What to Know About Night Terrors in Toddlers
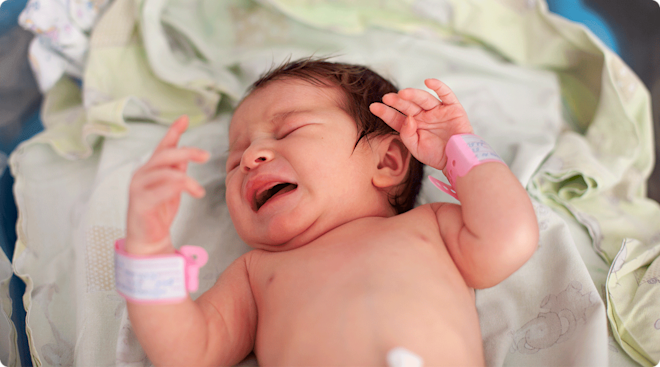
Night terrors in toddlers and young kids can be both baffling and scary. One moment your little one is sleeping soundly in their nursery, and the next they’re frantically screaming. Even more heartbreaking? During these charged moments, it’s not always clear how you can help. So what’s the deal with night terrors in toddlers? We asked experts to break down exactly what they are, why they happen and what parents need to know.
“‘Night terrors’ is a term that refers to disconcerting screaming or crying that a toddler or young child may have at night during sleep,” explains Michael McKenna, MD, a pediatrician with Ascension in Indiana. Night terrors are different from nightmares, which are “far more common and affect almost all children at some point,” says Rachel Mitchell, a certified pediatric sleep consultant and founder of My Sweet Sleeper. However, experts don’t agree on how common night terrors in children are. While Mitchell says night terrors really only occur in 3 to 5 percent of children, according to the Mayo Clinic, they may affect around 40 percent of children at some point.
Most kids who have night terrors experience them between the ages of 4 and 12, but they can also occur sooner or later, especially if a child has experienced a traumatic event, Mitchell says. Tamara Glen Soles, PhD, a pediatric psychologist and parenting coach, adds that some children as young as one year can experience them. Night terrors affect boys and girls equally, and some studies suggest they may be genetic. The American Academy of Pediatrics (AAP) says they can last up to 45 minutes, however Mitchell notes night terrors in toddlers are typically shorter in duration. “[They’re usually only a few minutes in length, but can last up to 15 to 20 minutes,” she says. If night terrors consistently last longer, you’ll want to reach out to your pediatrician for guidance.
It’s important to note that toddler night terrors aren’t related to nightmares. “These are two entirely separate entities,” McKenna says. For starters, while babies as young as 6 months old can have nightmares, night terrors are usually experienced by toddlers and preschoolers, the AAP says. What’s more, nightmares and night terrors also happen during different stages of sleep. According to the American Psychological Association (APA), the earlier sleep stages entail non-rapid eye movement (NREM) sleep, while the later stages include rapid-eye movement (REM) sleep. REM sleep tends to be deeper sleep than NREM sleep—it’s also the stage of sleep where humans experience dreams and nightmares.
Night terrors, on the other hand, occur within two to three hours of falling asleep (maybe even while the parents are still awake). They’re a fear reaction (rather than a dream) children can have if their central nervous system is over-aroused as they transition between the deepest stage of NREM sleep and the lightest stage of REM sleep, notes Johns Hopkins Medicine. Essentially, this means that while large parts of your child’s brain are asleep and in repair mode, a small part that controls their voice and movements is still relatively alert.
Experts know that children’s night terrors are a fear reaction that can occur as little ones transition sleep cycles—and they can be intensified if a child is chronically overstimulated, overtired and/or has elevated levels of cortisol (the stress hormone), Mitchell explains. So what causes night terrors in children? Below, some of the most common reasons for night terrors in toddlers and young kids:
-
Sleep deprivation: As mentioned, lack of sleep and overtiredness is frequently named by experts as a top reason for children’s night terrors.
-
Stressful life events: According to Stanford Medicine, toddler night terrors could be triggered by a traumatic event or even by family stress, as emotional stress creates physical stress on the body.
-
Family history: Both Mitchell and Soles note that night terrors in children might be genetic. “[They can be] more common if family members have a history of sleep terrors or sleepwalking,” Soles explains.
-
Fever: Fevers are tough on toddlers and young children, making their little bodies more susceptible to tension and agitation—which, in turn, leads to a higher likelihood of toddler night terrors.
-
Suppressed melatonin: Mitchell notes that exposure to blue light (from screens, for example) before bedtime suppresses the body’s natural production of melatonin, a hormone that promotes sleep, and may play a role in the development of night terrors in toddlers and young kids.
-
Sleeping in unfamiliar surroundings: For little children, sleeping in an unfamiliar place can cause overstimulation of their brains. The uncertainty and need to adjust can increase the likelihood of toddler night terrors.
-
An overfull bladder: If your child was recently potty-trained, the sensation of an overfull bladder can create an arousal of their developing nervous system during sleep. “In some cases, [this] can trigger both bed-wetting and night terrors,” Mitchell says. “[This is] one reason we recommend having children use the bathroom just before they go to sleep, and limit liquids in the evening.”
-
Traumatic head injury: Sleep patterns are negatively affected by certain head injuries and can increase the likelihood of children’s night terrors, Mitchell says. “Certain studies also show that head injuries can cause sleep disorders which can cause night terrors.”
-
Medications: According to Soles, some medications that lengthen the NREM stage of sleep could lead to night terrors. “Parents should consult their physicians about medications such as sedatives, stimulants and antihistamines to figure out how they may impact their child’s sleep,” she says.
According to the AAP and Mitchell, toddler night terrors have distinct behaviors that are easy to spot, including:
- Kicking, sleepwalking and thrashing around
- Screaming or crying uncontrollably
- Sweating, shaking or breathing rapidly
- Looking terrified, confused or staring blankly
- Having widened eyes
- Not recognizing caregivers or realizing their presence
- Pushing away those who try to comfort and hold them
Despite these behaviors, unlike with nightmares, children don’t typically wake up from night terrors. That said, they’ll eventually relax. Your child will seemingly “fall right back to sleep,” though they’ve actually been sleeping the entire time. “Unlike nightmares, children generally don’t have a memory of night terrors happening, including events, like sleepwalking, that may have occurred—although they may wake up and feel more tired or sore,” Mitchell explains.
Unfortunately there are no quick fixes or medications to address night terrors in toddlers and young children. Kids usually outgrow them naturally. However, there are some things you can do to to help keep them safe during night terrors:
-
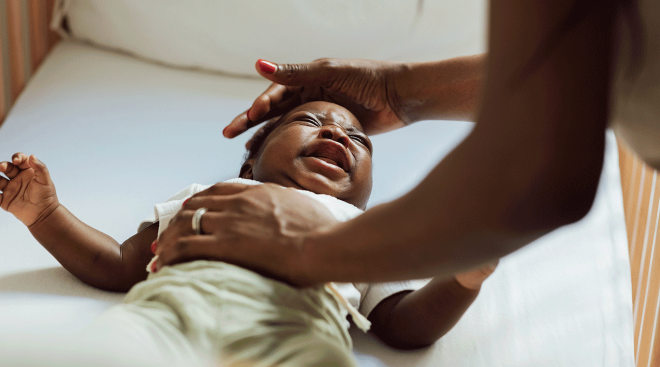
Help them return to normal sleep: It’s important to know that you shouldn’t shout at or try to wake a child in the middle of a night terror. “This could cause them to become more aggressive or increase their symptoms,” Mitchell says. Instead of promoting fear, try making soothing comments: Soles suggests saying, “You’re safe. I’m here.” You can also try holding them or [taking] their hand to comfort them, but only if they allow you to. “Many children don’t want to be touched during a night terror,” Soles adds. Finally, try gently guiding them back to bed (again, only if they allow you to).
-
Remove anything dangerous in their path: You shouldn’t try to rouse your child out of a night terror, but you can still protect them by ensuring they can’t hurt themselves or someone else. While going through a night terror, your child may move around—give them space to work through it, but be involved to steer them away from stairways, furniture or walls. “Parents should ensure they’re keeping [the child’s] body safe by removing any immediate safety hazards around them,” Mitchell says.
-
Advise and warn any caregivers: Make sure to inform babysitters and family members watching your child of the possibility of night terrors, and tell them what to do if one happens.
Certain lifestyle changes can help parents reduce the likelihood of night terrors occurring. Below, some tactics to potentially prevent night terrors in toddlers and kids:
-
Ensure a healthy sleep environment: “Ensuring children have a sleep-promoting environment, and are going to sleep within a healthy window are the most important to prevent night terrors from happening,” Mitchell says. This means setting up a good sleep space that’s quiet, dark and cool enough, as well as free of blue light and screens.
-
Create a calming bedtime routine: Having a bedtime routine that involves calming activities like bedtime stories, cuddles, songs and bath time is part of promoting a healthy sleep environment, as it winds little ones down for rest. Overstimulation prior to bedtime can cause a higher likelihood for toddler night terrors to occur.
-
Lengthen their sleep time. Overtiredness is a big contributing factor to night terrors in toddlers. After all, young children are growing and require a lot of rest to keep up with rapid development during the toddler and preschool years. A regular bedtime and nap schedule can reduce the occurrence of night terrors in children who are prone to them. Soles also recommends adding in an extra daytime nap to reduce the occurrence of night terrors.
-
Reduce stress: You might not think that young children experience stress, but they learn a lot about the world around them at a very quick rate—and that can be challenging. To help reduce their stress and offer comfort, Soles recommends making sure your little one has plenty of time to play outside and connect with you and other caregivers.
-
Look for patterns: Keep track of when the night terrors are occurring, and see if you can find a pattern for when during sleep they occur. If you can, try gently rousing them about an hour before the anticipated time, McKenna suggests. “Get them to sit up, open their eyes, recite the alphabet or anything like that,” he says. The goal isn’t to ensure your little one is completely awake, but rather to disrupt their sleep cycle so their brain can reset sleep patterns and avoid a night terror. “If you do this consistently, you should quickly start to see the episodes be less troubling, less often and then eventually stop,” McKenna says.
As scary as they can be to witness, rest assured that night terrors in toddlers and young kids can be developmentally normal; children usually outgrow them on their own. “There’s no solid research that shows they cause negative long-term effects,” Mitchell says. That said, there are certain symptoms and scenarios that warrant a call to the pediatrician, according to Stanford Medicine. These include if your child experiences:
- Drooling, jerking or stiffening movements during night terrors
- Frequent night terrors or night terrors lasting over 30 minutes
- Fear during day or around going to sleep
- Increased or sudden stress
Wondering if night terrors might point to an underlying developmental, mental or physical health issue? It’s true that children with neurodevelopmental conditions, like autism or ADHD, are more likely to experience sleep disorders, but Mitchell emphasizes these occurrences aren’t indicative of an underlying condition. “Many children experience night terrors without any mental or physical issues present,” she says. Soles agrees, adding that “the association between mental health conditions and night terrors is stronger for adults than young children.”
Whatever the situation, don’t hesitate to reach out to your pediatrician with any questions or concerns around night terrors in toddlers and kids. They can help you figure out what could be causing the night terrors and how to help prevent them.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Rachel Mitchell is a Boston-based certified maternity and pediatric sleep consultant, former night nanny and mom to seven. She’s the founder of My Sweet Sleeper, a team of maternity and pediatric sleep specialists that help growing families get some much needed shut-eye, as well as the founder of Sweet Sleep Academy, a pediatric sleep consultant certification program.
Tamara Soles, PhD, is a pediatric psychologist and parenting coach, as well as the founder of the Secure Child Center for Families and Children in Montreal, Canada. She earned her doctorate in applied child and school psychology at McGill University and completed her post-doctoral fellowship in early childhood mental health at Children’s Hospital Los Angeles.
Michael McKenna, MD, is a pediatrician with Ascension, located in Indiana. He earned his masters of science and medical degree from the Indiana University School of Medicine. He finished his residency at Riley Children’s Health in Indianapolis, Indiana.
Mayo Clinic, Sleep terrors (night terrors), April 2021
The British Journal of Psychiatry, Hereditary factors in sleepwalking and night terrors, August 1980
American Academy of Pediatrics, Nightmares, Night Terrors & Sleepwalking in Children: How Parents Can Help, September 2023
American Psychological Association, APA Dictionary of Psychology
Johns Hopkins Medicine, Johns Hopkins All Children's Hospital For Patients and Families
Stanford Medicine, Nightmares and Night Terrors
Neuropsychiatric Disease and Treatment, Traumatic brain injury-induced sleep disorders, February 2016
Learn how we ensure the accuracy of our content through our editorial and medical review process.
Target Baby Registry
Free $100+ Value Welcome KitFree $100+ Value Welcome Kit
15% Completion Discount15% Completion Discount
Free 1-Year ReturnsFree 1-Year Returns
20+ Exclusive 20% Off
Deals For Mom & Baby20+ Exclusive 20% Off Deals For Mom & Baby1:1 Concierge With
Baby Gear Specialists1:1 Concierge With Baby Gear Specialists

*Subject to availability and Retailer's terms.
We earn commissions from these links.