It's Not Just Your Family: CDC Reports a Spike in Strep Throat Cases
As Spring blossoms into full swing, you might be surprised to discover Strep throat, usually, a staple of winter, has cropped up around your house, daycare and school. The highly contagious bacterial infection caused by Group A streptococcus bacteria is being reported in record numbers, with many medical professionals claiming that numbers may be higher than we realize as the infection continues to present with uncommon symptoms. Learn what you need to know about the recent spike and how to protect your kids here.
How do we know cases are rising?
Earlier this month, the US Centers for Disease Control (CDC) issued a statement warning about the recent increase in invasive group A strep (iGAS) infections among children after two children died last fall.
Dr. James Versalovic, the pathologist-in-chief at Texas Children’s Hospital in Houston —one of the largest pediatric hospitals in the US—told NBC News that he has seen “a greater than fourfold increase” in potentially invasive infections in the last two months compared to the same period last year. While this may sound alarming, cases of iGAS are somewhat rare, with Texas Children’s reporting around 60 cases over October and November.
Outside of the more rare iGAS cases “minor” group A strep cases, the one’s you are most likely used to seeing around the house, are also reportedly peaking at hospitals across the nation.
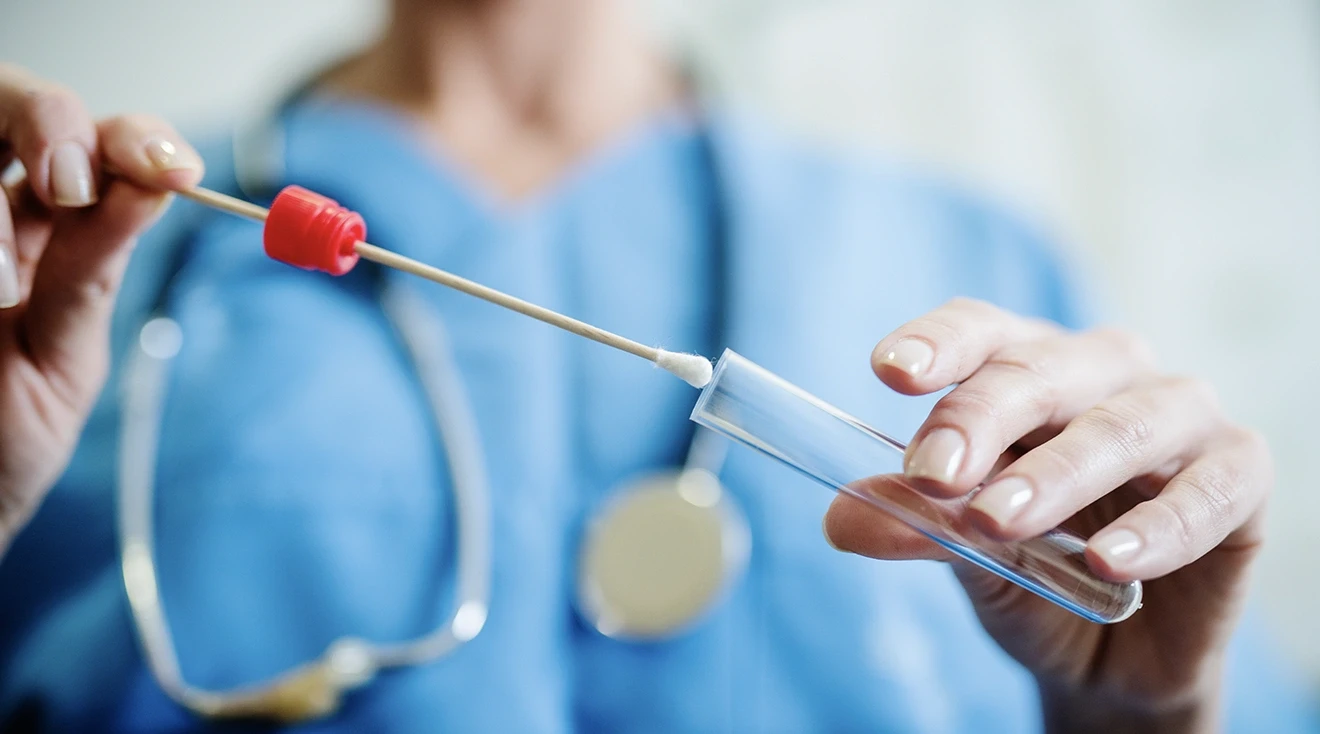
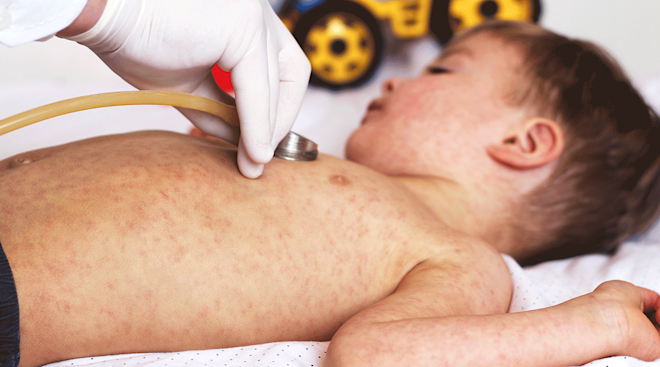
What does group A strep look like?
According to the CDC, bacteria called group A Streptococcus (group A strep) can cause many different infections. These infections range from minor strep illnesses to more serious and life-threatening diseases.
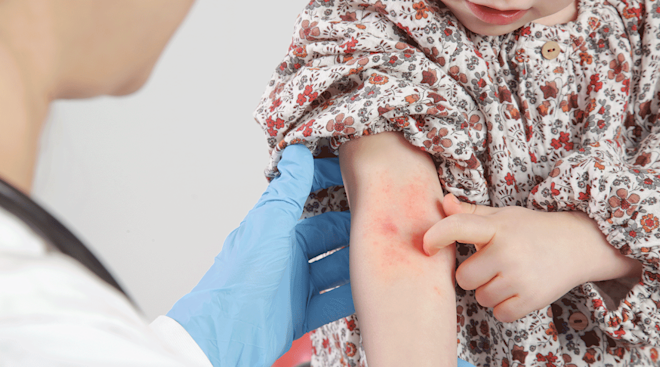
While we all know the token sore throat and fever that strep is known for, medical professionals across the United States have recently reported an uptick in the infection presenting in less common ways. A viral TikTok from Wisconsin-based pediatric nurse practitioner Dakota Felckowski discusses how strep has been showing up lately.
“The symptoms are not typical strep symptoms,” Felckowski says in her TikTok. “Typically, we see headache, sore throat, fever, stomachache, and vomiting, especially in kids with strep throat. These may or may not be happening right now, but more frequently we are seeing congestion, runny nose, cough which are not typically strep infections which makes it really tricky to diagnose and treat,” she notes.
Felckowski encourages those who might suspect they have been exposed to strep to go see their doctor. “Even if you aren’t showing any symptoms, especially those little kids, they don’t often show the symptoms, you might want to go to the doctor to get tested. Also, if you’ve had an infection that’s just lingering and we thought it was viral, you might want to have your doctor check you out and consider strep as an infection you are dealing with.”
As previously mentioned, iGAS is a far cry from your everyday strep and occurs when bacteria spread to areas of the body that are normally germ-free, such as the bloodstream. If contracted though, invasive group A strep can lead to trigger serious problems like lower airway infections such as pneumonia or empyema; skin infections like cellulitis or necrotizing fasciitis; or streptococcal toxic shock syndrome, an immune reaction that can lead to organ failure.
What should I do to protect my child?
The CDC recommends that parents take the following three routes of action and prevention.
- Learn about and look out for the symptoms of necrotizing fasciitis and streptococcal toxic shock syndrome—two of the more serious and life-threatening results of iGAS.
- Seek medical care quickly if you believe your child may have one of these infections.
- Make sure your children are up to date with flu and chickenpox vaccines, since contracting these infections can increase risk of getting an iGAS infection.
If you notice your child is unusually tired or exhibiting symptoms that are longer or more severe than the usual cold or flu symptoms, don’t hesitate to consult your pediatrician. Many offices today have help and sick lines where you can chat with a nurse or medical provider about your child’s symptoms so you can decide if a visit is needed.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Navigate forward to interact with the calendar and select a date. Press the question mark key to get the keyboard shortcuts for changing dates.