How To Handle A High-Risk Pregnancy
From the moment you see that double line on your pregnancy test, your child’s well-being is top of mind. So it’s completely normal for expecting parents to feel shocked, stressed and scared if they’re told that their pregnancy is high risk.
But before you panic, know that the term “high risk” in no way means you won’t give birth to a healthy baby.
“There’s often a focus on everything that can go wrong, but the truth is most of the time, things go well,” says Jacob Larkin, MD, medical director of inpatient obstetric services at UPMC Magee-Womens Hospital. “Many of the issues we see during pregnancy can be treated and managed to have a healthy mom and a healthy baby.” If your pregnancy is high risk—or if you’re just wondering what makes a pregnancy high risk—this guide will help answer your most pressing questions.
Put simply, a pregnancy is high risk if there’s an above average chance of complications, either for mom or baby, due to conditions that affect health during pregnancy, delivery or even after the child is born. Very few of these conditions are actually life-threatening. In fact, doctors may label a pregnancy as high risk for relatively minor issues, and there’s a blurred line between what defines a low-risk pregnancy and a high-risk one. “There isn’t some point where a patient magically transitions from a normal to a high-risk pregnancy,” Larkin says.
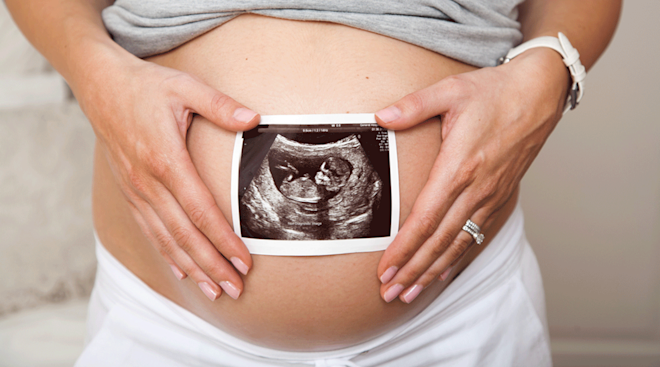
It’s also possible for risk to fluctuate throughout pregnancy, says Ozhan Turan, MD, director of fetal therapy and complicated obstetrical surgery at the University of Maryland Medical Center. For example, women over 35 are automatically placed in the high-risk category because they have a higher chance of giving birth to a child with a genetic disorder, like Down syndrome. But if fetal testing results (such as from an amniocentesis) show that the baby has no abnormalities, that mother’s status would be adjusted to normal risk.
Factors that can bump up the chance of complications during pregnancy include:
-
Being older than 35. At this age, mothers have a higher chance of delivery complications. The risk of giving birth to baby with a genetic disorder also increases after age 35.
-
Smoking, drinking alcohol or using drugs. This can lead to birth defects and other health issues for the baby.
-
Being overweight or obese. On the flip side, women who are underweight may also have a riskier pregnancy.
-
Having high blood pressure. Uncontrolled hypertension during pregnancy increases the chance of preeclampsia and low birth weight.
-
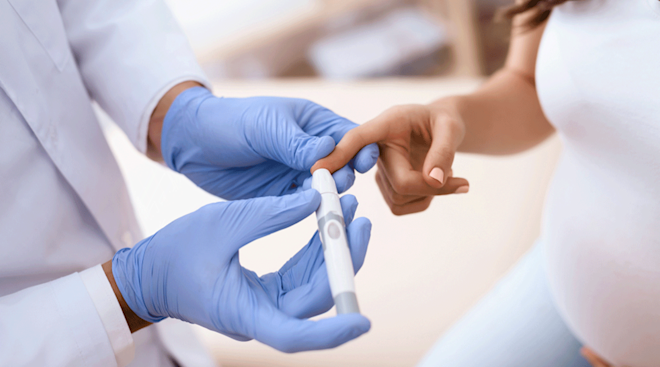
Being diabetic. High blood sugar levels can lead to birth defects early on in the pregnancy.
-
Carrying multiples. Being pregnant with twins, triplets or more can up the risk of premature birth.
-
Having had a prior pregnancy complication. If a previous baby was delivered via c-section, had a low birth weight, or was born prematurely, the chance of problems with future pregnancies can increase.
-
Having other existing health issues. Kidney, autoimmune and thyroid diseases may all set a woman up for a more complicated pregnancy.
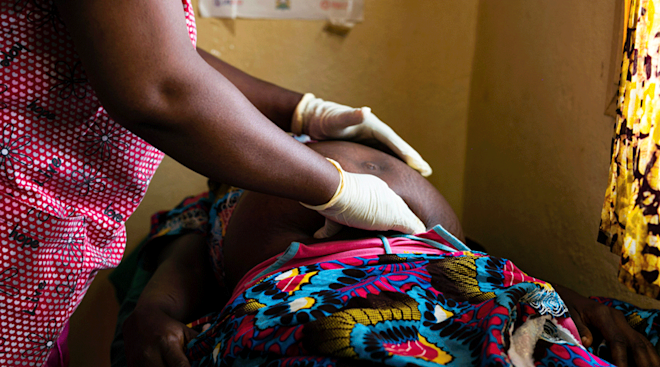
The good news is your obstetrician is already on the lookout for any trouble. “The identification of risk factors is built into the normal structure of prenatal care,” Larkin says. “The frequency of visits, the questions asked, the fact that blood pressure and urine gets checked at every visit, the ultrasounds and evaluation of baby—these are all done to look for and identify complications or indications of risk.”
For many women with a high-risk pregnancy, the main difference is you’ll be put under a greater microscope while expecting. In addition to routine prenatal visits and tests, your doctor will likely recommend additional and more frequent testing. If you have hypertension, you may need to see your doctor regularly for blood pressure readings, for example. Yes, that means a to-do list packed with visits to the doctor’s office or hospital, but the additional appointments shouldn’t be missed.
Baby will also be monitored closely, since high-risk pregnancies can set the fetus up for complications such as a low or high birth weight, birth defects and—in rare cases—the risk of death before or after delivery. “If there is any concern that a condition might introduce risk, we really escalate the amount of surveillance of baby’s well-being,” Larkin says. One of the more common tests is a nonstress test, which monitors the baby’s heart rate to ensure enough oxygen is being delivered to the brain.
If your regular obstetrician isn’t able to manage the pregnancy, you may be referred to a high-risk pregnancy doctor, such as a maternal fetal medicine doctor. (They have an extra three years of training and specialize in treating pregnancy complications—you’ll be in good hands.) It’s also important to note that a high-risk pregnancy could force you to tweak your birth plan—especially if you were hoping to give birth at home or in a birthing center. With more complicated pregnancies, it’s often safest to deliver in a hospital setting with a medical team at the ready to step in if anything does go wrong.
If you’ve been diagnosed as having a high-risk pregnancy, following these steps can help set you up for the best possible outcome—a happy pregnancy and a healthy baby:
- Stick to good-for-you habits. The usual lifestyle dos and don’ts that are recommended for any pregnancy can also benefit your and baby’s health during a high-risk pregnancy. You know the drill: Get enough sleep, eat a healthy and varied diet, exercise regularly, and avoid smoking and drinking.
- Manage your health. Now more than ever it’s important to keep health conditions such as high blood pressure and diabetes under control. Talk with your doctor if you need help coming up with a plan to stay on track.
- Manage stress. It’s normal to feel scared and stressed out about your pregnancy, but anxiety won’t just keep you up at night—it could also hurt your and baby’s health. In fact, one recent study found that a mom’s stress levels during pregnancy could impact baby’s developing nervous system, both during and after birth. Adopt relaxation techniques such as meditating or listening to music, and talk with your doctor if your anxiety feels unmanageable.
Finally, it’s smart for expecting parents to stay informed. You’ll feel more in control of your pregnancy if you have a strong understanding of what’s going on, and you may discover that your condition isn’t as scary as it sounds. “I think the most important thing to do is to get as much information as possible from reliable sources—not from Dr. Google,” Turan says. “Write down questions and discuss them with your physician. Even in the most difficult conditions, if you have all your answers in your hand you will be better able to handle the high-risk pregnancy.”
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Published March 2018
Target Baby Registry
Free $100+ Value Welcome KitFree $100+ Value Welcome Kit
15% Completion Discount15% Completion Discount
Free 1-Year ReturnsFree 1-Year Returns
20+ Exclusive 20% Off
Deals For Mom & Baby20+ Exclusive 20% Off Deals For Mom & Baby1:1 Concierge With
Baby Gear Specialists1:1 Concierge With Baby Gear Specialists

*Subject to availability and Retailer's terms.
We earn commissions from these links.