Why Some Moms Get Varicose Veins in Pregnancy—and What to Do About It
On today’s episode of Weird Things That Happen When You’re Pregnant, we’re talking about why some expectant moms get varicose veins—you know, those raised, squiggly leg lines that sometimes crop up just beneath the skin’s surface. Although the condition tends to be benign and typically resolves on its own after childbirth, varicose veins may make your legs feel achy, swollen or itchy. Basically, it’s the last thing you need when you’re busy growing a human. Read on to get a better grasp on how to handle varicose veins in pregnancy—and, better yet, learn when they’ll go away.
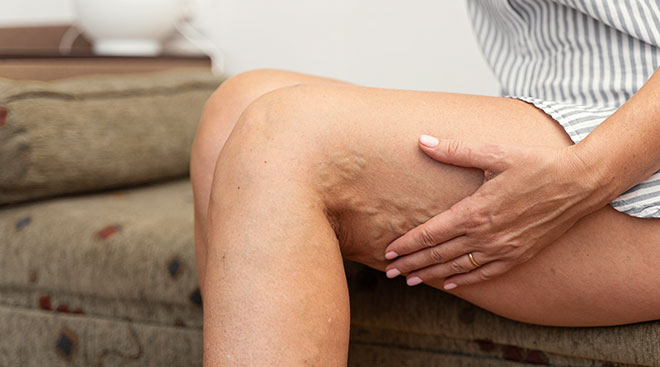
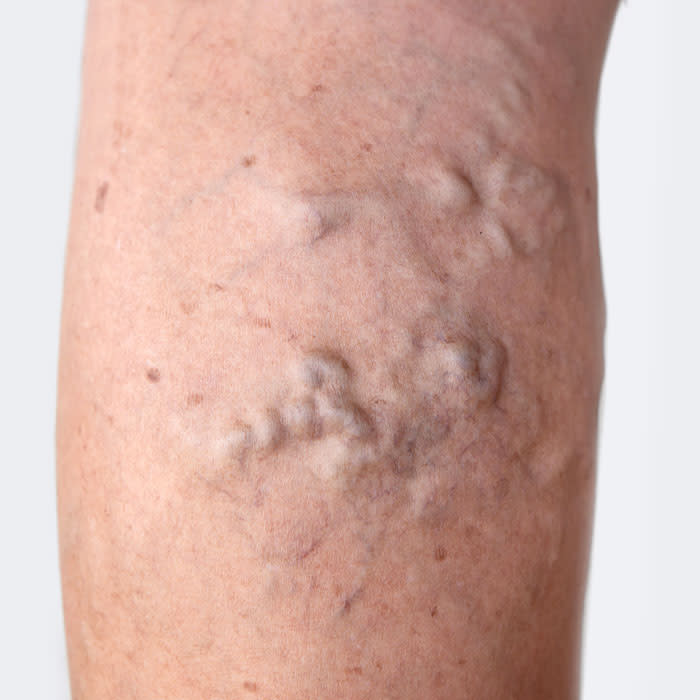
Varicose veins are enlarged and twisted veins in the legs that bulge from under the skin. They form raised, irregular lines and may cause swelling, aching, itching and heaviness in the legs. But while varicose veins can be uncomfortable for some women, others aren’t physically bothered by their presence.
Sound familiar? They’re common among the general population, and even more prevalent among pregnant women. Daniel Roshan, MD, a New York City-based ob-gyn and maternal-fetal medicine specialist, says he sees varicose veins in roughly 40 percent of his pregnant patients.
Your doctor or midwife should be able to confirm by sight, but in the meantime, you can see for yourself with a simple trick: Put your legs up in the air—if you have varicose veins, they’ll disappear when you’re in this position, says Glenn Jacobowitz, MD, a professor of surgery and chief of vascular and endovascular surgery at NYU Langone Health. It’s not magic—it’s basic biology. Typically, the muscles in your legs stop blood from pooling at your feet by pushing it up your veins through the groin to the pelvic area and up to the heart. They’re assisted by a series of one-way vein valves that are supposed to shut once the blood passes through and prevent the fluids from flowing backwards. However, when the valves are weak or damaged, or there’s extra pressure on the pelvis—as is the case during pregnancy—blood can flow backwards into superficial veins and cause them to bulge, resulting in varicose veins, explains Jacobowitz.
It’s worth noting that varicose veins are not the same as spider veins, those tiny, threadlike blue or green veins that can become dilated under similar pressure-filled circumstances. Spider veins don’t bulge like varicose veins, but they do become very visible—and they can pop up just about anywhere on your body. To add insult to injury, spider veins and varicose veins often appear together at the same time during pregnancy.
Wondering what causes varicose veins in pregnancy? For starters, you have extra blood volume. What’s more, your growing baby and expanding uterus put pressure on your pelvis that can lead to a backflow of blood into superficial veins. And if you’re predisposed to varicose veins due to weak vein valves or genetics, they may just appear one day. Some early research also indicates that hormonal changes can play a role here, but additional follow-up is needed.
While it can happen to anyone during pregnancy, there are some risk factors for varicose veins, according to the National Heart, Lung and Blood Institute. These include:
- Advanced age
- Long periods of standing, sitting or inactivity
- Excess weight or obesity
- A personal or family history of varicose veins
Being pregnant with twins or multiples potentially puts you at greater risk for more severe varicose veins, says Jacobowitz.
Don’t expect varicose veins to tip you off to an unconfirmed pregnancy during your first trimester. Varicose veins are most common during the second and third trimesters of pregnancy, when the weight of your uterus and your growing baby begin to apply pressure to the pelvic area, explains Jacobowitz.
Do varicose veins go away after pregnancy?
The reassuring news is that those bumpy veins should recede. Varicose veins almost always get better within a few weeks after delivery, says Jacobowitz. “It’s why we never operate during pregnancy,” he adds. That said, if they staunchly remain past six weeks postpartum, they probably won’t go away on their own. In this case, you might consider seeking a vascular surgeon who can outline your treatment options—more on that here.
More often than not, varicose veins affect the legs. Vulvar varicose veins in pregnancy are also possible, though. These tangled lines appear just outside of the vulva. Once again, you can go ahead and blame that budding human inside of you. The pressure of your growing baby and enlarged uterus on the lower abdomen is what causes vulvar veins to bulge in a condition known as vulvogavinal varicosities, which Roshan sees in about 5 percent of pregnant patients.
In very rare cases, extreme vulvovaginal varicosities could cause bleeding if injured during a vaginal delivery, Roshan says. But don’t panic; typically, they’re mild and controllable. (Just add it to the list of uncomfortable annoyances that occur during pregnancy.)
Looking to get some relief from varicose veins in pregnancy? There are a few steps you can take to reduce your varicose veins from bulging and causing you discomfort. Roshan recommends doing the following:
- Avoid extended periods of standing or sitting.
- Elevate lower limbs when you’re resting.
- Get regular exercise.
- Try compression. Depending on the location of the varicose veins, your doctor might recommend wearing compression knee highs, thigh highs or pantyhose with a maternity pouch for extra support, Jacobowitz says. You can take them off when you go to sleep, since elevating your legs on your bed will offer its own relief.
Unfortunately, compression garments and relaxation are simply temporary Band-Aids for pregnant women. “Varicose veins aren’t a problem you can really fix during pregnancy because of the pressure,” Jacobowitz says.
Generally, varicose veins in pregnancy are more of an inconvenience than a true problem. Still, you want to make sure your ob-gyn or midwife is aware of the issue, and that you escalate any worsening symptoms.
In rare cases, varicose veins can become inflamed due to a blood clot during pregnancy—and that can be dangerous. Tell-tale signs may include redness and swelling; the vein will become hard and painful, says Jacobowitz. If you feel any tenderness, call your ob-gyn. They may refer you to a pulmonary surgeon who can prescribe blood thinners or an anti-inflammatory that should clear things right up.
In the absence of inflammation, varicose veins won’t affect baby—so cross that concern off your list!
Unfortunately, there’s not much you can do to prevent varicose veins during pregnancy. If you know you’re prone to getting them—perhaps from a previous pregnancy—you can begin wearing compression garments at the first signs of appearance, Jacobowitz suggests. But, seriously, don’t freak out if you develop them. ”It’s not typically symptomatic of larger issues,” he says.
Those pesky varicose veins should subside on their own after baby is born. But, if not, there are minimally invasive treatment options available. In short, a vascular surgeon will choose one of several techniques to shut down blood flow to the problematic veins. And, for the record, you don’t have to worry about losing a vein your body needs. “We’re all built with many, many back-up veins because we tend to damage them all the time, ‘’ explains Jacobowitz. “There are always more where that came from.”
Remember, you don’t have to worry about treatment until you know your varicose veins persist post-pregnancy. Hopefully, they’ll go away naturally. In the meantime, put your feet up (seriously, it’ll help!) and try not to stress. The reality is that you may encounter all sorts of physical weirdness during the next 9+ months. Varicose veins in pregnancy may just be part of the ever-surprising journey.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Glenn Jacobowitz, MD, is a professor of surgery and the chief of vascular and endovascular surgery at NYU Langone Health. He received his medical degree from New York University.
Daniel Roshan, MD, is a New York City-based ob-gyn and maternal-fetal medicine specialist. He earned his medical degree from Tel Aviv University.
Ginekologia Polska, Risk factors for the development of venous insufficiency of the lower limbs during pregnancy--part 1, December 2012
National Heart, Lung and Blood Institute, Varicose Veins, September 2023
Learn how we ensure the accuracy of our content through our editorial and medical review process.
Navigate forward to interact with the calendar and select a date. Press the question mark key to get the keyboard shortcuts for changing dates.