How to Prevent and Treat Hand, Foot, and Mouth Disease
The mere mention of “hand, foot and mouth disease” is enough to make any parent shudder. This common childhood illness is incredibly contagious and can tear through playrooms, daycare centers and preschool classrooms at an alarming clip. And while its symptoms tend to be relatively mild, hand, foot, and mouth disease can make babies and toddlers (and their caregivers) pretty miserable. Here’s everything you need to know, including how to prevent it in your little one (and yourself!).
Hand, foot, and mouth disease is a type of viral infection, explains Sarah Kohl, MD, a clinical assistant professor of pediatrics at the University of Pittsburgh School of Medicine. The funny-sounding name is derived from the telltale rash that generally appears on the hands, feet and mouth (as well as blisters surfacing in the mouth) of those infected. The virus usually manifests with a high fever that may spike before the outbreak of the rash.
Hand, foot, and mouth disease is typically caused by the Coxsackie virus—usually, but not always, the Coxsackie 1 virus. It’s most commonly seen in babies and kids younger than 5, because they haven’t been previously exposed to the virus and haven’t developed an immunity to it yet. But older children and adults can also contract hand, foot, and mouth disease—even if they’ve had it before. That’s because the illness can be caused by several different viruses and even different strains of the Coxsackie virus, says Bande Virgil, MD, a pediatrician in Columbus, Georgia. So while you become immune to the specific virus that caused the illness the first time around, you’re still susceptible to other strains.
How contagious is hand, foot, and mouth disease?
Very! “These viruses spread quite easily,” says Jeffrey Kahn, MD, PhD, chief of the division of Pediatric Infectious Disease at Children’s Medical Center in Dallas. It’s generally contracted through contact with feces, saliva or mucus, and while it can surface year-round, hand, foot, and mouth disease tends to cluster in the summer and fall, according to Jonathan Auth, MD, a pediatrician at Children’s Hospital of Orange County in California. And because parents may not realize their child is infected at first, it paves the way for the illness to quickly spread through daycare centers and nursery schools.
So when is hand, foot, and mouth disease contagious? Here’s the tricky thing: It’s often contagious before any clear signs of the illness are present. “Because the virus can be shed by people without symptoms, it can be impossible to completely avoid exposure,” Kohl says.
While an official diagnosis can be made via a mouth swab or stool sample, pediatricians often simply make a determination based on the symptoms of hand, foot, and mouth disease, says Adam Spanier, MD, a pediatrician in Silver Spring, Maryland, who works in the Office of Vaccines at the Food and Drug Administration (FDA)—which is why it’s important to call your pediatrician if you suspect your child may have the illness.
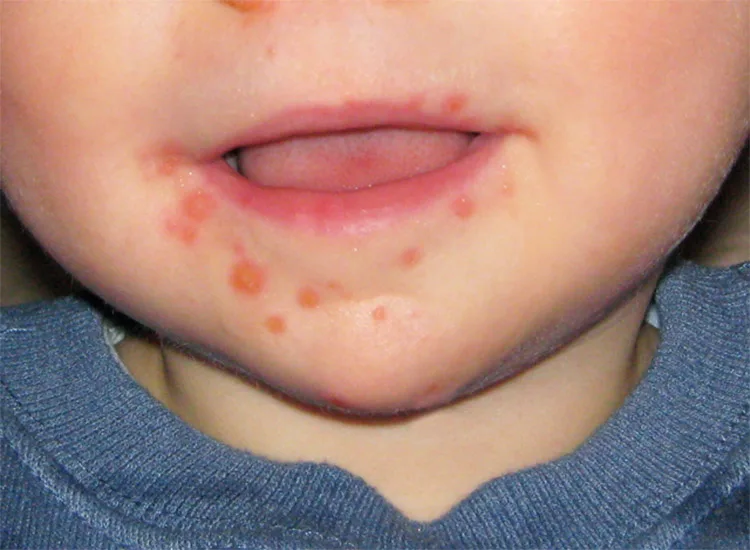
The telltale sign is the red rash, but you can’t always rely on it as an indicator. Sometimes, the rash can be quite subtle, Virgil says, or you may not see the rash before you notice a fever. You also may not spot a rash at all, since it can take the form of ulcers hidden inside your child’s mouth or throat.
Here, some symptoms of hand, foot, and mouth disease to look for:
• Fever. A high temperature is usually the first sign of the virus, which may or may not be accompanied by a rash, says Auth.
• Rash. Red spots may appear on the palms of the hands, soles of the feet and around the mouth, as well as on the knees, elbows, torso, buttocks and genital areas.
• Discomfort. Your child may seem a lot more irritable or uncomfortable than usual, even if they don’t have a rash or a temperature.
• Lack of appetite. If your child seems especially picky about their food, isn’t eating or doesn’t want to drink, it could be a sign that blisters are bothering them, says Spanier. An increase in drooling is also often a telltale sign.
• Sore throat. If your little one complains of a “sore throat,” blisters in their throat could actually be the real culprits.
Pregnant people who have been exposed to the illness and experience any of these symptoms should let their obstetrician know right away. “Fever in pregnancy can be harmful to a fetus, especially in the first trimester,” Virgil notes.
“While there’s no medical cure or treatment for hand, foot, and mouth disease, your pediatrician can help you come up with ways to make your child more comfortable while the illness runs its course,” Auth says. Here, some home remedies for hand, foot, and mouth disease to try.
• Over-the-counter pain relief. Ask your pediatrician about appropriate pain medications, such as ibuprofen (Motrin or Advil) or acetaminophen (Tylenol), and follow the dosage procedures for your child’s age. Taking them half an hour before mealtime can make eating and drinking less painful, Spanier says. Experts also recommend OTC pain relievers to help bring down a fever. Let your pediatrician know if your child’s temperature remains high after taking a pain reliever.
• Plenty of liquids. Make sure your child is hydrating, either with breast milk or formula, or, if they’re older, with water, Auth says. Keep track of urine output: If your child has less than three wet diapers during their waking day or, if toilet trained, goes to the toilet less than three times, call your pediatrician. “Another way to ensure your child is hydrated is to make sure he’s producing wet tears,” Spanier says. ‘If he’s crying without tears, it’s a sign he may be dehydrated and needs to be seen by a pediatrician ASAP.”
• Cold or soft foods. Bring on the ice pops! Foods that are cooling and easy to eat will help soothe a sore throat and painful mouth. Try making breast milk ice pops for baby, and pudding, applesauce, chilled soups or smoothies for an older child.
• Cover mouth blisters. “Many parents I’ve worked with use a combination of Maalox and Benadryl, then use a Q-tip to cover mouth sores with the mixture,” Kohl says. This can help soothe irritation and make it easier for babies and toddlers to drink; but just as with OTC pain relief, ask your pediatrician first before you try this remedy.
• Rest. Your child is likely to feel cranky, especially if they have a temperature or are in pain, so plenty of snuggles and cuddles on the couch are a good hand, foot, and mouth disease treatment.
The good news: By the time your child’s fever resolves, they may be back to their usual playful self, especially if the blisters are mild. The bad news: If they still have lesions, they may not be welcome back in daycare just yet. “Children are usually considered contagious until the lesions resolve, which may take five to seven days out of daycare or preschool,” Virgil says.
Following a bout of hand, foot, and mouth disease, peeling nails (and skin on the hands and feet) can sometimes happen, even a few days or even weeks after the illness has run its course. “A lot of parents see this and panic,” Spanier says. “Even though it’s weird, it’s just another effect of the virus and nothing to worry about.” Keep hands and feet clean and moisturized—the nails will grow back and look like normal in a few months.
No matter how hygiene-focused you are, hand, foot, and mouth disease can be tough to avoid, particularly if your little one is in daycare, preschool or engages in organized activities with other babies or toddlers. Still, there are some things you can do to help prevent it.
• Wipe down surfaces. Make sure all toys and surfaces are wiped down after playtime, washed and disinfected, Kohl says.
• Talk hygiene with your daycare. It sounds gross, but hand, foot, and mouth disease is often spread by fecal matter, usually because someone didn’t embrace proper hygiene habits. Make sure your daycare center is using disposable gloves and has protocols in place to sanitize hands and changing areas from one child to the next.
• Follow your doctor’s guidelines. While it can be tempting to send your child back to school as soon as they seem better, experts say it’s crucial to make sure they’re past the contagious period to avoid passing the illness onto others.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Jonathan Auth, MD, is a pediatrician at Children’s Hospital of Orange County in California. He earned his medical degree from the University of Southern California.
Jeffrey Kahn, MD, PhD, chief of the division of Pediatric Infectious Disease at Children’s Medical Center in Dallas. He earned his medical degree from SUNY Health Science Center at Brooklyn College of Medicine.
Sarah Kohl, MD, is a clinical assistant professor of pediatrics at the University of Pittsburgh School of Medicine. She earned her medical degree from Thomas Jefferson University.
Adam Spanier, MD, is a pediatrician in Silver Spring, Maryland, who works in the Office of Vaccines at the Food and Drug Administration (FDA). He earned his medical degree from Louisiana State University School of Medicine.
Bande Virgil, MD, is a pediatrician in Columbus, Georgia. She earned her medical degree from the Morehouse School of Medicine, where she also completed her pediatric residency.
Learn how we ensure the accuracy of our content through our editorial and medical review process.
Navigate forward to interact with the calendar and select a date. Press the question mark key to get the keyboard shortcuts for changing dates.