” What’s more, she stresses that “breastfeeding while COVID-positive is safe” (with those protective measures), and that a new mom who’s planning to nurse “shouldn’t delay breastfeeding her newborn.”
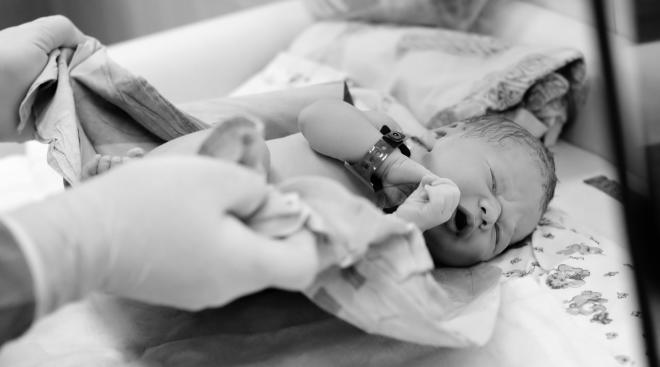
Since a newborn’s immune system isn’t fully developed, it’s understandable why you’d be nervous about keeping baby safe from COVID. The first (and best) thing you can do, according to all medical authorities, is to get vaccinated while you’re pregnant. “Mom’s immunity will get passed to the baby and will be especially present in the baby’s first few months of life,” Mieses Malchuk says.
Additionally, Mieses Malchuk explains how important it is for helpers and visitors who interact with baby to get their COVID shots and booster (as well as their flu and Tdap shots). Parents can also ask visitors and helpers to wear masks around baby for even more protection. Finally, anyone with known exposure to the virus or who shows symptoms of any kind should isolate away from baby until they get a negative COVID test.
All of the unknowns of COVID can be very scary during pregnancy, especially since you’re at a higher risk for severe illness. The best thing you can do? Get vaccinated and boosted, and take all of the precautionary steps to prevent exposure to the virus. Plus, don’t hesitate to reach out to your provider with any questions or concerns—they’re your best resource for getting credible, factual information.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Alexa Mieses Malchuk, MD, MPH, is an assistant professor in the department of family medicine at the University of North Carolina’s School of Medicine. She also practices family medicine at UNC and has a special interest in public health. She earned her medical degree and master of public health degree at the Icahn School of Medicine at Mount Sinai and completed her residency at Duke University Medical Center.
G. Thomas Ruiz, MD, is the lead ob-gyn at MemorialCare Orange Coast Medical Center in Fountain Valley, California. He earned his medical degree from UC Irvine School of Medicine and has been practicing medicine in Orange County since 1993.
Andres Romero, MD, is an infectious disease specialist and medical director at AHMC Seton Medical Center in Daly City, California. He received his medical degree from Greater College of Our Lady of the Rosary in 2009.
Geeta K. Swamy, MD, is a maternal-fetal medicine specialist at the Duke Perinatal Consultants of Durham and Fetal Diagnostic Center in Durham, North Carolina. She earned her medical degree from the University of North Carolina and completed her ob-gyn residency at the Magee-Womens Hospital in Pennsylvania.
Centers for Disease Control and Prevention, How COVID-19 Spreads, August 2022
Centers for Disease Control and Prevention, Variants of the Virus, February 2023
Centers for Disease Control and Prevention, SARS-CoV-2 Variant Classifications and Definitions, September 2023
World Health Organization,Classification of Omicron (B.1.1.529): SARS-CoV-2 Variant of Concern, November 2021
Clinical and Translational Medicine, The omicron variant of SARS-CoV-2: Understanding the known and living with unknowns, December 2021
Centers for Disease Control and Prevention, Pregnant and Recently Pregnant People, October 2022
Mayo Clinic, Pregnancy and COVID-19: What are the risks?, 2023
JAMA Pediatrics, Maternal and Neonatal Morbidity and Mortality Among Pregnant Women With and Without COVID-19 Infection, April 2021
Journal of Nepal Health Research Council, Vertical Transmission of COVID-19: A Case Report and Review of Literature, April 2021
Journal of Medical Virology, Possible vertical transmission and antibodies against SARS-CoV-2 among infants born to mothers with COVID-19: A living systematic review, March 2021
Centers for Disease Control and Prevention, COVID-19 Testing: What You Need to Know, September 2023
Cleveland Clinic, COVID-19 and PCR Testing, August 2021
American College of Obstetricians and Gynecologists, COVID-19 FAQs for Obstetrician-Gynecologists, Obstetrics, 2023
Johns Hopkins Medicine, Study Shows Paxlovid Can Safely Be Used to Reduce Risk of Severe COVID in People Who Are Pregnant, November 2022
Centers for Disease Control and Prevention, COVID-19 Treatments and Medications, October 2023
Centers for Disease Control and Prevention, Janssen (Johnson & Johnson) COVID-19 Vaccine, May 2023
US Food and Drug Administration, FDA Takes Action on Updated mRNA COVID-19 Vaccines to Better Protect Against Currently Circulating Variants, September 2023
Centers for Disease Control and Prevention, Stay Up to Date with COVID-19 Vaccines, October 2023
Centers for Disease Control and Prevention, Overview of COVID-19 Vaccines, October 2023
Centers for Disease Control and Prevention, COVID-19 Vaccines While Pregnant or Breastfeeding, September 2023
Centers for Disease Control and Prevention, COVID-19 Vaccines While Pregnant or Breastfeeding, September 2023
Centers for Disease Control and Prevention, Getting Your COVID-19 Vaccine, September 2023
Vaccine, COVID-19 booster vaccination during pregnancy enhances maternal binding and neutralizing antibody responses and transplacental antibody transfer to the newborn, August 2023
Centers for Disease Control and Prevention, Use and Care of Masks, May 2023
Centers for Disease Control and Prevention, COVID-19
American College of Obstetricians and Gynecologists, COVID-19, Pregnancy, Childbirth, and Breastfeeding: Answers From Ob-Gyns, October 2023
Learn how we ensure the accuracy of our content through our editorial and medical review process.
Navigate forward to interact with the calendar and select a date. Press the question mark key to get the keyboard shortcuts for changing dates.