7 Ways Your Prenatal Care Might Change Due to COVID-19
The coronavirus pandemic has upended life as we knew it, affecting everything from our jobs to our social interactions and, yes, how moms-to-be receive prenatal care. But the extent to which COVID-19 has impacted the way doctors care for their pregnant patients varies, depending on the individual care provider, the pregnancy and the geographic area. Some experts say the outbreak has significantly altered the delivery of prenatal care, while others say it’s resulted in minor changes. Either way, one thing is for sure—that baby is still coming, and you still need the best care possible. “The show must go on, we say in obstetrics,” says Heather Bartos, MD, an ob-gyn based in Cross Roads, Texas. Here, we’ve listed out several ways in which your prenatal care might look a little different these days.
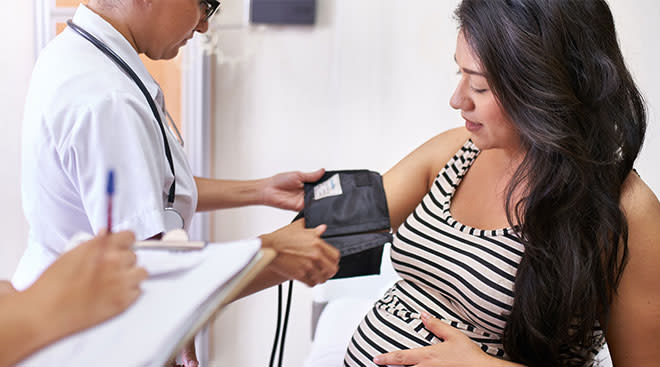
Even if you’re doing your best to spend your days at home, you’ll still need to go see your ob-gyn for in-person visits, especially if any tests (bloodwork, ultrasounds, etc.) are required. When you arrive, though, expect some new rules to apply.
Many practices are discouraging or no longer allowing partners or children to accompany women to their visits in order to minimize people’s potential exposure to the virus. “We had one family that showed up during stay-at-home orders with five kids, grandparents and the spouse!” Bartos says. “That’s too much risk for other patients and ourselves.” Depending on the practice, some may make an exception for partners to be present during ultrasounds, but if not, consider FaceTiming your loved one so they can get a glimpse of the baby.
You’ll also notice that doctors and office staff are wearing masks, and you’re encouraged to do the same, in addition to washing your hands often. It may be a good idea to bring along a bottle of hand sanitizer to use periodically (after opening the door, pressing the elevator button, sitting in the waiting room, etc.). Many offices are intentionally spacing out patient visits to have fewer doctors in the office at once and avoid a crowded waiting room. “When women do come in for a visit, we try to get folks into the exam room as quickly as we can to minimize any time spent in a waiting room,” says Mary Jane Minkin, MD, an ob-gyn at Yale NewHaven Health in New Haven, Connecticut.
You probably didn’t think much about the way you got around town before coronavirus struck, but these days when you’re gearing up for an in-office visit, carefully consider your transportation of choice.
Experts agree that the safest option is to drive your own car, if you have one, so you’re not sharing germs with others. If that’s not feasible, consider using a private car service such as Uber or Lyft, if you can afford it, so you’re in the car with only one other person. In the case that you use public or semi-public transportation, use a disinfectant to wipe down any surfaces you may touch, like railings or arm rests, and use hand sanitizer once you get settled and again after you exit. The CDC encourages everyone to wear a cloth face mask when out in public.
“If women don’t have cars and don’t have a ready way of getting to an office, it may be more appropriate to see if their provider can do a telehealth visit,” Minkin says.
“We’re trying to eliminate unnecessary visits,” Minkin says. The standard schedule of prenatal appointments is once a month through 28 weeks of pregnancy, then every two weeks until 36 weeks and then weekly until birth. While doctors are still scheduling sonograms at their normal intervals and conducting bloodwork and fetal wellbeing tests (like non stress tests) in office, if no tests are needed for certain appointments and your pregnancy is progressing well, “you can discuss with your provider to see if you can space things out a bit,” Minkin explains. “We’re also trying to put some visits together—like if a woman needs her blood glucose test at 28 weeks, we will try to combine that with her regular visit so she has to go out one less time.”
There will be instances when it’s necessary to see your doctor in person, but there may be other times when a virtual visit—conducted remotely through video conferencing—is preferable, to keep you home and minimize your exposure.
“The questions we usually ask—How is the baby’s movement? How are you feeling mood-wise?—are quite answerable via telehealth,” Minkin explains. Some women have even stocked up on certain medical supplies, such as home blood pressure cuffs, home fetal heart beat machines and tape measures to assess the size of the uterus, to help care providers conduct more effective check-ups virtually. “We cannot check a cervix or do a culture over the phone, but there is a lot we can do,” she says.
Many ob-gyn offices traditionally offer prenatal classes to help patients prep for labor and delivery. Those in-person group classes are not being held right now, but there are lots of options available online. It also used to be common practice for couples to take a tour of their chosen hospital maternity ward to familiarize themselves with the layout and hospital policies. Instead, “our hospital has started doing virtual tours of the hospital and labor floors to show the couple what to anticipate at the hospital,” Minkin says. Some ob-gyns, like Bartos, are also hosting weekly webinars on hospital updates, which she says have performed very well.
If you’re close to your due date, ask your doctor what their instructions are for when you go into labor. “For anyone who thinks they are in labor, we’re asking them to come to office first, unless it’s after hours,” Bartos explains, so they can avoid unnecessary trips to the hospital.
Expect certain changes at the hospital once Delivery Day rolls around. One of the biggest differences is that doctors will be wearing protective gear—meaning masks and head-to-toe protection, “which can be a little unnerving for our ladies,” Bartos says.
You may also need to wear a mask and be tested for COVID-19. If you test positive, you may be separated from your newborn for a time in order to keep your little one safe and healthy. “Fortunately, we have turned up very few women who were positive,” Minkin says. “The overarching thing to remember is that hospitals are now quite used to special COVID procedures, like negative pressure rooms and appropriate gowning, so the safety for patients is excellent. And despite anxieties about being closer to some folks with COVID, it’s still much safer to deliver at a hospital than at home!”
Another piece of good news? You may be at the hospital for fewer days than you think. “We’re encouraging our patients to leave as soon as they and baby are able (UK-style) to avoid prolonged exposure,” Bartos expains. “I even have some cesarean sections leaving after 24 hours!” Of course, you’ll be discharged only when you and baby are deemed well enough.
Doctors are now offering telehealth visits not just for prenatal care, but for postpartum check-ups as well. “We are actually doing more of those to check up on women; instead of the usual one to two in-person visits, we’re doing three to four telehealth visits,” Bartos says. “Most of our postpartum patients are loving it—they don’t want to come out of the house at all with a new baby.”
Regardless of any changes you might experience in your prenatal care, trust that your doctor has your and your baby’s best interests in mind and are doing everything they can to minimize your risk while making sure your pregnancy is progressing well. If you have any questions about possible changes to your care or new office or hospital policies, never hesitate to reach out to your provider and discuss what might be best for you and your growing family.
About the experts:
Heather Bartos, MD, FACOG, is an ob-gyn as well as the founder and medical director of Be. Women’s Health and Wellness in Cross Roads, Texas. She is also a certified lactation consultant and pilates instructor.
Mary Jane Minkin, MD, is an ob-gyn at Yale NewHaven Health in New Haven, Connecticut and has been in practice for more than 40 years. She also serves as a clinical professor of obstetrics and gynecology and reproductive sciences at Yale University School of Medicine.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Navigate forward to interact with the calendar and select a date. Press the question mark key to get the keyboard shortcuts for changing dates.