What You Need To Know About RSV in Babies and Infants
Any time baby is sick, a piece of your mama heart breaks a little. Not knowing the cause or the cure makes matters even more worrisome. Is it just a runny nose and cough, or is it something more? That “something more” is sometimes RSV. Here’s what you need to know about RSV in babies, so you can worry less and give your little one the treatments and TLC he needs.
RSV is a common respiratory virus that shares the same symptoms as a bad cold. (What does RSV stand for? That would be respiratory syncytial virus.) RSV season is the same as cold and flu season, spreading its misery from November through March. “The difference with RSV is this particular virus easily spreads and can extend into the lungs,” says Henry Bernstein, MD, professor of pediatrics at Hofstra Northwell School of Medicine in Hempstead, New York. While most adults can clear the virus eventually on their own, RSV in infants can develop into something more serious. Each year in the US, an estimated 57,000 children younger than age 5 are hospitalized because of RSV.
Viruses don’t discriminate, so every baby is at risk for RSV. In fact, the Centers for Disease Control and Prevention (CDC) reports that virtually all children contract RSV by age 2. But babies born earlier than 35 weeks are at a higher risk for a more severe case of RSV because their immune systems and lungs haven’t fully developed yet. The same goes for babies with heart or lung disease. Some of those severe cases can even lead to bronchiolitis, an inflammation of the small airways in the lungs, and pneumonia, a lung infection.
Full-term babies aren’t immune to the severe effects of RSV either. According to the CDC, RSV in infants is the most common form of bronchiolitis and pneumonia in US children under the age of 1. Statistics show that one to two out of every 100 children younger than 6 months who have RSV need to be hospitalized.
If you’re wondering, “Is RSV contagious?” the answer is an emphatic yes. RSV in babies can occur when an infected person merely sneezes or coughs in the direction of baby. Those little virus-containing droplets of saliva emitted into the air then land on baby (and eventually baby’s hands and eyes or mouth). Baby can also get RSV by touching a toy, crib rail or other surface that has the virus, then touching his eyes, nose or mouth before his hands are washed. “RSV is a virus that likes to live on surfaces,” says Paul Checchia, MD, professor of pediatric critical care medicine and cardiology at Texas Children’s Hospital in Houston. “It will live on the table for 24 to 48 hours.” In terms of how long RSV is contagious for, babies and anyone else with RSV can spread the virus over the course of three to eight days.
RSV symptoms usually don’t start to emerge until four to six days after baby is exposed to the virus, and it’s hard to tell a case of RSV in babies from a pesky cold. If you see any of the signs below, your best—and only—course of action is to keep baby comfortable (see RSV Treatment in Infants and Babies):
-
Congested or runny nose
-
Dry cough
-
Low-grade fever
-
Sore throat (signs include redness, loss of appetite and difficulty swallowing or opening wide)
-
Mild headache (which you can sometimes tell by a lack of energy and loss of appetite)
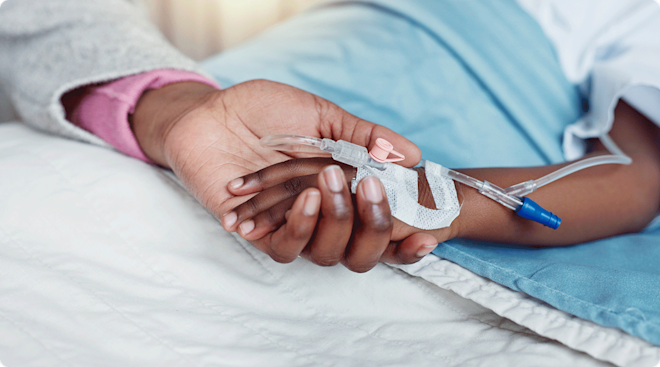
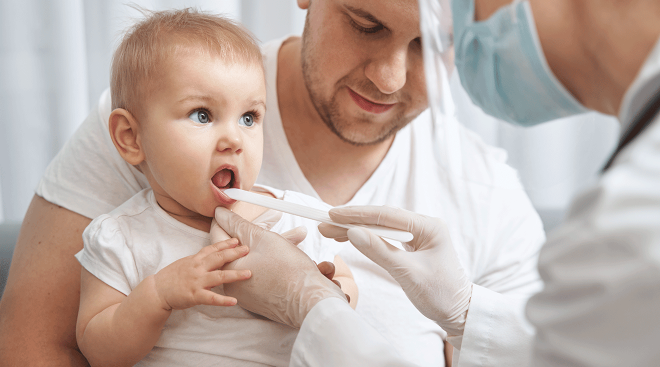
Occasionally, the typical cold-like RSV symptoms in infants can turn into something more serious. In this case, your doctor might use a swab to collect fluid samples from the back of the nose to confirm that it’s RSV. He might also simply look at baby’s symptoms and do a physical exam to make the diagnosis. If the conditions are severe, he might send you to the hospital, where RSV in babies and infants can be treated with humidified oxygen or intravenous fluids. The treatment and recovery time can vary. “The worst of it is usually a seven-day course,” Checchia says. “It’ll peak around day three or four, then start to get better. But it can take two to three weeks to fully recover from it.” That said, it’s crucial to call your doctor as soon as possible if you see these RSV symptoms:
-
Breathing faster than normal
-
Any difficulty breathing
-
Shallow cough
-
Trouble eating
When treating RSV in babies, there’s no magic medicine that can make it go away overnight. “Because it’s a virus, it needs to run its course,” Bernstein says. Until that happens, there are a few RSV treatment strategies that can help make the discomfort of RSV in infants and babies more bearable, including:
-
Give baby plenty of fluids.
-
Help baby blow nose with a nasal aspirator.
-
Use a cool-mist vaporizer during the winter months to keep the air moist (clean it on a regular basis to prevent mold buildup).
Unfortunately, one bout of RSV doesn’t prevent a second one. “A child who gets it in November can still get it in March,” Checchia says. “And having it one year doesn’t protect you from getting it the next year.” Still, a few common-sense precautions can help increase the chances of keeping RSV in babies at bay:
• Keep baby away from people with colds. Obviously.
• Do not share cups and utensils. You never know if you might be harboring the virus without showing symptoms.
• Wash hands before touching baby. Encourage others to do the same. It’s hard to tell if you or anyone else has inadvertently touched something infected with the virus.
• Cover coughs and sneezes. Use a tissue (then wash your hands), or cough and sneeze into your sleeve.
• Keep surfaces clean. Wipe down countertops, tables, doorknobs, toys, bedframes and so on, especially if someone at home is sick.
• Keep hands off face. Avoid touching your eyes, nose and mouth, especially if you haven’t washed your hands.
• No smoking in the house. Smoking will only make RSV symptoms worse.
• Keep sick siblings away. If one child develops RSV, a sibling doesn’t necessarily have to get it too. Although it may be hard, separate them whenever one is sick.
• Avoid crowded areas. That means malls, elevators and other confined spaces where baby could come into contact with sick people. (Perhaps some online shopping during RSV season?)
• Antibody injections. Babies with chronic medical problems who may be at higher risk for developing RSV might be eligible to get an injection of the drug Synagis to prevent RSV. Ask your doctor for details. As of yet, there is no RSV vaccine, which requires a tiny sampling of the virus itself (as opposed to antibodies). “It’s a tricky virus, and [finding a vaccine] is not easy to do,” says Checchia, “but there’s a lot of research being conducted.”
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Target Baby Registry
Free $100+ Value Welcome KitFree $100+ Value Welcome Kit
15% Completion Discount15% Completion Discount
Free 1-Year ReturnsFree 1-Year Returns
20+ Exclusive 20% Off
Deals For Mom & Baby20+ Exclusive 20% Off Deals For Mom & Baby1:1 Concierge With
Baby Gear Specialists1:1 Concierge With Baby Gear Specialists

*Subject to availability and Retailer's terms.
We earn commissions from these links.