First-Time C-Section Rates Are at an All-Time High, New Report Shows
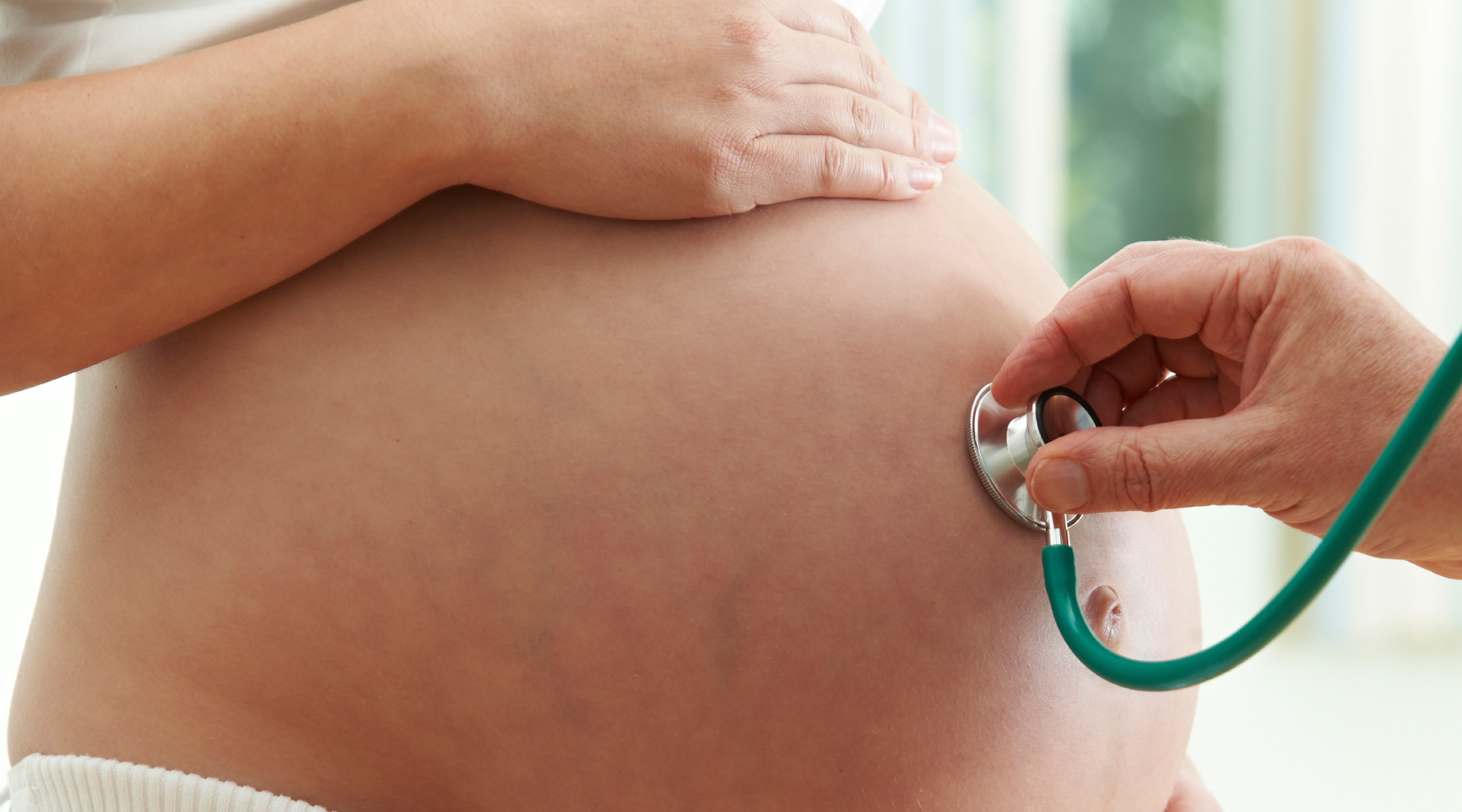
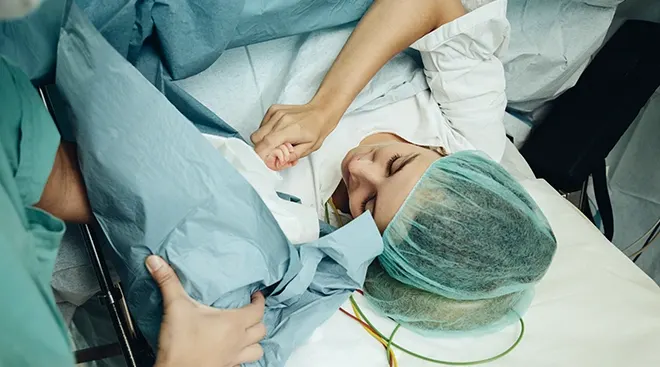
C-sections are on the rise. According to a new report by the Centers for Disease Control (CDC), 32.1 percent or 1 in 3 American babies are now born via c-section. Of this number, first-time c-sections have risen 4 percent from 2020-2021 to 22.4 percent, an all-time high since c-section data was collected. Because 4 out of 5 women who have a first-time c-section will go on to have another, the increase in this first-time rate means c-section rates overall are likely to increase in the future.
While the CDC and the World Health Organization (WHO) maintain that a c-section can be an essential and life-saving surgery, it can also put the lives of women and babies at unnecessary risk of short- and long-term health problems if performed when there is no medical need.
It can be challenging to discern precisely when c-section rates cross the line into unnecessary risk territory, but many consider the “ideal c-section rate” to be between 10-15 percent, almost half that of the United States. This percentage is gleaned from research by the WHO that shows maternal mortality goes down as countries move toward a 10 percent c-section rate, but when the rate goes over 10 percent, there is no evidence that death rates improve—so often, the risks outweigh the benefits.
Some of these c-section risks include the potential for heavy bleeding or infection, slower recovery times after childbirth, delays in establishing breastfeeding and skin-to-skin contact and increased likelihood of complications in future pregnancies.
Although there is no clear explanation for why c-section rates continue to increase, some suggest the increase comes from a lack of patient-doctor communication, poor education and even monetary incentives. Physicians are routinely paid more for a c-section than for a vaginal delivery—on average, about 15 percent more.
So what can we do to lower c-section rates and ensure mothers and babies aren’t put at unnecessary risk? While there are many suggestions, from decreasing c-section costs to requiring a second opinion on c-section decisions, the WHO believes quality, woman-centered care lies at the solution’s core.
“It’s important for all women to be able to talk to healthcare providers and be part of the decision making on their birth, receiving adequate information including the risks and benefits. Emotional support is a critical aspect of quality care throughout pregnancy and childbirth,” said Dr. Ana Pilar Betran, Medical Officer at WHO and HRP, in a statement.
To learn more about what to expect when getting a c-section, check out The Bump’s Truth About C-Sections article.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Navigate forward to interact with the calendar and select a date. Press the question mark key to get the keyboard shortcuts for changing dates.