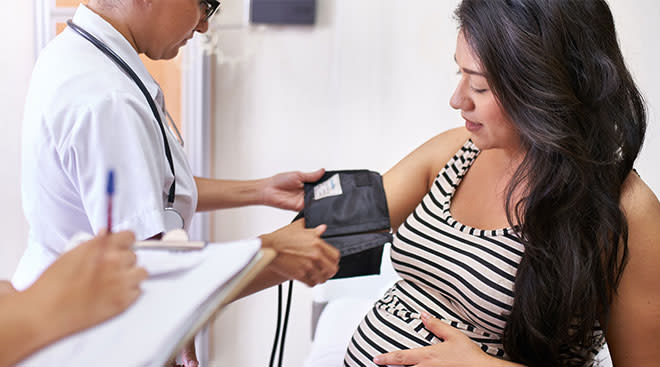
The rapid spread of COVID-19 has pregnant women understandably concerned about their health and that of their developing child. And with the situation changing day to day, it’s no wonder we’re bursting with questions. Here, an ob-gyn tackles the top questions she’s been getting about the novel coronavirus and how to keep women safe during pregnancy.
We currently don’t know, but there are currently no data to suggest that pregnant women are more likely to get COVID-19. However, we do know that pregnant women undergo changes to their immune systems that may make it easier to become infected with any virus, including COVID-19. Additionally, if a pregnant woman does become infected, they may be at higher risk of more serious disease. Therefore, all pregnant women should practice social distancing and frequent, proper hand-washing.
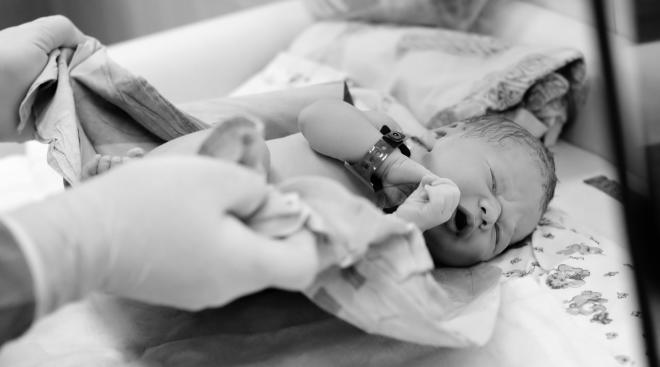
Data on this is mixed and is extremely limited, as we only have small numbers from case reports and case series. A small case series of nine women from China, as well as another study of 38 women from China, all positive for COVID-19, showed that all of the infants born to these women were negative for COVID-19. Testing was performed of the placentas, amniotic fluid, neonatal throat swabs and/or breast milk.
But there have also been recent case reports of newborns screening positive for virus-specific antibodies, suggesting vertical transmission—meaning it may be possible for moms-to-be to pass the virus onto their babies, either through the placenta, direct contact during birth or through breast milk. The newborns in these studies tested negative for COVID-19 through throat swabs; however, the presence of antibodies—in particular IgM, which cannot cross the placenta due to their size—suggest the infants could have been exposed in-utero.
Additional limited data suggests women who are infected with COVID-19 may be at a slightly higher risk of preterm birth, but it’s difficult to determine if the preterm birth was due to infection with COVID-19 or other pregnancy-related complications.
A recent study also notes pregnant women who do contract COVID-19 may pass on protective antibodies to baby.
Again, this data is extremely limited and will likely change as more information about the virus in pregnancy is studied. In the meantime, the most important recommendations pregnant women can follow are to practice social distancing and adequate hand-washing to decrease their risk of infection.
Watch, Hospital Bag Essentials During Covid-19:
Follow local and federal guidelines. Right now, it’s critical that the curve of infected individuals remain flat or else we run the risk of overwhelming the supply of medical equipment for those who may need it.
Individual cities and states all have different guidelines, but right now the CDC and federal government recommend:
- Get vaccinated, especially for pregnant women who are at a high-risk for COVID-19 (As always, speak to your healthcare provider first.)
- Practice social distancing
- Wash your hands with soap and water properly and frequently. If you can’t wash your hands, use hand sanitizer
- Cover your sneeze or cough with your arm or a tissue and throw the tissue away
- If you are sick, stay home and quarantine for at least two weeks!
- Wear a face mask (or two, one cloth mask and one surgical mask) to reduce the risk of spread to others
- Wipe down frequently touched items such as your cell phones, wallets, keys, computers, etc.
- Those who are immunocompromised should stay home and only leave the house for essential needs
You should discuss this with your ob-gyn. Many clinics are changing their policies and trying to do more telemedicine appointments, but this may not be possible for prenatal visits. When you do go to appointments, practice social distancing and wash your hands with soap and water.
Allergies and the common cold may present with itchy or watery eyes and a runny nose or congestion. If you routinely get allergies this time of the season or your symptoms are mild, it’s likely you have a cold or seasonal allergies. Most symptoms are limited to the nasal passages.
Symptoms of COVID-19 and the flu are more systemic and include fever greater than 100.4, chills, sore throat, a cough and overall body aches. COVID-19 may be more likely if you have the above symptoms and you recently traveled, had recent exposure to someone positive for COVD-19 or have shortness of breath.
The CDC now recommends that everyone wear cloth masks out in public, or even a cloth mask and a surgical mask if available. Some governors and mayors from hard-hit areas have also recommended that residents in their local areas wear masks when going outside for essential needs. Remember, though, that masks alone do not protect you from getting the disease. It’s still important to maintain social distancing of at least 6 feet and to only go out in public for essential needs.
It’s likely that all hospitals are developing contingency plans regarding hospital beds and how to handle a possible influx of patients. As you enter into your third trimester, you can discuss with your ob-gyn what changes your delivery hospital may be making over the next few weeks and how this may impact you. If you have other children, I would recommend having a plan in place for childcare in case your hospital is not allowing visitors.
If COVID-19 is active in your community, there will likely be limitations to the visitors and guests allowed in your room and extra measures set-up to screen any individuals coming into the hospital. Some hospitals in affected areas may be banning all visitors or partners in the labor and delivery area or in the postpartum unit. Many of these hospitals may offer the option of video conferencing or extra support staff to help you during your birth and postpartum recovery.
While it’s natural to be anxious, fearful or angry about these guidelines, know they are intended to keep you, your baby, the medical staff and other patients safe. The American College of Obstetricians and Gynecologists (ACOG) and the Society for Maternal Fetal Medicine (SMFM) still recommend that all women give birth in a hospital, hospital-based birth center or an accredited birth center, as it’s the safest place to deliver for both mother and baby.
Continue to follow guidelines put out by local and federal government. Practice social distancing, limit the number of individuals who are around you and your baby and avoid any sick individuals. Newborns are at especially high risk of infections since their immune systems are still developing, so make sure to wash your hands with soap and water (or use hand sanitizer if you’re unable to wash your hands) before picking up your baby. This is a difficult time and everyone wants to share in the joy of a new baby being born, but it’s important to keep you and your newborn safe.
Hospitals have put plans together in preparation for the event that a woman positive for COVID-19 or is considered a person under suspicion (PUI) delivers a newborn. These plans may include temporary room separation of the infected woman and her newborn and also limiting the number of individuals in the delivery room. I would recommend speaking to your ob-gyn and delivery hospital for these details.
Right now, individual hospitals will likely have their own policies set up for who can visit you in the hospital and how many individuals can be with you in the delivery room. All individuals should consider local or federal guidelines and those who are at highest risk of serious illness should avoid any situation in which they may place themselves at greater risk of contracting the illness. I would recommend asking your ob-gyn or delivery hospital about their current policies on visitors and support persons allowed in the delivery room.
The situation is evolving, and updated recommendations and policies are being implemented on an ongoing basis. For continued up-to-date information, be sure to check the CDC’s guidelines on COVID-19.
About the author:
Temeka Zore, MD, is a reproductive endocrinologist and infertility specialist as well as a board-certified ob-gynt currently practicing in Los Angeles at Reproductive Medicine Associates of Southern California. She enjoys taking care of a wide range of reproductive and fertility issues but has a special passion for fertility preservation and educating and empowering women regarding their reproductive health. Follow Zore on Instagram @temekazoremd.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Navigate forward to interact with the calendar and select a date. Press the question mark key to get the keyboard shortcuts for changing dates.