Can You Take Tylenol While Pregnant? The Latest Medical Guidance & Safety Tips
As your pregnancy progresses, you might find yourself in need of relief from symptoms such as headaches or a cold. While many women are hesitant to take medications during pregnancy, Tylenol is generally considered a safe, commonly used go-to for fevers, headaches, and other aches and pains.
Still, with the recent news in which the Trump administration linked Tylenol to autism, you might be asking yourself: Can I take Tylenol during pregnancy? It’s important to remember: Years of research have found no evidence that acetaminophen causes autism, and it remains safe to take Tylenol during pregnancy. “It’s considered safe when used as directed,” confirms Sameena Rahman, MD, an ob-gyn at Northwestern Medicine and founder of GYN & Sexual Medicine Collective.
As a mom of four who’s had complicated pregnancies, I get it. You want what’s best for baby, and even a hint that something may potentially hurt your little one is enough to cause anxiety. But the science is squarely on Tylenol’s side: The small correlations seen in research do not mean Tylenol causes autism. (More on this later!) Plus, as many experts confirm, it’s dangerous to leave a fever in pregnancy untreated.
Still, it’s fair to have questions. Here’s everything you need to know about the safety of taking Tylenol while pregnant, according to the data and doctors.
- There’s no credible link that ties Tylenol use in pregnancy to the development of autism.
- Several major medical organizations recently confirmed that Tylenol use is considered safe during pregnancy.
- Doctors still recommend using the lowest effective dose for the shortest duration possible. Always consult with your healthcare professional before use.
“Acetaminophen is the first-line medication for pain and fever in pregnancy,” reiterates Rahman. The American College of Obstetricians and Gynecologists (ACOG) released a statement after the Trump administration’s announcement confirming that it’s (still) safe to take Tylenol while pregnant.
“Suggestions that acetaminophen use in pregnancy causes autism are not only highly concerning to clinicians, but also irresponsible when considering the harmful and confusing message they send to pregnant patients, including those who may need to rely on this beneficial medicine during pregnancy,” ACOG president Steven J. Fleischman, MD, said in the statement. Fleischman also noted that the claim is “not backed by the full body of scientific evidence and dangerously simplifies the many and complex causes of neurologic challenges in children.”
He also pointed out that the conditions people use Tylenol for during pregnancy are “far more dangerous” than “any theoretical risks.”
The U.S. Food and Drug Administration sent a letter to healthcare providers that took a milder stance than President Trump’s public comments. “While an association between acetaminophen and autism has been described in many studies, a causal relationship has not been established and there are contrary studies in the scientific literature," the letter said.
Some studies have shown that Tylenol correlates with autism. However, if you plot the number of Kennedys alive during the years along with the number of cases of autism in the US, you can see that these two things also correlate. The take-home point is just because something is correlated doesn’t mean it’s causing something.
Yes, Tylenol is considered safe to use during pregnancy. “Acetaminophen use during pregnancy was not associated with children’s risk of autism, ADHD or intellectual disability in sibling control analyses,” according to the latest research on the subject, published in JAMA in 2024. The study analyzed the potential impact of Tylenol use in pregnancy in nearly 2.5 million siblings.
Trump’s announcement appears to be tied to a scientific analysis of 46 studies published in Environmental Health in August that looked at Tylenol use during pregnancy and neurodevelopmental disorders. That study found “strong evidence of an association” between Tylenol use and autism, but the study authors were careful to point out that they found an association—and that the results didn’t mean that acetaminophen causes autism.
Eran Bornstein, MD, director of the center for maternal-fetal medicine at Northwell Lenox Hill Hospital in New York City, cites an analogy that breaks down the difference between correlation and causation: “If we ran a study about what’s going on at the beach in the summer, you’ll see there’s a much higher increase in eating ice cream and also an increase of shark attacks,” he says. “You could say there’s an association between eating ice cream and shark attacks, but eating ice cream doesn’t cause shark attacks.”
Tylenol safety by trimester
Experts agree that Tylenol is considered safe to use across all three trimesters of pregnancy.
First trimester
Tylenol use is considered safe in the first trimester, Rahman says. “In fact, leaving a patient in fever or distress while trying not to take Tylenol is not safe,” she says.
Second and third trimesters
Tylenol is also “safe for most people at standard doses” during the second and third trimesters, says Jamie Alan, PharmD, PhD, an associate professor of pharmacology and toxicology at Michigan State University.
The potential risks and side effects of taking Tylenol during pregnancy are considered the same as when you’re not pregnant, Bornstein says. While there’s no clear link between taking Tylenol and neurodevelopmental delays or complications in baby, there is a risk of liver damage if you take more Tylenol than recommended.
Bornstein stresses the importance of using the medication as recommended. “Like any medication, we want to limit its duration and take it in the smallest dose,” he says. “[But] I wouldn’t hesitate using it if needed.”
Again, when it comes to Tylenol while pregnant, doctors recommend taking the lowest dose necessary and only as needed. There are a few other things to keep in mind.
Dosage and frequency
The maximum dosage of Tylenol for an adult is 4,000 milligrams per 24 hours, according to Cleveland Clinic. Harvard Health notes that if you take it often or are on the smaller side, it’s best to stick to under 3,000 milligrams a day. Always be sure to speak to your healthcare provider about dosing. If you have certain kidney or liver conditions, you may not be able to take as much Tylenol.
Tylenol for pregnancy headaches
Headaches are common in pregnancy, and Bornstein says that Tylenol is considered a safe option for occasional headaches.
Tylenol for fever
Treating a fever is very important in pregnancy, given that uncontrolled fever in pregnancy can cause preeclampsia or even miscarriage, experts say. It’s also linked to neurodevelopmental disorders—such as autism. Tylenol is a recommended way to help lower a fever in pregnancy.
Tylenol for aches, pains and more
Tylenol is also considered a safe medication in pregnancy for aches and pains, Bornstein says. “For those patients who need it, it’s okay to use it,” he says.
Tylenol vs. other medications
While Tylenol is considered safe to use in pregnancy, other common pain relievers, like non-steroidal anti-inflammatory drugs (NSAIDs) including ibuprofen, are advised against. “These should be avoided later in pregnancy, particularly in the third trimester,” Alan says. “These drugs can cause premature closure of the patent ductus arteriosus (PDA), which is an important structure in the developing fetus’ circulatory system.”
Again, if you need Tylenol during pregnancy, it’s considered safe to use it. But if you’d rather try non-pharmacological options first, doctors say these may help provide relief:
- Relaxation and deep breathing techniques
- Gentle exercise
- Acupuncture
- Prenatal massage
- Applying hot or cold packs
- Meditation
- Rest
Frequently Asked Questions
Is it safe to take Tylenol in the first trimester?
Yes, it’s generally considered safe to take Tylenol in the first trimester, according to ACOG and other expert organizations. Be sure to speak with your doctor before taking any medications during pregnancy.
Can I take Tylenol PM while pregnant?
It’s likely okay, but still a good idea to check with your doctor first. “Typically Tylenol PM products contain acetaminophen and diphenhydramine—Benadryl,” Alan says. “This combination is safe for pregnant people. For all combination over-the-counter products, I recommend you check all the ingredients in the product. Ask your healthcare provider if you need extra help.”
Can I take Extra Strength Tylenol while pregnant?
Yes, you can take Extra Strength Tylenol during pregnancy. “This is just acetaminophen at a higher dose,” Alan says. “As long as you take the indicated dose, this is just fine.”
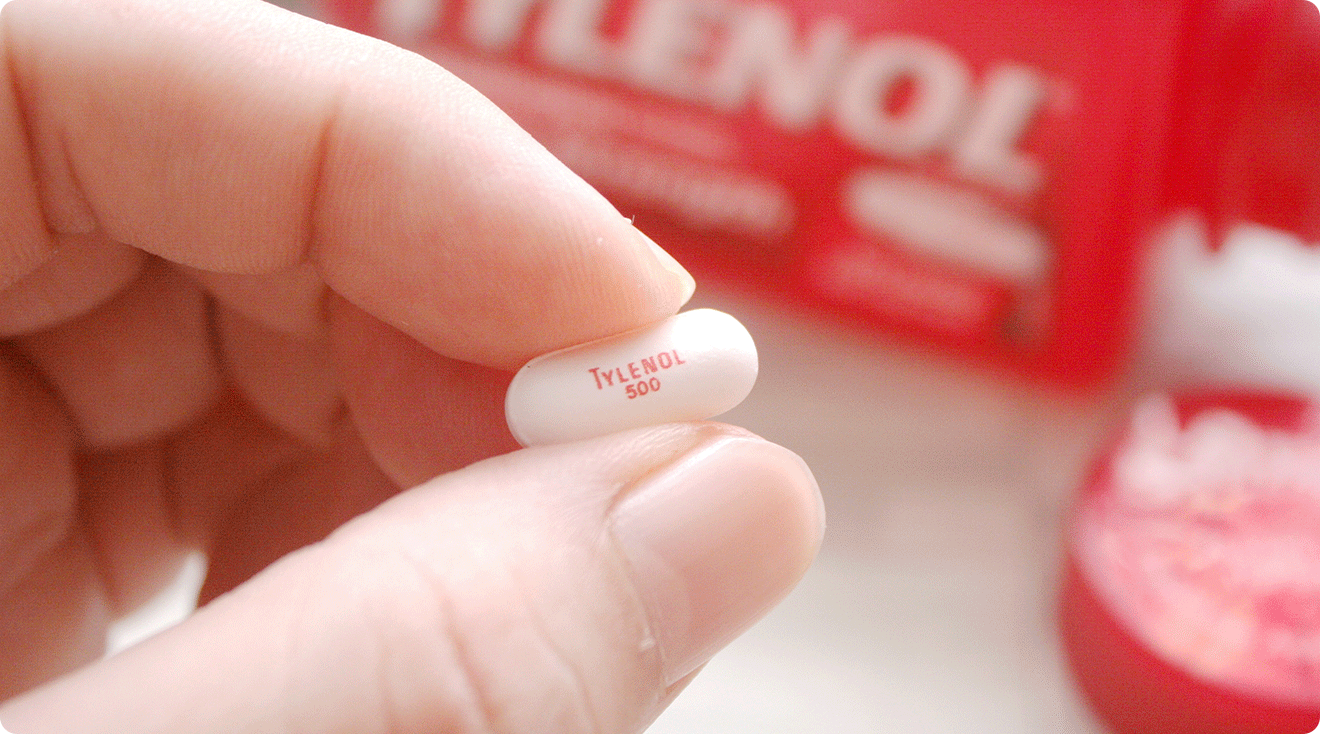
Is 500 mg Tylenol safe during pregnancy?
Yes, as long as you stick to one or two every six to eight hours, as per Harvard Health. This falls within the recommendations of taking a maximum dose of 4,000 milligrams a day.
Can I take 1000 mg of Tylenol while pregnant?
You can take 1,000 milligrams of Tylenol in a day while pregnant.
Can taking too much Tylenol harm baby?
Taking the recommended dose of Tylenol will not harm baby—but a fever during pregnancy can prove dangerous. A truly excessive amount of Tylenol, though, can lead to liver toxicity. Bornstein stresses the importance of sticking to the recommended dose.
Does Tylenol use during pregnancy increase the chance for miscarriage?
There’s no data to suggest that Tylenol use leads to miscarriage. “Current data doesn’t support an increase in miscarriage,” Rahman says. “However, untreated or elevated fevers can indeed lead to congenital issues or miscarriage.”
Can taking Tylenol affect baby’s brain development?
Again, data doesn’t suggest that taking Tylenol within the recommended amount will impact baby’s brain development.
So, can you take Tylenol while pregnant? The bottom line is yes. The science is clear: “Tylenol is generally safe for pregnant people,” Alan says. “However, it’s always a best practice to take the lowest dose and minimum number of doses possible to achieve the desired effect.”
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Jamie Alan, RPh, PharmD, PhD, is an associate professor of pharmacology and toxicology at Michigan State University.
Eran Bornstein, MD, is the director of the Center for Maternal-Fetal Medicine at Northwell Lenox Hill Hospital in New York City. He earned his medical degree from Tel Aviv University.
Sameena Rahman, MD, is an ob-gyn at Northwestern Medicine and founder of GYN & Sexual Medicine Collective. She earned her medical degree from the University of North Carolina School of Medicine.
American College of Obstetricians and Gynecologists, ACOG Affirms Safety and Benefits of Acetaminophen during Pregnancy, September 2025
U.S. Food and Drug Administration, Notice to Physicians on the Use of Acetaminophen During Pregnancy, September 2025
JAMA, Acetaminophen Use During Pregnancy and Children’s Risk of Autism, ADHD, and Intellectual Disability, April 2024
Environmental Health, Evaluation of the Evidence on Acetaminophen Use and Neurodevelopmental Disorders Using the Navigation Guide Methodology, August 2025
Cureus, Acetaminophen: A Liver Killer or Thriller, October 2023
Cleveland Clinic, Is It Safe to Take Tylenol If You’re Pregnant?, October 2025
Harvard Health Publishing, Acetaminophen Safety: Be Cautious But Not Afraid, April 2024
Molecular Autism, Fever During Pregnancy As a Risk Factor for Neurodevelopmental Disorders: Results from a Systematic Review and Meta-Analysis, September 2021
Learn how we ensure the accuracy of our content through our editorial and medical review process.
Target Baby Registry
Free $100+ Value Welcome KitFree $100+ Value Welcome Kit
15% Completion Discount15% Completion Discount
Free 1-Year ReturnsFree 1-Year Returns
20+ Exclusive 20% Off
Deals For Mom & Baby20+ Exclusive 20% Off Deals For Mom & Baby1:1 Concierge With
Baby Gear Specialists1:1 Concierge With Baby Gear Specialists

*Subject to availability and Retailer's terms.
We earn commissions from these links.