Revolutionary Wireless Sensors Could Allow Skin-to-Skin Contact With NICU Babies
A set of wireless sensors has the potential to advance NICU technology. It’s still waiting approval, but the battery-free sensors are designed to be more comfortable for premature babies, while still collecting vital signs, National Geographic reports. The research was published in the journal Science, and comes from a collaboration of material scientists, dermatologists, pediatricians and students affiliated with Northwestern University.
The study was conducted at Prentice Women’s Hospital and Ann and Robert H. Lurie Children’s Hospital of Chicago, where 21 infants were monitored by traditional wires while simultaneously monitored by the new sensors. The new sensors were able to capture all the important information as well as blood pressure estimates.
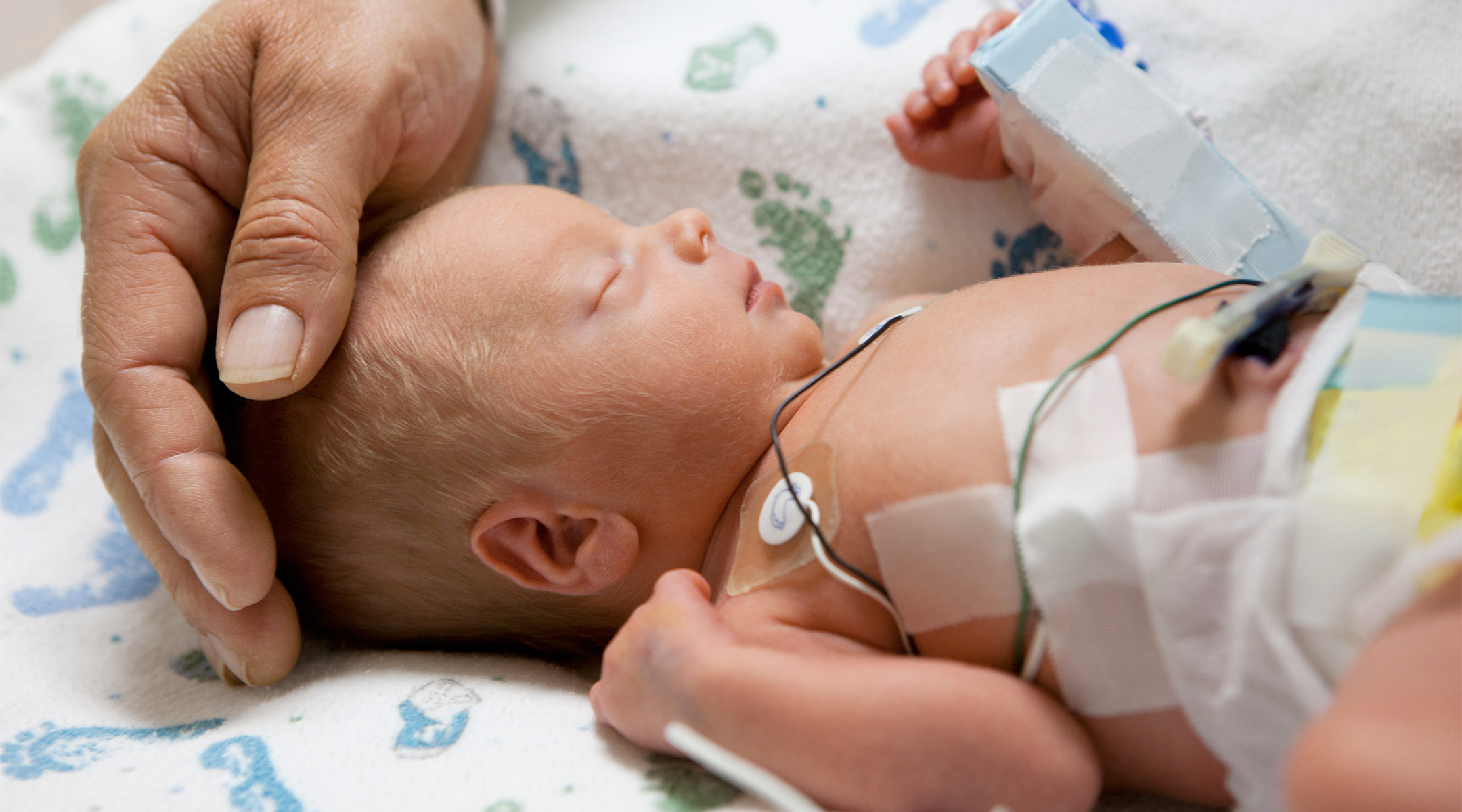
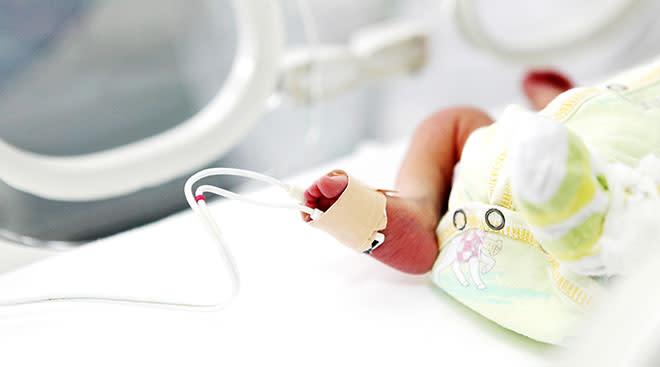
Babies in the NICU are typically secured to wires to monitor vital signs like body temperature, heart rate, blood oxygen and more. If the new sensors get approved, it’ll virtually eliminate all of the wires.
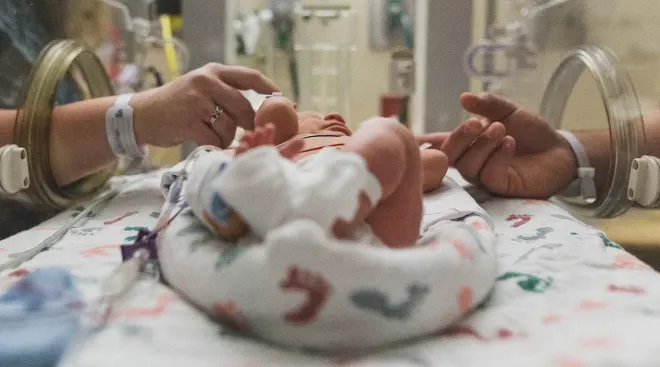
Instead, the sensors are fastened to a baby’s chest and foot so they can collect and stream the baby’s vitals to a tablet, where data is read by NICU nurses and other medical professionals. The sensors were also developed with comfort in mind. When a baby is born early, the outer layer of skin hasn’t fully developed, so even slight tugs can cause pain or infection. The new sensors are ultra-thin and soft to avoid discomfort for baby.
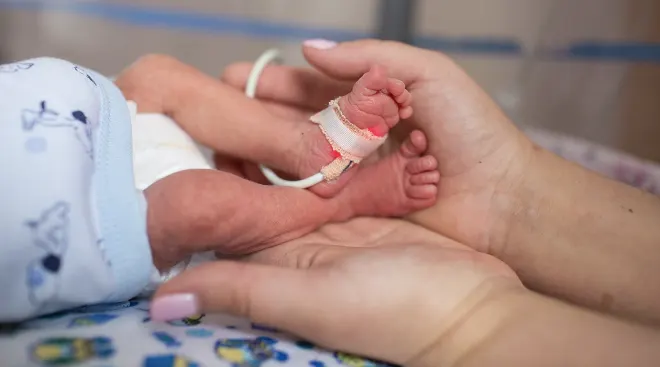
And skin-to-skin bonding with premature babies isn’t always possible for parents when their baby is hooked up to several machines and wires. The sensors, however, would allow new parents more of a chance to enjoy a snuggle with baby. While skin-to-skin helps mom bond with baby, studies of full-term babies have also linked it to better respiratory function, longer breastfeeding sessions and stabilized body temperature.
With that in mind, there are some cords the sensors can’t eliminate. Many babies in the NICU require feeding tubes and other lines, as well as oxygen support systems called CPAP to assist with breathing.
While the sensors haven’t been approved by the FDA yet, the study’s authors think once it passes the review stage, they could be administered in hospitals in as a little as two years.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Navigate forward to interact with the calendar and select a date. Press the question mark key to get the keyboard shortcuts for changing dates.