What Is SPD in Pregnant Women? Everything to Know About Symphysis Pubis Dysfunction
Pregnancy can come with a host of random aches, pangs and twinges you didn’t see coming. But if you’re having pelvic pain during pregnancy, it could be due to a fairly common condition called symphysis pubis dysfunction, aka SPD. For the record, SPD in pregnancy won’t affect baby at all, but it can make you feel very uncomfortable—particularly as your bump grows.
“Typically this is a condition of the second half of pregnancy, when the mass of the growing uterus starts to strain the supporting ligaments and tendons,” explains Jonathan Schaffir, MD, an ob-gyn at the Ohio State University Wexner Medical Center.
“By the middle of my second trimester or so, my pelvis hurt significantly every single time I shifted in bed, and getting out of bed was pretty excruciating,” says Natalie Gontcharova, senior editor at The Bump and mom of one. “I couldn’t sleep without my pregnancy pillow. Also I did pelvic floor therapy postpartum, which helped with lingering issues, but it would’ve been a good idea to do some physical therapy during pregnancy too. Having a big baby (which I did) is a risk factor for SPD, so I’m not particularly surprised I had these symptoms.”
Whether you’re just starting to experience some pelvic pain or have a confirmed SPD diagnosis, you likely have questions about what’s happening in your body and how to get relief. Ready for answers? From symptoms to treatment of SPD in pregnant women, here’s everything you need to know.
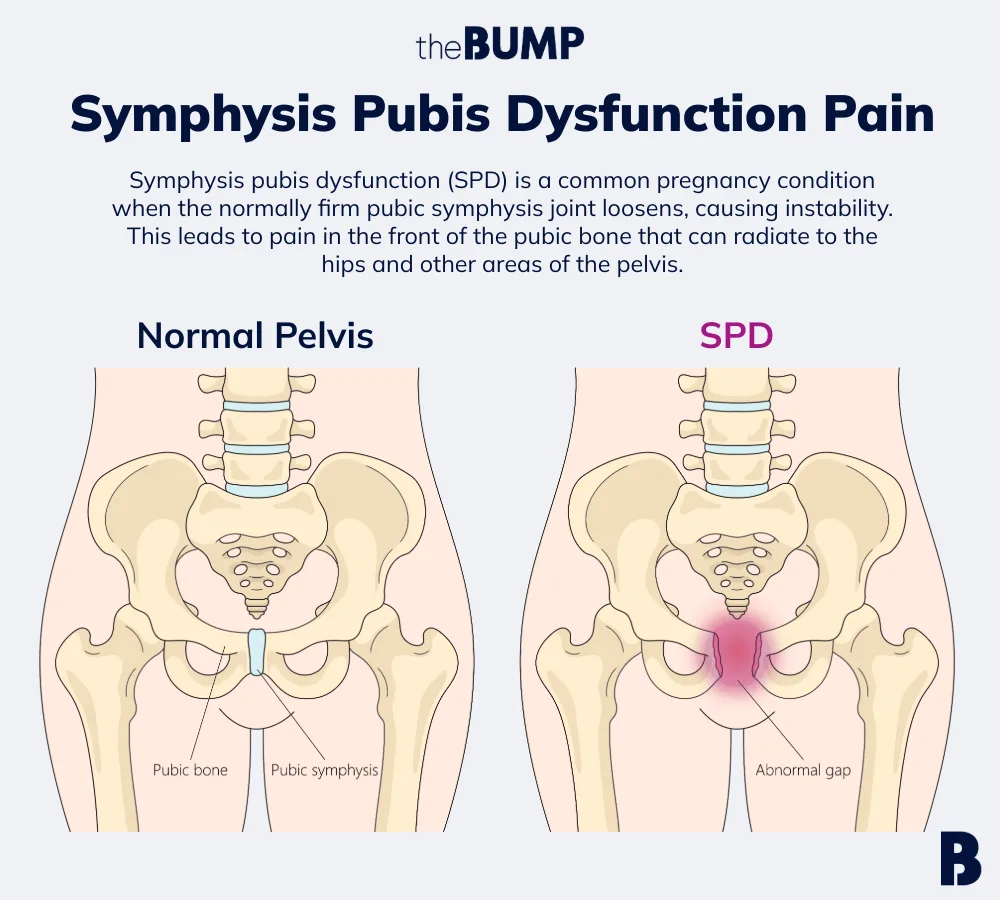
- Symphysis pubis dysfunction (SPD) is a pregnancy condition that causes pain or soreness in the front of the pubic bone that can radiate to the hips and other areas of the pelvis. It often gets worse with certain movements.
- SPD in pregnant women is typically caused by hormonal changes, excessive weight gain or having a large baby. Preexisting injuries or conditions like arthritis can exacerbate the symptoms.
- There’s no specific test you can get for an SPD diagnosis; doctors typically make the determination based on a physical exam and your symptoms.
- While there’s no specific treatment for SPD, you can help alleviate your symptoms with pelvic floor exercises and by avoiding certain movements, such as lunging or sitting with your legs crossed. Your doctor may refer you to a physical therapist for SPD.
- SPD in pregnant women often resolves a few weeks after delivery. However, if the pain persists, make sure to see your healthcare provider. Many moms can benefit from postpartum physical therapy as well.
Symphysis pubis dysfunction (SPD) is a condition that causes pelvic pain in pregnant people. “During pregnancy, the joint between the two pubic bones—the symphysis, which is usually a firmly fixed and immovable joint—starts to loosen a bit in order to prepare for baby to fit through the pelvis,” says Schaffir. “In some women, this loosening creates an instability of the joint that causes strain on the surrounding joints and ligaments of the pelvis.” This can make movement painful; the pain can range from dull and mild to absolutely agonizing.
It’s not entirely clear why some women develop SPD in pregnancy and others don’t. Hormonal changes during pregnancy, particularly an increase in the hormone relaxin, can cause your ligaments and joints to stretch more easily, putting strain on your pelvis, notes Cleveland Clinic. There are a few factors that may raise your risk of developing the condition, says Julie Lamppa, APRN, CNM, the director of midwifery services at Mayo Clinic in Rochester, Minnesota. These include:
- Excessive weight gain in pregnancy
- Twin or multiples pregnancy
- Having a large baby
- A history of SPD in a previous pregnancy
Additionally, if you have a pre-existing injury to your pelvic bones or pain from conditions like arthritis, the risk of getting SPD is higher, Schaffir says.
SPD in pregnant women typically starts during the third trimester, as your growing uterus begins to strain your pelvis more, says Christine Greves, MD, FACOG, an ob-gyn at the Orlando Health Women’s Institute. But it’s possible for it to start earlier too: “The hormone that may loosen the symphysis pubis joint is secreted early in pregnancy, so earlier symptoms are possible,” says Schaffir.
Some sporadic pangs are par for the course in any pregnancy. But SPD in pregnant women is different from feeling the occasional sharp pain in your groin or hip pain when you stretch out your pelvis, Schaffir says. While it’s not common, some women with SPD will have “instability to the degree that it causes severe pain or interferes with normal activity.”
According to Lamppa, SPD symptoms usually include “pain or tenderness felt in the front of the pubic bone that can also radiate to the hips and other areas of the pelvis.” It usually gets worse with certain movements and can “come on suddenly and be excruciating,” during specific activities, like climbing the stairs. “Getting in and out of the car or bed nearly drops me to my knees,” says The Bump community member Macchiato.
I've dubbed my SPD ‘vagina pain’! Sometimes the pain is so severe, especially at night after being in bed for a while, that when I get up I've literally crumpled to the ground. I mentioned it to my doctor and she brushed it off saying it's normal, the baby is pressing down there, my ligaments are loosening up, blah blah. All I know is that it feels like someone took a running jump kick straight to my groin!
You may want a definitive answer or explanation, but there’s no specific test you can have to get a confirmed SPD diagnosis. “Typically, SPD is diagnosed based on symptoms and physical exam alone,” Lamppa says. Imaging can be done to look at your joints, but this is generally not recommended during pregnancy and will usually be put off until after delivery (if the pain lingers).
There isn’t a specific medical treatment for SPD in pregnant women. However, there are a few different options you can try at home to get some relief from pelvic girdle pain. Talk to your doctor about your options; either way, your SPD treatment plan may include:
Symphysis pubis dysfunction exercises
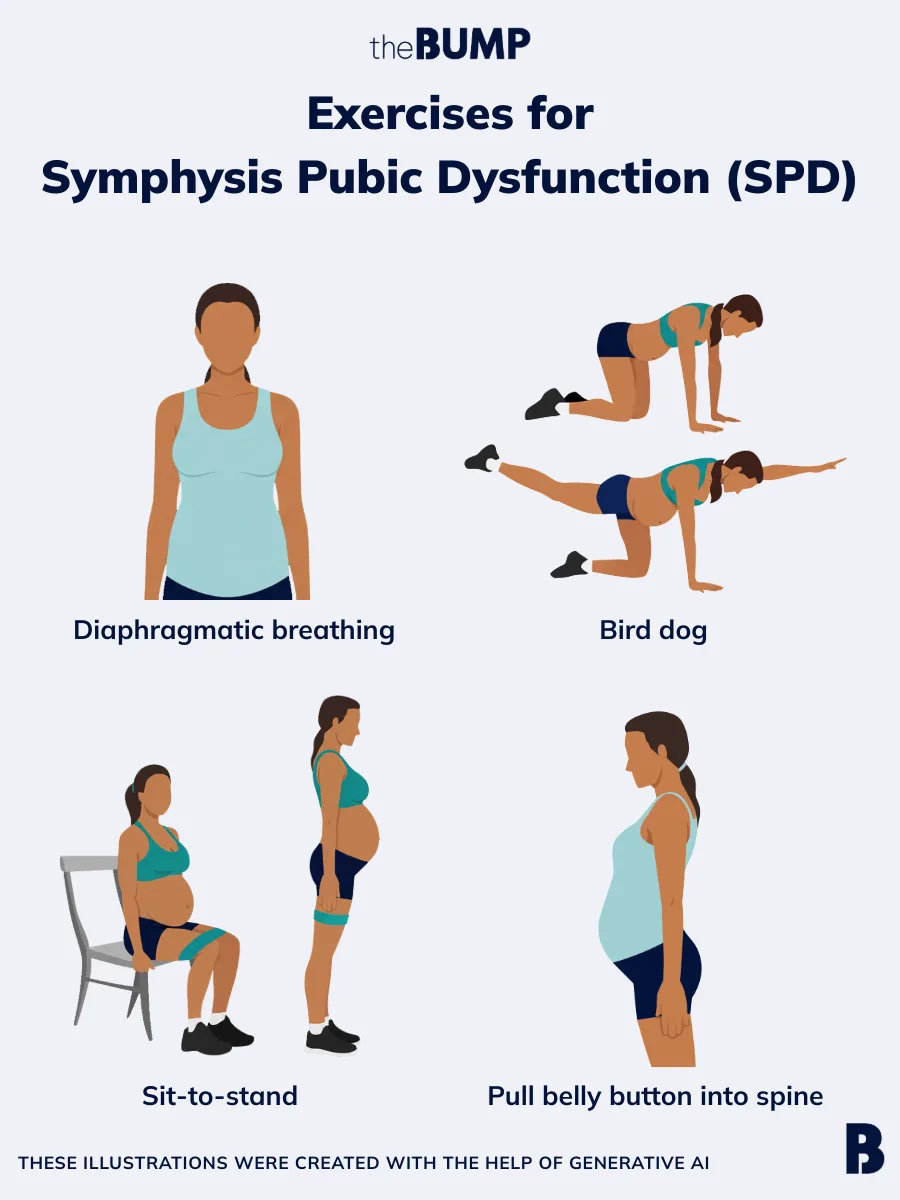
If you’re struggling with SPD pain, your doctor may refer you to a physical therapist. “Physical therapy may be helpful to prescribe exercises that strengthen the muscles and ligaments of the pelvis, which improve stability of the joint,” Schaffir says. Symphysis pubis dysfunction exercises and stretches may include:
- Diaphragmatic breathing, which “allows the pelvic floor muscles to relax and stretch in order to reduce tension and pain,” says Kristin Sapienza, PT, DPT, a physical therapist and the founder of FemFirstHealth in New York City. Inhale through your nose and let the air expand into your ribs and abdomen. Then, exhale through your mouth and feel your ribs and abdomen deflate and return to their resting position. You can do this sitting, standing or reclining.
- Pulling your belly button into your spine, holding it for a few seconds and then releasing (and then repeating several times). You can do this sitting or standing.
- Doing “bird dogs,” which involve getting on your hands and knees and alternating raising your opposite arm and leg while pulling your belly button into your spine
- Doing sit-to-stand exercises with a resistance band around your mid-thighs: Sit on the edge of a chair with feet flat on the floor and back straight, and shift your weight to your feet, gently squeezing your gluteal muscles as you exhale. Sit back down slowly and with control. Sapienza says this can help improve hip stability, which in turn helps support the pelvis.
SPD movements to avoid
To help with your SPD symptoms, Lamppa recommends focusing on your movements and activities: “You want to keep your pelvis stable by taking shorter strides when walking, keeping your legs side by side when getting out of the car or bed and keeping legs together when rolling over in bed.” She also suggests avoiding certain exercises and positions: Lunging and sitting with your legs crossed can exacerbate any discomfort. Sapienza cautions that “single-leg activities” like putting on pants, underwear or shoes while standing can cause pain. She suggests sitting for these activities instead—it can make a big difference.
SPD medication
There’s no universally prescribed medication for SPD. Acetaminophen is generally considered a safe pain reliever during pregnancy, but it “may not be extremely helpful with SPD pain,” Lamppa says. Instead of medication, experts recommend focusing on the exercises above, avoiding certain movements and other at-home support.
Pelvic support belts for SPD
A pelvic support belt for SPD can be helpful. “They help to compress the symphysis joint, holding the bones of the pelvic girdle together, and add stability during movement,” Schaffir explains. It probably won’t eliminate your pain entirely, but it can minimize it. (Check out our list of best pregnancy belly bands, tested by pregnant moms.)
Other at-home support for SPD
Cleveland Clinic suggests that wearing comfortable shoes, sitting and standing with good posture, sleeping with a pillow between your knees—as well as treatments like prenatal massage and acupuncture—can help with SPD. Schaffir also recommends using a heating pad on your lower back. (Just make sure the pad isn’t too hot, and don’t use it for an extended period of time.)
It may take a few weeks after you deliver for your SPD pain to go away. “The relaxation of the joint should improve soon after delivery, but, as with many pregnancy-related changes, it may take six weeks for the symptoms to resolve,” Schaffir explains. If you’re still uncomfortable after giving birth, he recommends continuing to wear a support belt and resting on your side in bed. At that point, you can probably also take non-steroidal anti-inflammatory medications like ibuprofen, Lamppa says. And if your pain continues to be severe, talk to your doctor. It may be time to do an imaging test to see what’s going on in there.
Sapienza adds that you can see a pelvic floor physical therapist postpartum—not just during pregnancy—to address SPD symptoms. “Some patients greatly benefit from internal pelvic floor physical therapy to help address the pain,” she says.
Frequently Asked Questions
Is symphysis pubis dysfunction normal during pregnancy?
One in four pregnant people experience SPD or pelvic girdle pain in general, according to Cleveland Clinic. Since there’s no specific diagnostic test for SPD in pregnant women, it’s tough to say exactly how common SPD is. But it’s safe to say that some type of pelvic pain in pregnancy is fairly common—which is no surprise given all the hormonal changes and your growing bump.
That said, Schaffir says that while some discomfort is normal, “having pain to the point of being dysfunctional” is pretty uncommon. Make sure to see your healthcare provider if you have concerns.
What does symphysis pubis dysfunction feel like?
Schaffir says SPD in pregnant women involves pain that’s centered on the joint at the front of the pelvis, which may radiate to the hips, lower back and legs. Greves says that SPD can feel like “a sharp or shooting pain, sometimes a clicking noise and just overall discomfort.” Experts note that the pain may get worse with certain movements (such as getting out of bed).
How do you sleep with symphysis pubis dysfunction?
Experts and moms say a pregnancy pillow could be your BFF when it comes to trying to sleep with SPD. Sleeping with it between your legs can alleviate some pain at night, says Schaffir. “Trying to keep the legs together when rolling over in bed may help,” he adds.
Can symphysis pubis dysfunction cause early labor?
It’s unlikely that symphysis pubis dysfunction can cause preterm labor. “This situation isn’t associated with early labor,” says Schaffir.
If you have SPD, pregnancy can feel extra uncomfortable. Your best bet is to proactively care for your body and be cautious and careful with abrupt or strenuous activities; try to be mindful of the movements you make and the strides you take. The good news? You’re likely to get relief soon after baby is born. That said, if pain or discomfort persists, make sure to see your healthcare provider.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Christine Greves, MD, FACOG, is an ob-gyn at the Orlando Health Women’s Institute. She received her medical degree from the University of South Florida College of Medicine.
Julie Lamppa, APRN, CNM, is the director of midwifery services at Mayo Clinic in Rochester, Minnesota. She has 15 years of experience as a certified nurse midwife. She’s also the contributor to the Mayo Clinic Guide to a Healthy Pregnancy and co-author of Obstetricks: Mayo Clinic Tips and Tricks to Pregnancy, Birth and More. She earned her degree in nurse-midwifery from the University of Minnesota Medical School in Minneapolis.
Kristin Sapienza, PT, DPT, CMLDT, is a physical therapist and the founder of FemFirstHealth in New York City. She received her Doctor of Physical Therapy degree from the State University of New York at Stony Brook.
Jonathan Schaffir, MD, is an ob-gyn at the Ohio State University Wexner Medical Center. He received his medical degree from Brown University.
Cleveland Clinic, Symphysis Pubis Dysfunction, August 2024
Real-parent perspectives:
- Natalie Gontcharova, senior editor at The Bump and mom of one
- AgentLDub, The Bump community member
- Macchiato, The Bump community member
Learn how we ensure the accuracy of our content through our editorial and medical review process.
Target Baby Registry
Free $100+ Value Welcome KitFree $100+ Value Welcome Kit
15% Completion Discount15% Completion Discount
Free 1-Year ReturnsFree 1-Year Returns
20+ Exclusive 20% Off
Deals For Mom & Baby20+ Exclusive 20% Off Deals For Mom & Baby1:1 Concierge With
Baby Gear Specialists1:1 Concierge With Baby Gear Specialists

*Subject to availability and Retailer's terms.
We earn commissions from these links.