What to Expect at Baby’s 2 Month Checkup
By the time baby is 2 months old, you both have probably settled into a more predictable routine. Your little cutie is likely growing rapidly and learning new things each day, and they may be a little more alert during the day by this age—and paying more attention to you, watching you as you move around, cooing when you talk to them or even smiling from time to time. To ensure all of these milestones and baby’s overall development is on track, your pediatrician will want to bring them in for their two-month checkup. Here’s what to expect during the visit and how to prepare.
At two months old, baby is developing their senses and starting to follow objects with their eyes, recognizing familiar faces and attempting to communicate with different cries for different needs. During this visit, your pediatrician will still want to hear about baby’s growth, feeding and sleeping patterns, as well as the early developmental milestones they’re hitting, says Elizabeth Cilenti, MD, MPH, a pediatrician with Northern Virginia Family Practice.
Physical screenings at the 2-month checkup
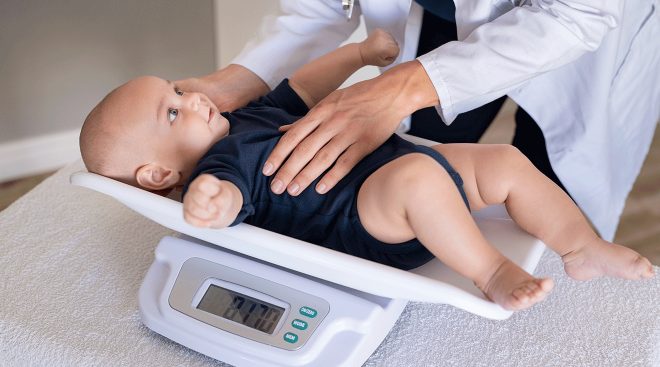
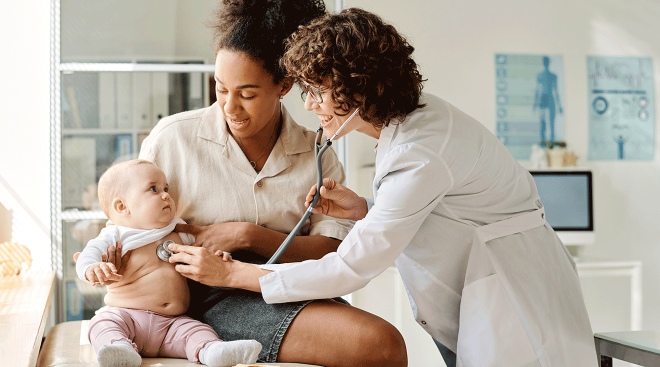
It’ll be similar to baby’s one month checkup. Your pediatrician will start off baby’s two-month well child check by measuring their height, weight and head circumference for their growth chart, which shows the average height and weight for boys and girls in baby’s age range, explains Preeti Parikh, MD, a pediatrician in New York City. But don’t worry too much about baby’s specific measurements, as doctors really just use these to ensure baby’s growth is on track. They’ll also check baby’s heart, joints, eyes, ears, mouth, lungs, genitals and reflexes, as well as the shape of baby’s head and their fontanelles (the soft spots on baby’s head) to make sure they’re developing properly.
Along with checking baby’s physical development, your pediatrician may also inquire about your mental health. They’ll want to know if you’re having any struggles with postpartum recovery, breastfeeding, anxiety, sadness and depression or anything else concerning your well-being.
Milestone assessment at 2 months
“Babies are learning new skills every day. [They] change quickly, so a lot of what we went over last visit has changed completely,” Cilenti says. At this age baby will be interested in looking around and at moving objects—and they may even start to show off their social smile. Plus, they may also be able to hold their head up during tummy time and move their limbs a little more, Cilenti says. For more information on how baby will progress, she recommends looking at the Center of Disease Control and Prevention’s (CDC) milestone tracker. “It’s a great resource for parents to familiarize themselves with what we expect at each age.” Below, some questions your pediatrician may ask at this visit:
- How are things going? Is there anything new going on? Do you have any concerns?
- Is baby gurgling, cooing and smiling?
- Do you have any concerns about baby’s vision?
- Does baby follow moving objects and faces?
- Does baby respond to loud sounds?
- Does baby recognize their parents and their voices?
- How often does baby do tummy time? Do they try to lift their head up?
- Are they able to grasp an object placed in their hand?
Nutrition check-in at the 2 month well child check
Eating is a big part of baby’s early life, and you want to ensure they’re growing well and putting on enough weight. By 2 months old, you and baby probably have a good rhythm for mealtimes—and your pediatrician will want to hear all about it. These are the questions you can expect them to ask, according to experts:
- How many times does baby eat each day and overnight?
- Are you using formula or breast milk?
- How many ounces does baby drink at each feeding (if measurable)?
- Have you introduced a bottle yet?
- How many times does baby pee in a day?
- How many times does baby poop each day?
- What is baby’s stool consistency?
- Are there any signs of dairy intolerance, like diarrhea or blood in stools?
- How are you ensuring baby is getting enough Vitamin D? Do you use supplements or vitamin D drops?
- What is your breastfeeding diet like?
- Are you and baby having any issues with feeding?
Sleep check-in at the 2 month checkup
By 2 months old, baby probably has a slightly more predictable sleeping pattern—and a few may even be sleeping through the night, Cilenti says. Still, your pediatrician will want to hear all about baby’s sleeping habits and patterns. Below, some questions they might have:
- What is baby’s sleep schedule like?
- How long does baby sleep each night?
- How often does baby wake to feed?
- What is baby’s nap schedule during the day?
- Is baby put on their back to sleep both at night and during naps?
- What is baby’s sleep environment like? Does it follow safe sleep practices?
Child safety check-in at the 2-month checkup
Similar to baby’s previous one month checkup, your pediatrician will want to ask you about several topics related to baby’s safety. Here are some of the questions your pediatrician will ask:
- Are you returning to work? Do you need help finding childcare?
- Do you have a changing table? If so, how high is it, and do you keep a hand on baby at all times?
- How do you calm baby when they cry or are fussy?
- Do you ever get frustrated when baby cries? How do you handle it?
- Have you already baby proofed your home and vehicles?
- Do you have any questions about car seat safety?
Baby will get first doses of multiple vaccinations to protect against diseases at their two month well child check, Cilenti says. These include:
- Pneumococcal conjugate vaccine (PCV)
- Diphtheria, tetanus, acellular pertussis vaccine (DTaP)
- Haemophilus influenza type B vaccine (Hib)
- Inactivated polio vaccine (IPV)
- Rotavirus vaccine (given orally)
- Hepatitis B (HBV) (if not already given at the previous checkup)
It may seem like a lot of shots, but the good news is, depending on your provider’s practice, there are many different combination vaccines available, which means less poking (and fewer tears) for your little one, Cilenti says. “Practically speaking, you should expect baby to receive one to four shots, depending on which products your pediatrician’s office carries.”
Parikh notes that your provider will likely give baby these vaccines towards the end of the visit. There may be some mild side effects, Cilenti adds, including fussiness, redness or nodules at the injection site and a fever lasting 24 to 48 hours after the immunizations. “Ask your doctor about when to call the office if baby has a fever after vaccines,” Cilenti says, as well as if to give Tylenol and at what dosage.
The CDC also notes that babies younger than 8 months will also be receiving their first dose of the new RSV vaccine starting in the fall of 2023, but doesn’t yet specify exactly when.
You’ll undoubtedly have a better grasp on life with baby as the weeks go by—but that doesn’t mean there won’t be questions. Cilenti recommends parents bring a list of any and all questions they have, as well as all baby updates since the last visit. Consider writing these down as they occur between visits on a notepad or in an app on your phone so you don’t forget anything. Below, Cilenti and the AAP note some questions to ask at baby’s 2 month well child check:
- Is it normal for baby to smile only at me (not at anyone else)?
- When should baby start solids?
- How can I handle my older kids while I’m breastfeeding baby?
- Are the medicines I’m currently taking or wish to take safe to take while breastfeeding?
- How should I introduce formula? A bottle?
- Should I increase feedings in the next few weeks?
- Is baby sleeping enough?
- How can I make sure baby’s sleeping safely?
- What should I do if baby rolls over in their sleep?
- When should I stop swaddling baby?
- What should the water temperature be for baby’s baths?
- What should I look for developmentally in baby over the next few weeks?
- What should I do when I feel myself get frustrated with baby’s cries?
- What recommendations do you have for finding a support system? Trustworthy childcare?
- What should I do when baby gets sick? When should I call you, and when should I manage it at home?
- What medications can I give baby when they’re sick?
- How can I support baby’s learning and development?
- When is it okay to take baby outside?
- How can I manage baby’s gas and constipation?
- What should I do when baby spits up?
- What should I do about baby’s acne? Cradle cap? How can I protect their skin?
- How can I protect baby from sun exposure and other seasonal dangers?
Clienti says to be sure that your pediatrician knows about your plans for childcare if you already have them, and if there are any changes to the health of other household family members. Don’t forget to bring an extra change of clothes, diapers and wipes, in case baby needs them and there’s a wait at the doctor’s office. Rest assured, while baby’s next well visit won’t be for another two months, you can always reach out to your pediatrician with any and all questions or concerns whenever they occur.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Elizabeth Cilenti, MD, MPH, is a pediatrician with Northern Virginia Family Practice. She completed her medical degree and residency at Indiana University School of Medicine and her master’s degree in public health at the Harvard T.H. Chan School of Public Health.
Preeti Parikh, MD, is a pediatrician with Westside Pediatrics, located in New York City, as well as a spokesperson for the AAP. She earned her medical degree from Rutgers University and completed her pediatric residency at Mount Sinai Hospital.
Centers for Disease Control and Prevention, Important Milestones: Your Baby By Two Months, June 2023
Johns Hopkins All Children’s Hospital, Your Child's Checkup: 2 Months, 2023
Healthy Children (American Academy of Pediatrics), Checkup Checklist: 2 Months Old), September 2021
Centers for Disease Control and Prevention, Respiratory Syncytial Virus (RSV) Immunizations, August 2023
Learn how we ensure the accuracy of our content through our editorial and medical review process.
Target Baby Registry
Free $100+ Value Welcome KitFree $100+ Value Welcome Kit
15% Completion Discount15% Completion Discount
Free 1-Year ReturnsFree 1-Year Returns
20+ Exclusive 20% Off
Deals For Mom & Baby20+ Exclusive 20% Off Deals For Mom & Baby1:1 Concierge With
Baby Gear Specialists1:1 Concierge With Baby Gear Specialists

*Subject to availability and Retailer's terms.
We earn commissions from these links.