Can Breast Milk Protect Against COVID-19? a Researcher Hopes to Find Out
A researcher from the Icahn School of Medicine at Mount Sinai in New York City is in search of spare breast milk.
Rebecca Powell is a human milk immunologist looking to find out if breast milk has the power to protect babies—and even adults down the line—from COVID-19. A few days ago, she issued a call for it on social media. Since then, she’s heard from a surprising number of women.
“There’s a lot of lactating people out there that are getting infected and would be ready and willing to donate milk. I can tell you because I have hundreds of emails from people who want to participate, and many of them have said they had highly suspected infection or a positive test,” Powell told VICE News in an interview. “They’re out there, and I don’t think it should be overlooked.”
Breast milk has long been believed by the AAP and many other experts to protect against a variety of diseases and conditions in infants. It contains antibodies that, along with immune cells, can protect newborns from viruses in those first few months of life. Currently, the CDC believes, with proper precautions, moms with COVID-19 can continue breastfeeding their babies.
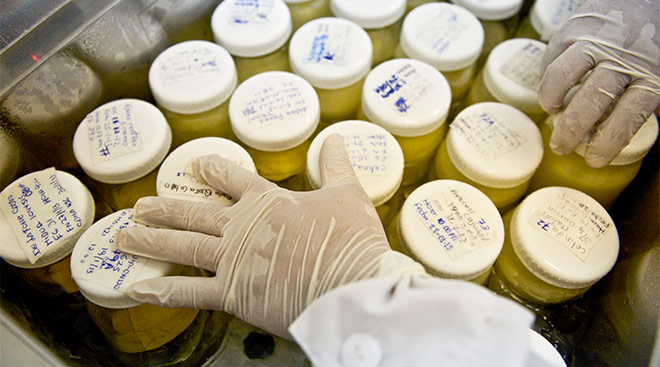
For her research, Powell is looking for samples particularly from healthy, lactating women living in New York City and is even willing to pay $5 per ounce of milk. She is accepting samples via mail from women outside of the city, as long as they have either a confirmed or suspected case of COVID-19 or are at high risk for exposure to it. She says these samples should be pumped and frozen. Powell will be collecting samples for one year or longer, although women can choose to opt out whenever they wish.
She will first check these samples for antibodies to see if the women were infected with or exposed to COVID-19. Then, she will examine how many and the class types of the antibodies in the milk, how strong they are and whether they would be able to, either by themselves or by provoking other cells, ward off the virus. “It was never done with SARS, it was never done with MERS, and even for flu, which is so well-studied. The data on milk protection is actually really sparse, unfortunately,” Powell said.
Even now, many researchers are looking at the antibodies found in the blood and convalescent plasma of recovered COVID-19 patients to see if they can be used in testing for or treating the virus. According to a recent, limited study published in Proceedings of the National Academies of Sciences, this may be an effective treatment option. The study looked at researchers at three hospitals in China who infused a dose, using antibodies from the blood of recovered patients, to 10 very ill patients. According to their preliminary findings, the patients saw their symptoms subside.
Of course, more research is needed, and Powell believes that human milk may provide a better treatment option than blood, as 90 percent of milk antibodies are particularly durable and resistant to degradation. She explains that, if milk does prove as an effective protector, people wouldn’t be getting it directly—the antibodies in the milk would first be purified and then transfused.
“You can take it one step further because you can ask the question, ‘Well, if we find that there’s really potent antibodies in the milk, can those be used therapeutically in a way that Mt. Sinai and other hospitals are now using convalescent plasma to treat those who are really ill?” Powell tells the outlet.
As scientists continue to look for a treatment for COVID-19, Powell poses an interesting question. Can breast milk really protect against the virus the way it does against other conditions? Only time will tell. After all, Powell has just begun her quest for answers.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Navigate forward to interact with the calendar and select a date. Press the question mark key to get the keyboard shortcuts for changing dates.