How to Spot Fifth Disease in Babies and Big Kids
A case of the sniffles and sore throat is pretty run-of-the-mill for kids—but while these mild symptoms may not send up a red flag, they can actually be early signs of a viral infection known as fifth disease. Colloquially called “slapped cheek” (named for the facial rash that accompanies it), the virus usually isn’t cause for concern—in healthy children, it rarely leads to severe symptoms or problems. But for pregnant women and other vulnerable patients, it can be a different story. Read on to learn what causes fifth disease, how to spot it and how to go about effectively treating it.
Fifth disease is a mild to moderately contagious infection caused by a virus called parvovirus B19. Wondering how it got its unique name? “In the 1900s, physicians defined rashes by numbers,” explains Dennis L. Murray, MD, FAAP, FIDSA, a pediatric infectious disease specialist in Georgia. “First disease was measles, and fifth disease is the only one whose numerical name survived.”
Babies and toddlers with fifth disease develop cold or flu-like symptoms, as well as a rash on their cheeks, arms and legs. It’s most prevalent among school-age children, especially during the winter and spring. “This particular virus is very common throughout the world. It’s there. You can’t escape it,” says Chadi El Saleeby, MD, a pediatric infectious disease specialist at MassGeneral Hospital for Children in Boston. “For school-age kids, around 25 to 50 percent will encounter the virus. By the time someone reaches adulthood, up to 80 percent of adults have been exposed to fifth disease.”
The infection almost never causes serious problems in healthy children, but it can be dangerous for pregnant women and those with preexisting health issues, including HIV, hemolytic anemia and sickle cell anemia.
Can babies get fifth disease?
Fifth disease in babies is relatively rare but does occasionally occur. “Think of it like a curve,” El Saleeby says. “As you get older, you start becoming exposed to viruses, and the older you get, the higher the chances are that you’ve seen the virus before.” In most cases, infants catch fith disease from an older sibling who picked up the virus in childcare or school.
Fifth disease—which is a contagious infection—can be transmitted in one of three ways:
1. By interacting with someone who’s infected. “The most common way is respiratory transmission,” El Saleeby says. “It means somebody is sick with the virus, and through either coughing or person-to-person contact the virus can get transmitted to another person, usually via the respiratory route.”
2. By touching a contaminated surface. Fifth disease can also be passed along if someone coughs or sneezes onto a surface that another person then touches, and the virus works its way into their respiratory system. “The virus is fairly stable in the environment, so it doesn’t die quickly on surfaces like pens, doorknobs and kitchen utensils,” El Saleeby says.
3. By passing the virus onto baby during pregnancy. This is what’s called vertical transmission, where a pregnant mom becomes infected with fifth disease and transmits the virus to her fetus. At least 50 percent of moms-to-be have already had the infection pre-pregnancy and therefore have antibodies that ward off fifth disease, El Saleeby says. But if the virus is passed to baby within the first half of the pregnancy, it can potentially lead to miscarriage—but it’s rare, only occurring in less than 5 percent of women.
Fifth disease isn’t often considered perilous, but tragedy does strike. Mary C. of West Orange, New Jersey, suffered a miscarriage when she was 15 weeks pregnant after contracting fifth disease from her 3-year-old son, who caught it at his preschool. “Awareness of fifth disease is low, and we believe the death of our daughter could have potentially been prevented,” she says. “Fifth disease was going around the school, but we didn’t receive a notification about this very contagious illness. We knew nothing about fifth disease prior, but it affects about 5 percent of pregnancies. One death is one too many.” Now Mary is urging her son’s school to adopt a health policy and teacher training around health issues to prevent this from happening to other families.
“In essence, fifth disease is a very mild viral infection that starts out looking like a cold,” Murray says. Fifth disease symptoms typically set in four to 14 days after the virus enters the body and then progress. Throughout the course of the illness, common symptoms include:
- Fatigue
- Sore throat
- Running nose
- Headache
- Fever
- “Slapped cheek” rash
- Rash on body
- Itching
- Upset stomach
- Nausea
- Vomiting
- Diarrhea
- Swelling and stiffness of joints (more common in adults)
Early fifth disease symptoms can include fatigue, runny nose, sore throat, headache, fever and achy muscles. With such mild symptoms, it can be hard to know that your child has the virus—in fact, 20 percent of kids won’t have any symptoms at all before the telltale rash appears. “I’ve seen kids with fifth disease running around just fine,” Murray says. Unfortunately, this is also the time when they’re most contagious.
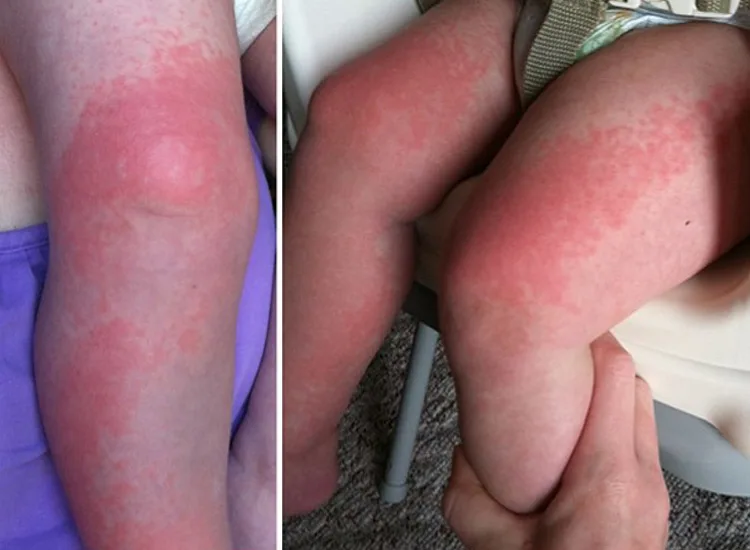
After about seven to 10 days, a red rash may appear on the child’s face, almost as if they had been slapped (hence fifth disease’s nickname, “slapped cheek”). A few days later, a second, itchy rash can crop up on the child’s chest, back, butt, arms or legs. “It looks like a lacy pattern, and it can be a little darker than red on the shoulders,” Murray says. “When that rash goes away, the illness is over,” Murray says.
While a blood test can confirm whether a patient has fifth disease, in most cases a doctor can make the diagnosis without one based on indicative fifth disease symptoms.
In typical cases, fifth disease in healthy patients can last anywhere from four days to a couple of weeks, according to Murray. The classic “slapped cheek’ rash can stick around for a few days, followed by a body rash that varies in intensity. It usually goes away within 10 days, but it can briefly reappear over the next several weeks, especially when your child is taking a bath, running around or out in the sun.
The good news? Patients aren’t contagious the entire time they’re sick. Kids can transmit fifth disease to others before the onset of a rash, but once your child develops the rash, they’re no longer infectious—although the fever can still be quite high (up to 104 degrees Fahrenheit) for several days after.
Since the viral infection will eventually clear up on its own, the standard fifth disease treatment is aimed at easing any uncomfortable symptoms. If your child has a fever, you can give them acetaminophen (Children’s Tylenol). “To avoid dehydration, make sure your child gets plenty of fluids,” Murray says. “See the doctor if the fever doesn’t go away.”
The fifth disease treatment plan differs for high-risk cases. Babies one to 2 months of age with a fever should be brought to the hospital for treatment. Expectant moms-to-be—especially those in the first 21 weeks of pregnancy—should get tested immediately if they suspect they have the virus and discuss fifth disease treatment with their doctor right away, since in rare cases the illness can lead to fetal anemia or even miscarriage. Fifth disease can also be dangerous for people with an immunodeficiency, such as HIV or cancer patients, and their doctors can determine the best course of treatment.
“Unfortunately, there’s no vaccine that can prevent fifth disease,” El Saleeby says. But there are still a few things you can do to reduce the chances of infection. “You can help prevent it by avoiding sick children, especially kids in elementary school, who are the most symptomatic with this infection,” he says.
Aside from avoiding close contact with those who are sick, the key to fifth disease prevention is practicing good hygiene: Wash your hands regularly, cover your mouth with your sleeve or elbow when you cough or sneeze, and don’t touch your eyes, mouth or nose.
Updated February 2020
Expert bios:
Dennis L. Murray, MD, FAAP, FIDSA, is a pediatric infectious disease specialist in Augusta, Georgia. He received his medical degree from University of Michigan Medical School and has been in practice for more than 20 years.
Chadi El Saleeby, MD, is a pediatric infectious disease specialist at MassGeneral Hospital for Children in Boston and an assistant professor of pediatrics at Harvard Medical School.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Navigate forward to interact with the calendar and select a date. Press the question mark key to get the keyboard shortcuts for changing dates.