What to Know About C-Section Procedures
If you’re like many women whose pregnancy is progressing steadily toward a vaginal birth, there’s one area of your birth plan you’re probably not fleshing out: What happens in the event of a cesarean section? No one wants to dwell too deeply on the circumstances that call for surgery. But given that roughly 1 in 3 US births today are via c-section—most of which occur well after vaginal labor is underway—it’s best to know a little bit about what the c-section procedure entails, just in case. After hours of laboring, when you see your OB suddenly rip off their white jacket and call for an anesthesiologist and OR prep, some information about what you’re getting into can really help dissipate the confusion.
Want to understand what happens during a c-section, why you might need one and just how long the surgery will take? We have the answers—plus, a step-by-step guide to a typical c-section procedure.
Most women plan to give birth to their baby vaginally—but when problems arise, either during pregnancy or labor and delivery, a c-section procedure may be in order. A cesarean section, aka c-section, is a surgical procedure used to deliver baby through incisions made in a mother’s abdomen and uterus. It’s considered to be major surgery, so a c-section can potentially lead to more complications for you and baby than a vaginal birth. But if your health or the health of your little one is at risk during childbirth, a c-section may be the safest way to bring baby into the world.
Why it’s called a cesarean section
There are many references to cesarean sections in ancient folklore from around the world, from China to India to Europe, but the history behind the name remains unclear. According to pop culture, some believe the term comes from Julius Caesar as the first to be born from a c-section procedure. At the time of Caesar’s birth, the surgery was primarily used on mothers who were dead or dying, though Caesar’s mother lived to hear about her son’s invasion of Britain. However, according to the US National Library of Medicine, it’s more likely due to the Latin derived from an Ancient Roman law, issued for population increase, that dictated women should be cut open to save the child if a vaginal birth is not possible.
Fortunately, we’ve since come a long way. Presently, around 30 percent of all births in America are conducted via cesarean section, the American College of Obstetricians and Gynecologists (ACOG) notes. Today, a c-section is commonly used for a range of reasons to make sure both mom and baby come out of the OR healthy.
There are several reasons to have a c-section, and many of these will be based on your individual circumstances. According to Johns Hopkins Medicine, these include:
- Abnormal fetal heart rate
- Abnormal fetal position
- Baby is too big for vaginal delivery
- Vaginal labor is not progressing as it should
- Issues with the placenta (such as its placement)
- Maternal medical issues, such as high blood pressure or diabetes
- Active herpes sores in the vagina or cervix
- A pregnancy with twins or multiples
- A history of previous c-sections
There are three types of c-sections: unplanned, emergency and scheduled. The type you’ll have will largely depend on your individual circumstances and reasons for a c-section procedure. Here’s what to know about each:
-
Unplanned c-section. OBs employ an unplanned c-section to skirt serious harm to a mother or baby after labor is already underway but for one or more reasons has stalled. Either the baby is too big to pass through the mother’s pelvis, her contractions aren’t strong enough to open the cervix so her baby can descend or the baby is facing the wrong way. OBs will also decide on a c-section if the placenta is covering part or all of the mother’s cervix, otherwise known as placenta previa. “Babies don’t have a lot of blood they can afford to lose,” says Carla Weisman, MD, an ob-gyn in Baltimore. If your doctor does a c-section due to excessive bleeding from an unresolved placenta previa, that’s considered an emergency c-section (see below).
-
Emergency c-section. An emergency c-section happens when baby is in distress during labor. For instance, “if a baby’s heart rate drops precipitously below the normal range and isn’t coming back up, if the umbilical cord comes out the vagina [before imminent delivery], or if a mother has had a c-section previously and her old scar ruptures when she’s trying to have a vaginal birth,” Weisman says. While uterine rupture is very rare—12 in 36,000 births, according to one study—it can be hard to detect and could result in heavy bleeding, fetal distress, ejection of the fetus and/or placenta into the mother’s stomach and a hysterectomy.
-
Scheduled c-section. A smaller percentage of c-sections are ones that moms-to-be and their OBs schedule ahead of time, before labor begins, mostly due to the way baby is positioned—either transverse (sideways) or breech (buttocks or feet first). The training today is not so profound that all OBs know how to deliver a breech baby vaginally, says William Schweizer, MD, an ob-gyn at NYU Langone Health in New York City. Mothers delivering multiple babies also have a high rate of scheduled c-sections, especially if the babies need to be delivered prematurely or if they aren’t ideally positioned. Plus, most women who’ve had previous c-sections also tend to plan c-sections for subsequent births rather than going the VBAC (vaginal birth after cesarean) route, especially if their scar runs vertically and increases the risk of uterine rupture.
Can you request a c-section?
Yes, first-time mothers can—and do—request a scheduled c-section, usually because they fear the pain of childbirth and the incontinence that can follow some vaginal births. “It’s not very common,” says Robert Atlas, MD, chair of obstetrics and gynecology at Mercy Medical Center in Baltimore. “And of course, we’ll discuss with them why they should or shouldn’t opt for one.”
Experts don’t yet have a limit to how many c-sections a woman can have. However, it’s important to be aware that the more c-section births you have, the greater the risk for medical problems and issues with future pregnancies, the ACOG says. (More on this below.) If you’d like to request a c-section, talk to your doctor about your concerns and desires for the birth. They’ll be able to help you map out the best birth plan for your specific circumstances.
Like any major surgery, a c-section procedure comes with a basket of risks and complications that mothers must sign off on. “Every time I open someone up, there is a chance of adhesion—the bowels can get stuck to the abdominal wall,” Schweizer says. “The bladder can also get pushed up.” In addition, he notes that the risks increase with multiple c-sections. “The chances of the placenta being abnormal is greater,” he says. In rare instances, you could end up with complications that require a hysterectomy. Many complications, though, can be treated quickly in the OR, such as:
- Blood loss
- Infection
- Blood clots in the legs
- Injury to internal organs
- Fluid in baby’s lungs
- Bad reaction to anesthesia or other medications used
Some of these c-section risks may be intensified if the mother has had previous surgeries in her midsection because of the presence of scar tissue, Weisman notes.
So how does a c-section procedure work? Once your OB makes the c-section call, things move pretty quickly. Here’s a step-by-step breakdown of what to expect:
C-section procedure preparation
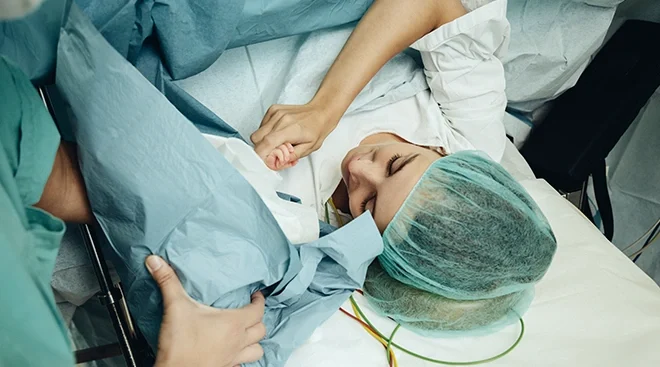
First, the doctors will prep you for the c-section procedure. You’ll get an IV inserted into your hand or arm if you haven’t had one already, you’re moved into the OR and your stomach gets scrubbed down right before draping. If you haven’t already, you’ll probably get an epidural or spinal block—or a combination of the two—which numbs your lower body. In this case, you won’t feel any pain, but you’ll be awake. General anesthesia (when a mother is put completely to sleep) is rarely used—except in the event of true emergencies when complications arise that require more time than what a spinal block allots, Schweizer says. Either way, you’ll probably also have a catheter placed. Your doctors might request that your arms be strapped down so that you remain safe and don’t accidentally interfere with the procedure. This practice is largely based on the hospital’s policy and your individual circumstances. For specific questions and concerns, it’s best to reach out to your healthcare provider.
The medical team will then drape a curtain just below your chest so you don’t have to watch the c-section surgery. Some hospitals perform gentle c-sections, which may include a transparent cellophane curtain that allows mothers to see baby when they’re lifted out and to do skin-to-skin contact almost immediately afterward.
Incisions are made
Once your OB is certain you’re numb and won’t feel any pain, they’ll make at least two incisions: one to open your skin and one across the lower part of your uterus, according to the Mayo Clinic. Usually, c-section incisions are horizontal—a bikini cut—although vertical cuts, which offer more room to extract the baby, are used when the baby is sideways, premature or when the mother is obese.
While the doctor will cut the abdominal wall, they won’t actually cut your abdominal muscles. Rather, they will move them aside, explains the American Pregnancy Association. Your bladder and intestines may also need to be moved out of the way.
Baby is born
Now is the exciting part: Your doctor will begin to carefully pull baby out. At this point, you may feel some tugging or pulling, but you shouldn’t feel any pain. If you do, let your anesthesiologist know right away.
During a gentle c-section, the practitioner usually cuts the umbilical cord and immediately hands baby to a pediatric team to ensure they’re responsive, breathing well and haven’t aspirated any amniotic fluid. They’ll also pull out the placenta. Once the baby is checked out by the pediatrician, you can request skin-to-skin time or even the first breastfeeding session, though there might only be time for a quick cheek nuzzle.
Incisions are stitched
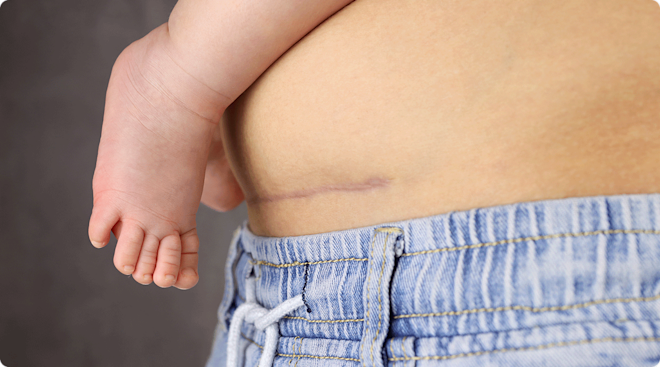
After your OB removes and inspects your placenta, they’ll start stitching you up. The uterus is usually sutured with dissolvable stitches. Depending on your doctor’s preference and your particular c-section procedure, the abdominal incision will be closed with either stitches or staples. Research has found that the use of stitches reduces the risk of wound separation and infection. Staples, on the other hand, are faster.
C-section post-op recovery
Your medical team will monitor you closely to ensure your vitals are stable before sending you into the postpartum recovery room, where you can reunite with baby.
From start to finish, how long does a c-section take? If all goes smoothly, a c-section procedure lasts roughly 45 minutes, according to the Cleveland Clinic. Add 15 to 20 minutes if you require more medication and need to wait for it to take effect. And if things get complicated—there are adhesions of your body parts that require additional surgical techniques or you’re bleeding excessively (which, if every effort to stop the bleeding fails, may require a hysterectomy)—you might have to be put under general anesthesia to allow for another hour or two of surgery.
You shouldn’t really feel any pain during a c-section, but may feel some pressure and tugging. Once the searing prick of the epidural and/or spinal block is over, the sensations are more strange than anything else. You may shiver involuntarily from the medicine and you’ll probably feel cold in the chilled OR. There’s a lot of pressure on your abdomen as the c-section procedure starts and as your doctor pushes on your belly to help deliver the baby.
“Depending on the surgeon, the uterus is taken out and put on top of the mom’s belly so we have better visualization and exposure while closing the uterine incision,” Weisman says. “It’s sometimes uncomfortable for the patient to have the uterus on the abdomen, because it stretches the peritoneal lining and may cause nausea.”
The first 12 hours after a c-section procedure can be excruciating, though not necessarily pain-wise. If you had an epidural, your OB can administer narcotics for the next day or so before switching you to oral ibuprofen or acetaminophen. All you’ll want to do is sleep off the impact of the anesthesia, but if you’re breastfeeding, you’ll get woken up every couple of hours to feed baby. “The best thing is to get whatever help you can,” Weisman says. “That may mean sending baby to the nursery for a while, and you shouldn’t feel guilty about that.”
Once you’re no longer numb, practitioners will get you up and out of bed for a quick walk to the bathroom or around your room, which “decreases your risks of breathing problems, improves your pain tolerance and helps to avoid developing blood clots in your lower extremities,” says Yvonne Butler Tobah, MD, an ob-gyn affiliated with the Mayo Clinic in Rochester, Minnesota. Walking around soon after a c-section should also open up your bowels a little faster. To that end, Schweizer recommends chewing peppermint gum as soon as you can after c-section surgery, which he says helps.
You’ll feel sore and have cramping and also see bleeding, which are signs that your uterus is shrinking and healing. Most c-section patients spend an average of two to three nights in the hospital before they can go home; this is mostly so your practitioners can closely watch your c-section incision for signs of infection and make sure you’re healing throughout. The silver lining: Spending more time in the capable hands of nurses as you get acquainted with baby can help gradually build up your self-confidence, which you’ll need when you return home.
The general consensus is that it takes longer for your body to feel whole again after a c-section procedure than it does with a vaginal birth, but there are doctors who advocate for streamlining the process—healthily, of course—especially for mothers who have been through it more than once. For women who have had a repeat c-section and who have breastfed with prior children, Schweizer sometimes recommends releasing them from the hospital within 48 hours.
“The idea is that these women who understand what c-section pain is like and who have other children at home—they want to get home,” he says, noting that educating new mothers on breastfeeding makes up the bulk of what they need to learn before returning home. “Hospitals can be dangerous places for falls and infections. We want to get you out quickly to the advantages of home.”
As you adapt to your new normal with baby, you’ll need to manage the pain in your c-section incision, cramping (especially while breastfeeding) and continued bleeding. You’ll also have a checkup with your OB within a week to ensure you’re healing well. With the right strategies and care at home, your body should feel like itself again (albeit on minimal sleep) in four to six weeks.
C-sections may sound scary, especially if you haven’t planned for it, but take heart in knowing that they’re common surgeries in the United States. Whether or not a c-section procedure is part of your initial birth plan, understanding what happens during a c-section can help you feel educated and empowered throughout your pregnancy, leading up to the grand finale event.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Robert Atlas, MD, is chair of obstetrics and gynecology at Mercy Medical Center in Baltimore. He received his medical degree from Jefferson Medical College
William Schweizer, MD, is an ob-gyn at NYU Langone Health in New York City. He received his medical degree from SUNY Stony Brook.
Yvonne Butler Tobah, MD, is an ob-gyn affiliated with the Mayo Clinic in Rochester, Minnesota. She earned her medical degree from Michigan State University College of Human Medicine.
Carla Weisman, MD, is an ob-gyn in Baltimore. She earned her medical degree from New York University School Of Medicine.
US National Library of Medicine, Cesarean Section - A Brief History, July 2013
American College of Obstetricians and Gynecologists, Cesarean Birth, May 2022
Johns Hopkins Medicine, Cesarean Section, 2023
The Journal of Obstetrics and Gynecology of India, A Case Series of Uterine Rupture: Lessons to be Learned for Future Clinical Practice, January 2013
American College of Obstetricians and Gynecologists, Cesarean Birth, May 2022
Mayo Clinic, Uterine incisions used during C-sections, 2023
American Pregnancy Association, Cesarean Procedure
American Journal of Obstetrics and Gynecology, Suture versus staples for skin closure after cesarean: a metaanalysis, December 2014
Cleveland Clinic, C-section, August 2022
Learn how we ensure the accuracy of our content through our editorial and medical review process.
Target Baby Registry
Free $100+ Value Welcome KitFree $100+ Value Welcome Kit
15% Completion Discount15% Completion Discount
Free 1-Year ReturnsFree 1-Year Returns
20+ Exclusive 20% Off
Deals For Mom & Baby20+ Exclusive 20% Off Deals For Mom & Baby1:1 Concierge With
Baby Gear Specialists1:1 Concierge With Baby Gear Specialists

*Subject to availability and Retailer's terms.
We earn commissions from these links.