5 Medication Options for Pain Relief During Labor
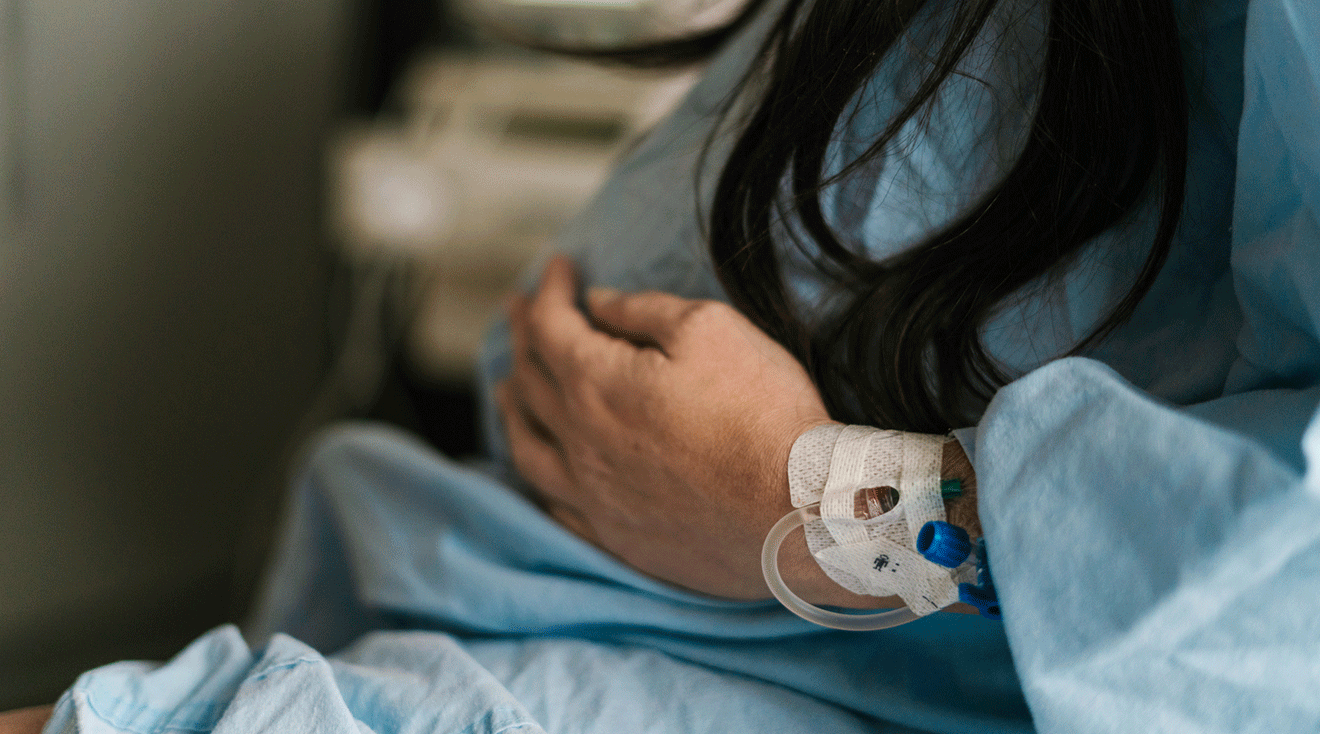
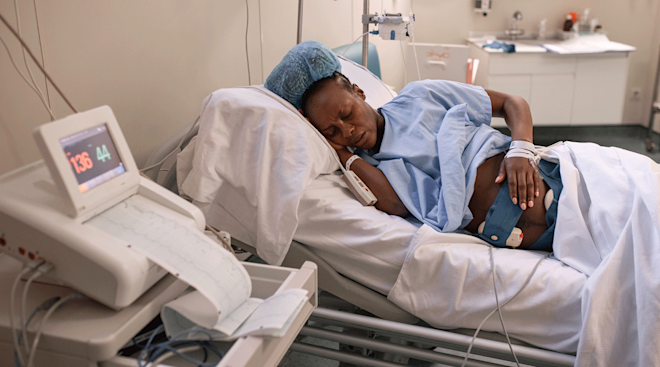
It’s a fact of pregnancy: Before the awws come the owws. Yes, labor pain can be excruciating, but thankfully, doctors have a number of options for easing it. The question is: Which one is right for you?
One factor to consider is your level of pain tolerance: Can you typically handle discomfort, or do you cringe at the thought of a flu shot? Do you think you’ll want medication to quash labor pain discomfort ASAP, or are you okay waiting until later into your labor? Also keep in mind that exhaustion can lower pain tolerance, so if you got little sleep in those last few weeks, you may find yourself needing pain medication during labor sooner than expected.
That said, it’s best not to commit yourself to any particular labor pain management strategy. “Keep an open mind,” says Philip Hess, MD, director of obstetric anesthesia at Beth Israel Deaconess Medical Center in Boston. “The doses and techniques we use are designed to be as safe as possible, so if you try one and it doesn’t work, you can move on to another. Having that flexibility allows women to have the best experience possible.”
Even if you opt for a natural birth and intend to bypass the meds entirely, know that you can change your mind during labor. “There are a fair number of patients who think they’ll breathe through the process and endure the pain, but then they get to the hospital and have contractions and that whole birth plan goes out the window,” says Jeffrey Bernstein, MD, chief of the division of obstetrical anesthesia at Montefiore Medical Center in the Bronx, New York.
Still, it’s important to be familiar with your labor pain medication options at the hospital—so when the time comes to choose, you can make an informed decision (despite being just a little distracted).
When it comes to pain relief during labor, most women in the US opt for an epidural, also known as an epidural block—and for good reason. “The amount of pain relief is significant—it can take away 90 to 100 percent of pain,” Hess says. Although it’s commonly used, epidurals may not be available at all hospitals (especially smaller or rural locations).
How is an epidural administered?
To make the process as pain-free as possible, your anesthesiologist first administers a local anesthetic to numb the area of the back where the epidural will be placed (you’ll feel a pinch). Then, with a slightly larger needle, you’ll get an injection of a small amount of anesthetic, or a mixture of anesthetic and narcotics, depending on the solution that your hospital uses. This goes into the outermost part of the spinal canal, called the epidural space. You should only feel pressure, and the pain relief will kick in around 20 minutes later. “The anesthetic and narcotics work on the nerve fibers in the spinal cord, numbing them so that you don’t feel pain when you’re having a contraction,” Bernstein explains.
That one shot doesn’t always last until delivery, so the doctor usually sets up a catheter, which allows additional anesthetic or narcotics to be injected throughout labor and even after delivery. “The catheter is about the same width as angel hair pasta and flexible and soft, so you won’t feel it once it’s in place,” Hess says. Once you have the catheter, there’s no worrying about the meds wearing off, since you can get relief for as long as you need it.
What can I expect once I get the epidural?
Once the epidural is in place, you’ll lose some feeling in the lower half of your body, so don’t plan to get up and stroll around the hospital, since you likely won’t be able to move your legs. If moving your legs is important to you, ask your hospital if it provides a low-dose epidural (also known as a walking epidural), which uses a reduced amount of anesthetic to keep you more mobile. “Each medical center runs its own solution,” Hess says, and many centers concoct a so-called walking epidural solution. Depending on the solution and your strength, this would allow you to move your legs, turn around in bed or, in some cases, even go to the bathroom, he says.
It’s thought that epidurals can result in a longer second stage of labor, but new research shows this may not be the case. In the study, the length of the second stage of labor was about the same for women who had an epidural as it was for those who were given a saline placebo. More research is needed, and Bernstein points out that without the feeling of discomfort you get from a meds-free birth, some women may simply have a decreased urge to push through their labor, which could, in fact, slow the process.
Does the epidural come with any risks?
Epidurals aren’t for everyone. If you have had spine surgery, are allergic to anesthetic or have blood-clotting problems, you typically won’t be able to get an epidural. And an epidural does come with an increased risk of temporary side effects, including itchiness (anywhere on the body), low blood pressure and a bad headache (which can occur if the epidural needle goes too deep, causing spinal fluid to leak).
A spinal block is similar to an epidural, except the anesthetic is injected even closer to the spinal cord, causing the lower half of the body to go numb faster.
When would I want a spinal block?
A spinal block is great when you want to nix labor pain ASAP. For example, if you arrive at the hospital in active labor—meaning your contractions are long, strong and close together—you may not want to wait the 20 minutes it takes to get relief from an epidural. In this case, a spinal block may be the better option, as the single shot takes effect in just a couple of minutes, Bernstein says. Spinal blocks are also often used for c-sections.
What can I expect once I get the spinal block?
Getting a spinal block will feel the same as getting an epidural, but the downside is that the labor pain relief only lasts an hour or two. That’s why many anesthesiologists administer what’s called a combined spinal-epidural block. “We give a spinal block at the same time as placing the epidural catheter to help get the pain quickly under control, and then place the epidural for continued pain relief,” Hess says.
Does the spinal block come with any risks?
The side effects and risks that come with a spinal block are the same as those that come with an epidural. However, a combined spinal-epidural block may be more likely to cause an uncomfortable itching sensation. And like an epidural, smaller hospitals or ones that don’t have an anesthesiologist on staff may not be able to administer spinal blocks.
Opioids (aka narcotics or analgesics) also ease labor pain, but they don’t numb the body like an epidural. Instead, these meds (which include morphine, fentanyl, Nubain and Stadol) work on the nervous system to help block pain, resulting in a drowsy, calming state. Because an anesthesiologist isn’t needed to administer narcotics, they are readily available at hospitals.
How are opioids administered?
Opioids can be administered as a shot into the muscle (such as the thigh or buttocks) or dripped into the bloodstream via an IV. Opioids are typically used during the early and active stages of labor, but your doctor will hold off on using them once you start pushing, since they can affect baby if used too close to your delivery.
What can I expect if I use opioids?
The pain relief isn’t as strong as an epidural and only lasts about two hours, Hess says, but it does work within minutes. You may feel sleepy and even nod off between contractions. “Narcotics are good for someone who’s in early labor and needs to get some rest, or someone who’s having labor but has become exhausted and needs to take the edge off the pain and recuperate for a couple hours,” he adds.
What risks come with using opioids?
Unlike with an epidural, opioids cross the placenta and can affect baby—especially when given late in labor, Hess says. That means baby may appear sedated upon delivery. Opioids can also increase the chance of nausea, vomiting and a drop in blood pressure.
Also referred to as laughing gas, nitrous oxide for labor isn’t widely available in the US, though it’s starting to become more common, Hess says. But because most hospitals don’t yet use it, you’re not guaranteed to have this option available during labor.
How is nitrous oxide administered?
The mom-to-be places a mask over her face and breathes in a combination of nitrous oxide and oxygen. The gas has no taste or odor, and works by lowering anxiety levels to make labor pain easier to tolerate. Unlike with other labor pain medication options, the patient is in control and decides when and how often to breathe in the nitrous oxide.
What can I expect if I use nitrous oxide?
Don’t expect your discomfort to—poof!—be gone as soon as you start breathing in the laughing gas. In fact, new research shows that about 60 percent of women who use nitrous oxide end up having an epidural. “It’s a pretty weak pain relief medication, but good for patients who want to be in control of their experience,” Hess says, noting that nitrous oxide works very quickly, usually within 30 seconds. Still, it can get tricky. “You have to start breathing at the beginning of the contraction. If you wait too long, it may kick in after the contraction has passed.”
What risks come with using nitrous oxide?
Laughing gas for labor can cause nausea and dizziness, but this feeling usually passes within minutes.
Chances are you won’t receive a pudendal block—another anesthetic-based pain relief method—during your delivery. It helps ease pain in the lower vagina and perineum (area in front of the anus) but isn’t commonly used, since an epidural has those areas covered too. Pudendal blocks are also used only during the second stage of labor when the mom-to-be is fully dilated and ready to push, Bernstein says. Your doctor might use it, however, if an epidural isn’t an option and she needs the help of forceps, suction cups or an episiotomy to deliver baby.
How is a pudendal block administered?
A doctor (usually your obstetrician) injects the anesthetic into nerves in the vaginal wall. This helps ease pain in the area for up to an hour. “It can be hard to administer because by this point of labor, the woman is in so much pain that it’s going to be difficult for her to lie still while someone sticks a needle into her cervix,” Bernstein says.
What can I expect if I use a pudendal block?
You’ll experience numbness of the vagina and birth canal, but the pudendal block doesn’t do anything to help with contractions, Hess says. The pain relief also doesn’t last long, which is why doctors administer it soon before delivery.
What risks come with using a pudendal block?
A pudendal block is generally safe, but—like with an epidural—shouldn’t be used if you have allergies to anesthetics.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Target Baby Registry
Free $100+ Value Welcome KitFree $100+ Value Welcome Kit
15% Completion Discount15% Completion Discount
Free 1-Year ReturnsFree 1-Year Returns
20+ Exclusive 20% Off
Deals For Mom & Baby20+ Exclusive 20% Off Deals For Mom & Baby1:1 Concierge With
Baby Gear Specialists1:1 Concierge With Baby Gear Specialists

*Subject to availability and Retailer's terms.
We earn commissions from these links.