Birth Control After Baby: 9 Popular Methods
Sure, becoming a mom is pretty amazing. But you’re probably not ready to do it again so soon! These postpartum birth control methods will help you get back in bed without conceiving another baby before you’re ready. Talk to your doctor about what method is best for you.
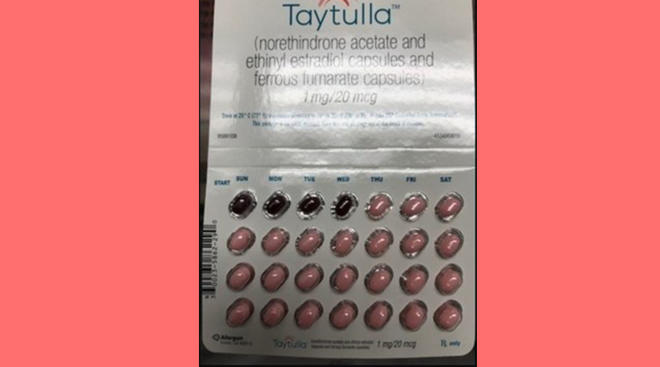
The pill
The birth control pill, which uses hormones to halt ovulation, is fine to use once you’re green-lighted for sex, usually at your six-week postpartum checkup. It’s considered 99 percent effective when taken correctly. If you’re breastfeeding, your ob-gyn will likely prescribe a progestin-only pill, also known as the minipill, which won’t affect milk production. “Birth control pills are safe in breastfeeding patients,” says Rebecca Starck, MD, FACOG, department chair of regional obstetrics and gynecology for the Cleveland Clinic. “The amount of hormone excreted in breast milk is miniscule and not harmful to the baby.” Generic brands of the minipill come and go frequently, and your doctor can prescribe whichever one is best for you.
While we’re on the topic of nursing, let us warn you now: Many women think they can’t get pregnant while they’re breastfeeding, because they haven’t started getting their period again. But that’s not actually true, since ovulation can occur before that first period without you even realizing it. “Exclusive breastfeeding does make it less likely that you’ll conceive, but if a woman doesn’t want to get pregnant I would never say it’s reliable enough to use as birth control,” Starck explains.
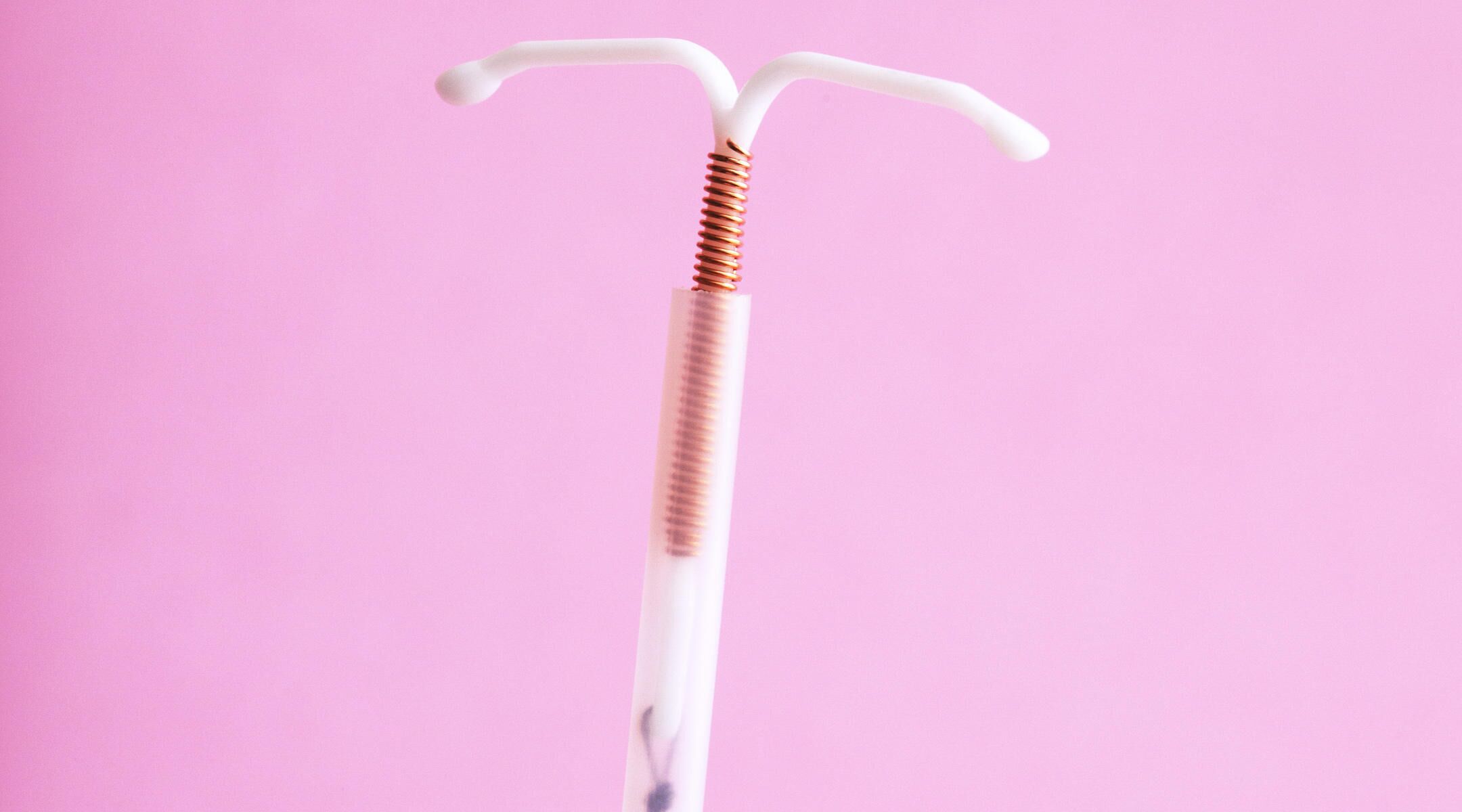
Intrauterine device
There are three kinds of intrauterine devices (IUD). The synthetic progesterone IUD, called by the brand name Mirena, excretes a hormone for up to five years that immobilizes sperm, ending their march toward an egg. Skyla does the same thing, but for three years. Instead of hormones, the copper IUD (known by brand name ParaGard) releases a safe, small amount of the metal to similarly disable sperm for up to 12 years. But Connie Young, MD, director of Women’s Health Services at Community Healthcare Network says ParaGard makes your periods heavier and more crampy. All forms are about 99 percent effective, but each have different potential side effects so talk to your doctor about which one is best for you. “Most women who have the IUD think it’s a great method because once it’s inserted, you don’t have to think about anything,” says Starck. “And it’s completely reversible.” Just have your doctor take it out when you’re ready to try to get pregnant again.
Withdrawal
Withdrawal—where you trust your partner to pull out before he ejaculates—is the sixth most common form of birth control, believe it or not. Some research suggests that when practiced perfectly, its failure rate is only 4 percent, but don’t count on it. That’s because perfection is pretty hard to achieve, so about one in five couples practicing withdrawal do conceive. “Withdrawal is probably one of the biggest lies going,” says Terry Gibbs, DO, FACOG, ob-gyn at Toledo Hospital. “There’s a small amount of ejaculate that comes out before a man comes to climax. He can’t feel it, and so withdrawal should never be considered a reliable form of birth control.”
Fertility Awareness-Based Methods
Women using fertility awareness-based methods (FAMs) or natural family planning methods avoid vaginal intercourse when they’re fertile. A couple of other ways women do this is by taking cues from their cycle to regulate fertility: examining cervical mucus for clues of ovulation and taking their temperature each morning (the number can spike when you’re fertile). Many women also choose to use ovulation predictor kits to help indicate when they are most fertile, and practice abstinence during these days. If you choose to practice one (or, more commonly, all of these methods) to predict when you ovulate each month, be warned: Failure rates can be as high as 25 percent, and women shouldn’t depend on this method if they have an irregular cycle.
Condoms
Condoms, when used properly—meaning they make it on at the very start of intercourse and remain on until finished—are up to 98 percent effective at preventing pregnancy. Condoms might be a good method for you if you’re not into the idea of medicines, devices or injections, or if you also want to protect yourself against sexually transmitted diseases.
Vaginal ring
The NuvaRing (currently the only vaginal ring on the market in the US) is a plastic ring about the size of a silver dollar that you insert in your vagina once a month. Similar to the Pill, it delivers hormones that suppress ovulation and is up to 99 percent effective at preventing pregnancy if used correctly. After three weeks, you remove the ring for a week while you get your period, and then you insert a new one. If you find yourself forgetting to take your daily pill, NuvaRing might be good for you. But because it contains estrogen, it’s not the preferred choice if you’re still nursing.
Injectable birth control
The Depo-Provera shot delivers a dose of progestin that provides three months of contraception, so you’ll have to see your doctor quarterly to get it. Think of it as the Pill by injection—this is also a good choice if you’re not good at remembering to take an oral contraceptive—and it’s 99 percent effective. Just make your appointments and you can’t make a mistake. And because it relies on progestin, not estrogen, it won’t interfere with breast milk production.
Implantable rod
If you want something long-lasting but don’t want an IUD, consider Nexplanon. A small, flexible rod that delivers synthetic progesterone into the bloodstream is inserted under the skin on the inner part of your upper arm. It’s about 99 percent effective for up to three years and is okay for breastfeeding moms.
“Nexplanon has become increasing popular for postpartum women,” says Young. “That’s because it’s so easy—with a five-minute insertion, you don’t have to think about birth control for three years.”
Nonsurgical sterilization
If you’re sure that your family is complete—and we mean 100 percent, no doubt in your mind, you never want to be pregnant again—then nonsurgical sterilization might be for you. The Essure device is inserted vaginally into the fallopian tubes, creating a roadblock in the very place where fertilization must occur. Two small coils create scarring that ensures sperm and egg can never meet. The results are similar to tubal ligation—a type of laparoscopic sterilization, but without the surgery.
Plus, more from The Bump:
Target Baby Registry
Free $100+ Value Welcome KitFree $100+ Value Welcome Kit
15% Completion Discount15% Completion Discount
Free 1-Year ReturnsFree 1-Year Returns
20+ Exclusive 20% Off
Deals For Mom & Baby20+ Exclusive 20% Off Deals For Mom & Baby1:1 Concierge With
Baby Gear Specialists1:1 Concierge With Baby Gear Specialists

*Subject to availability and Retailer's terms.
We earn commissions from these links.