The 411 on Baby Acne (and How to Treat It)
Your newborn is picture-perfect, of course—but as you memorize every square inch of your little one, you may notice some blemishes on their otherwise brand-new skin. What gives? It’s not as if they’ve been chowing down on fast food. Those bumps may be red and raised, they may be tiny and white or they may resemble the acne flare-ups you experienced in high school. But while these spots may be disconcerting, they’re actually not surprising, when you think about it: Just like a teenager, a baby experiences profound hormonal shifts as they adjust to the world outside the womb, and that can manifest as baby acne. Here’s how to recognize baby acne and how to treat it when it pops up.
There are two different types of acne, depending on baby’s age. Newborn acne, otherwise known as neonatal acne, can appear when baby is a newborn up to 3 months old—and it’s totally normal. “Neonatal acne is a benign skin condition that roughly 20 percent of newborns have,” explains Katie Pyle, DO, a pediatrician at UCHealth Pediatric Care Clinic in Firestone, Colorado. “We don’t really know the cause, but it’s likely either due to the stimulation of baby’s oil glands from mom’s hormones or an inflammatory reaction to a type of yeast that colonizes on a baby’s skin.” The good news: While baby may have a few pimples in their pics, newborn acne doesn’t point to future skin problems.
If baby is older than 3 months, they may be experiencing what’s called infantile acne, especially if you notice larger red, raised blemishes or pustules, says Meagan O’Neill, MD, a pediatrician with Riley Children’s Health in Indianapolis. Like newborn acne, infant acne occurs in about one-fifth of babies. “While neonatal acne tends to go away on its own with age, infantile acne may stick around longer and, since it can be more severe than neonatal acne, may require treatment to avoid scarring.”
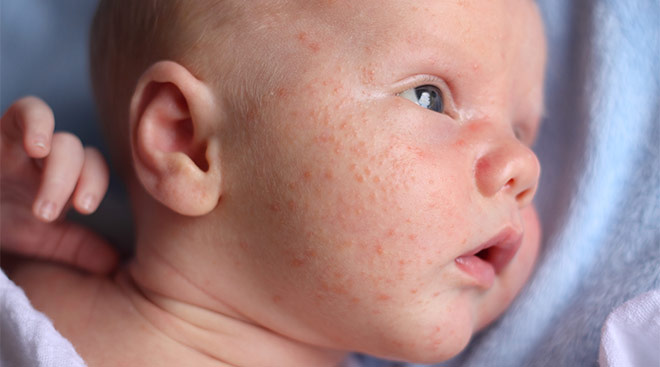
The characteristic signs of newborn acne are small red or white bumps that can appear all over the body but are usually concentrated on baby’s face and torso. You might also spy tiny white bumps on your newborn’s forehead, cheeks or near the mouth, called milia. These actually aren’t baby acne, per se—instead, the bumps are dead skin cells trapped in small pockets on the skin’s surface and tend to disappear within the first few weeks of life.
Infant acne can manifest as a crop or cluster of raised red bumps, sometimes filled with pus, and can appear anywhere on the body. Sometimes they disappear on their own; sometimes they require treatment. Unlike neonatal acne, they can be a predictor of skin issues later in life, so partnering with a pediatrician or pediatric dermatologist can help set up a smart course of treatment, says Omar Baker, MD, FAAP, assistant clinical professor in the department of pediatrics at Columbia University and co-president of Riverside Medical Group in Northern New Jersey.
Is it baby acne or a rash?
All this talk of red, raised bumps can sound suspiciously like describing a rash. And, as any parent can tell you, trying to identify a rash can be tricky work. So how do you know if it’s baby acne or a rash?
Baby acne actually falls under the umbrella of a rash. “A rash is defined as any skin change, and broadly speaking, neonatal and infantile acne are both considered rashes,” O’Neill says. That said, it can be tough to tell the difference between baby acne and other benign skin conditions that commonly affect newborns and infants, like heat rash or eczema. The best way to tell whether or not it’s baby acne is to take a close look at the rash and see how angry it looks. “Eczema and skin infections are generally red and inflamed, with areas of very dry and sometimes cracked skin,” Baker says. Here, a rundown of some common baby skin issues to help you identify the difference between infant acne and baby rashes.
• Contact dermatitis: This rash appears as red bumps or flat red areas of irritated skin, and pops up when baby’s skin comes in contact with something irritating (which is why it’s smart to use products designed for sensitive baby skin). The rash usually clears up on its own once contact with the irritant has stopped. Diaper rash is usually a form of contact dermatitis and can be resolved by changing baby’s diaper frequently and using protective ointment.
• Eczema: Eczema often looks dry and flaky, with areas of red irritation. It often appears on the cheeks, scalp and the creases of the elbow, knee and groin, and shows up later in life than newborn acne—usually between 2 and 4 months of age. It’s important to keep baby eczema well moisturized. If you suspect eczema, talk to your pediatrician about the right product to use on baby’s skin.
• Erythema toxicum: This common rash occurs in approximately 48 to 72 percent of full-term babies, according to the National Center for Biotechnical Information (NCBI), often one or two days after birth. It’s a blotchy, red rash with tiny, fluid-filled bumps (which can look like they contain pus, but there’s no infection) and clears on its own after a few days.
• Heat rash: This rash occurs when babies get overheated and the sweat glands are blocked. Heat rash typically appears where heat and moisture can get trapped: neck folds, armpits, diaper area and creases of the elbows and knees. It looks like lots of tiny red bumps and should clear on its own once baby cools down.
• Milia: These small, firm white bumps are the result of skin or keratin getting trapped under the skin. Both common and harmless, milia appear on 40 to 50 percent of newborns, according to the NCBI, and typically resolve on their own within the first few weeks of baby’s life.
It’s also helpful to know that if baby doesn’t seem bothered, that’s a great sign. “Eczema and other worrisome rashes will often cause baby a good deal of discomfort and could present with other symptoms like extreme fussiness or fever,” says Baker.
If you’re concerned about possible baby acne, flag it for your pediatrician, who can diagnose the problem and provide a best course of treatment. Plus, talking through any skin breakouts or eruptions with your doctor can help you become familiar with baby’s unique skin needs.
Baby acne is a common skin condition, but there isn’t necessarily one clear cause. Even more frustrating: There’s very little about it that you can control. Here, some of the main causes of baby acne:
• Hormones. Yup, just like when you were a teen, hormones are often to blame, experts say. For newborns, it’s actually your hormones that are likely the cause—at the end of pregnancy, a mother’s hormones can cross the placenta into baby’s system and can stimulate baby’s sebaceous (oil) glands on the skin, leading to breakouts. For infants over 3 months, their own hormones can drive an overgrowth of skin glands, causing infant acne, O’Neill says.
• Yeast. The Malassezia species, a common type of yeast that colonizes skin surfaces, can sometimes create an inflammatory reaction in newborns, resulting in newborn acne.
Baby’s skin is incredibly sensitive, so it’s important to be gentle when dealing with baby acne. That means whatever go-to techniques you used as an adolescent or currently turn to as an adult probably aren’t appropriate for baby’s skin. Here’s how to treat baby acne properly:
• Don’t scrub. Or pick at or pop those pimples. “That can break the skin, introducing bacteria and increasing the risk of infant infection,” Baker says. You could also scar baby’s beautiful skin by picking at baby acne on the face.
• Wash and moisturize. If your newborn has neonatal acne, keep baby’s face clean and moisturized. “Skin is the body’s first line of defense against infection,” says Baker. Try using a mild soap designed for babies and a fragrance-free, hypoallergenic moisturizer to keep skin healthy and supple.
• Use a humidifier. Acne may be exacerbated by dry air, so using a humidifier can ensure that baby’s skin stays moisturized, Baker says.
• Consult your pediatrician. They may have product recommendations, other tips than can help, or may refer you to a pediatric dermatologist. But don’t wait to get help: “If severe infantile acne is left untreated, it could run the risk of scarring,” O’Neill says.
Natural remedies for baby acne
If you’re eager to test out natural home remedies to treat baby’s skin, it’s smart to first check in with your pediatrician, who can assess your child’s skin and make sure those treatments won’t cause any additional harm. “Most natural remedies aren’t well studied in children, so it’s hard to predict what side effects may occur,” O’Neill says. “Particularly with something you may be putting on your baby’s skin, you might run the risk of causing further irritation or inflammation.” Some natural remedies for baby acne that you may want to discuss with baby’s doctor include:
• Coconut oil. Coconut oil is a tried-and-true baby acne treatment around the world and one Baker recommends to his own pediatric patients. This ultra-hydrating oil can help moisturize baby’s skin—just add a few drops to a cotton ball and swab over baby’s face. (This remedy may pose a small risk if baby has a coconut allergy—keep an eye out for any allergic reactions after the first few uses.)
• Breast milk. There isn’t any research indicating that breast milk will clear up infant acne, so officially, the jury’s still out on this one. But while breast milk for baby acne may sound like an old-wives’ tale, there may be something to it. There are many moms out there who sing the praises of using breast milk to clear up baby acne on the face. Breast milk is loaded with antibodies and has antimicrobial properties to improve baby’s immune system, and those benefits could transfer to topical use too. “Breast milk contains lauric acid, which has antibacterial and anti-inflammatory characteristics,” Baker says, adding that wiping a few drops of milk over baby’s skin and then letting it air dry may help. “I swore by this,” says Jenna, a nursing mom of a one-year-old. “It definitely seemed to clear up my daughter’s skin.” If you want to give this trick a try, use a clean, soft cloth to dab your breast milk onto the newborn acne.
• Changing your diet. Nursing? According to Cleveland Clinic, certain hormones from Mom’s breast milk may be affecting baby’s hormones and causing baby acne. If you’re concerned about whether breast milk may be playing a role in baby’s acne, don’t hesitate to flag it with your pediatrician.
Newborn acne can appear anytime in the first three months of baby’s life but usually disappears by month three, Pyle says. Infant acne can last a few weeks and disappear on its own or it may linger, Baker says. If you’re consistently seeing symptoms for a few months, see your pediatrician to discuss baby acne treatment options.
While it’s impossible to prevent neonatal acne, the newborn period is the best time to develop smart infant skin care habits, which can help prevent future rashes, infant acne and skin issues. Even if baby was lucky enough to be born with silky-smooth skin, many of the strategies used to treat baby acne can also help prevent it:
• Go fragrance free. The chemicals that make up artificial fragrances can irritate baby’s sensitive skin. Try hypoallergenic products, including lotions, shampoos and laundry detergents, when possible, to help prevent newborn acne.
• Wash, don’t scrub. Scrubbing can cause further irritation and make matters worse. Instead, gently wipe and pat baby’s skin dry to help prevent baby acne on the face.
• Bathe baby regularly. For older, active infants, dirt and oil can get trapped in pores and exacerbate breakouts, just like with adults, so giving baby frequent baths can help minimize the possibility of breakouts.
Generally speaking, there’s no need to see your pediatrician specifically for baby acne. If you’re concerned about trying to prevent or get rid of baby acne on the face, or you’re not sure whether it’s infant acne or something else, it’s never a bad idea to discuss it with baby’s pediatrician. It can be reassuring to find out exactly what’s going on with baby’s skin and, in the case of baby acne, to hear directly from the doctor that it’s truly nothing to be concerned about.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Omar Baker, MD, FAAP, is an assistant clinical professor in the department of pediatrics at Columbia University and co-president of Riverside Medical Group in Northern New Jersey. He earned his medical degree from George Washington University.
Meagan O’Neill, MD, is a pediatrician with Riley Children’s Health in Indianapolis. She earned her medical degree from Indiana University School of Medicine, Indianapolis.
Katie Pyle, DO, is a pediatrician at UCHealth Pediatric Care Clinic in Firestone, Colorado, with a clinical interest in newborn care. She earned her medical degree from Lincoln Memorial University-DeBusk College of Osteopathic Medicine.
Stat Pearls, Erythema Toxicum, September 2023
Maedica A Journal of Clinical Medicine, Newborn Skin: Common Skin Problems, January 2017
Cleveland Clinic, Baby Acne, December 2022
Learn how we ensure the accuracy of our content through our editorial and medical review process.
Target Baby Registry
Free $100+ Value Welcome KitFree $100+ Value Welcome Kit
15% Completion Discount15% Completion Discount
Free 1-Year ReturnsFree 1-Year Returns
20+ Exclusive 20% Off
Deals For Mom & Baby20+ Exclusive 20% Off Deals For Mom & Baby1:1 Concierge With
Baby Gear Specialists1:1 Concierge With Baby Gear Specialists

*Subject to availability and Retailer's terms.
We earn commissions from these links.