The Lowdown on Using Pitocin During Labor
When it’s time to give birth, your body generally knows what to do. It’s programmed to release hormones that jump-start contractions and move your labor along. But childbirth doesn’t always go as planned. If your contractions stall or labor is slow to start (and baby really needs to come out), your doctor may recommend a Pitocin induction.
You may have heard some things about Pitocin—both positive and negative. The fact is: Pitocin can be incredibly useful to induce or augment labor, but, as with any drug, there are potential side effects and risks. Because Pitocin is a drug commonly used during labor, it’s important for you to better understand how it works, and what it could mean for your overall labor and delivery experience. So what is Pitocin, and why might you need it? Moreover, why do so many women have such strong feelings about this medication—and is it something you can or should try to avoid? Read on to learn everything you need to know about Pitocin, including its benefits and drawbacks.
According to the American College of Obstetricians and Gynecologists (ACOG), Pitocin is a brand name medication that replicates oxytocin, a natural hormone made by the body that produces contractions and stimulates labor.
When the hormone was first identified and synthesized in 1953 by an American scientist named Vincent du Vigneaud, it was hailed as a groundbreaking medical discovery. In fact, Vigneaud received the Nobel Prize in chemistry in 1955 for his work. “Up until the middle of the century, if a person stalled during labor, there was no good way to increase the intensity of the contractions and help them deliver,” says Barak M. Rosenn, MD, director of maternal fetal medicine at Jersey City Medical Center. At the time, the only option was to go straight to the operating room. “But now, as an alternative to performing a c-section, we have the ability to give this medication to start or strengthen the contractions.”
There are two reasons a doctor may use Pitocin during labor: to induce labor, if the health of Mom or baby is at risk, or to augment labor when contractions have already begun but aren’t moving quickly enough, creating a potential for infection and other problems. ACOG also notes some reasons for a Pitocin induction include a post-term pregnancy or problems with the placenta or amniotic fluid, among others.
Using Pitocin after delivery
Pitocin is also sometimes used after delivery. “You want the uterus to contract as firmly as possible to stop postpartum bleeding, and a larger dose of [Pitocin] can help do that,” Rosenn says. While post-delivery Pitocin isn’t necessary for every patient, it can be especially helpful for those who have developed an infection during labor. The uterus can become weak, and Pitocin puts pressure on exposed blood vessels to quell excessive bleeding.
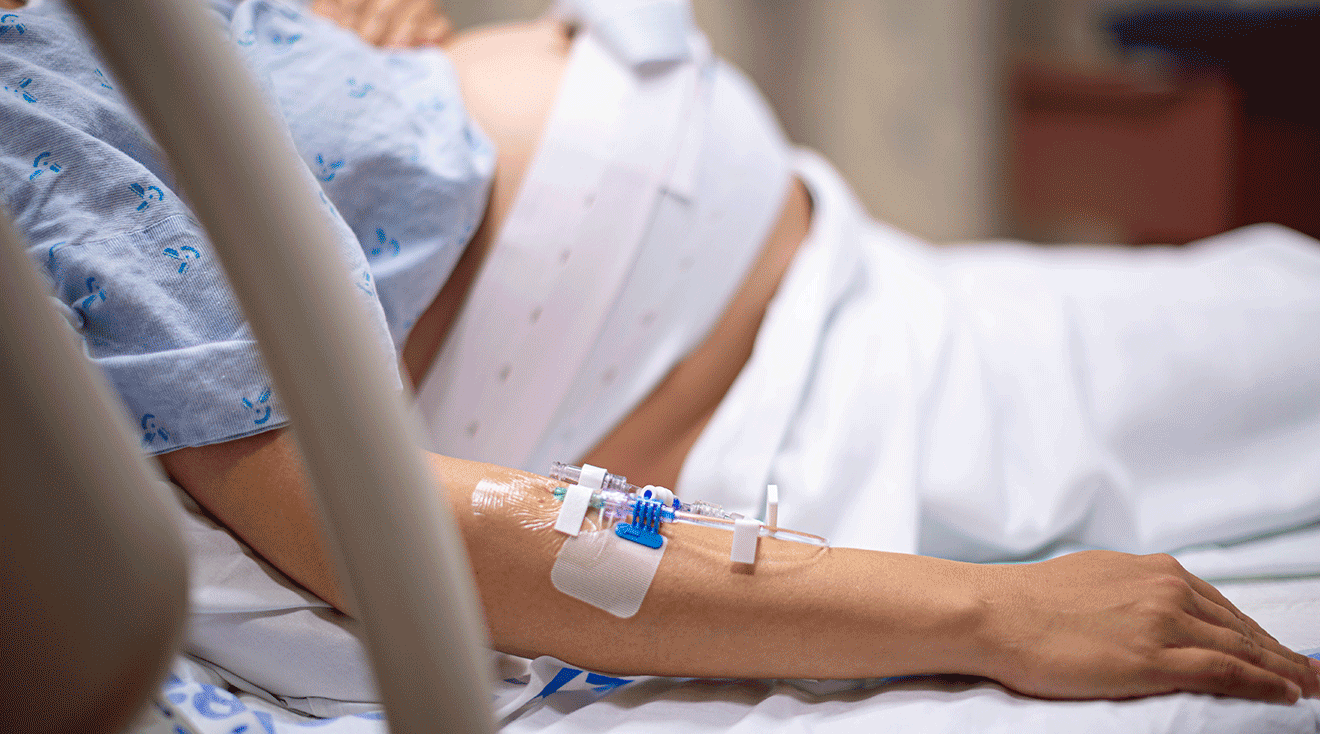
To induce labor, Pitocin is usually administered through an IV. The hormone binds to receptors in the uterus, which then activate the uterine muscles to encourage contractions. The contractions will gradually make the cervix dilate and then help to push baby through the birth canal.
While Pitocin induction triggers contractions, it works best “against a ripe cervix,” says Heather Bartos, MD, medical director at Be. Women’s Health and Wellness in Frisco, Texas. “A low Bishop score (which is a measure of cervical ripeness) generally won’t be changed by Pitocin.” This situation would typically call for the use of an oral or vaginal cervical ripening agent, such as Cytotec or Cervidil; these drugs work to thin and soften the cervix. Additionally or alternatively, your doctor may use a Foley bulb to speed things along. During this procedure, a balloon filled with saline is positioned against your cervix to promote ripening and help with dilation.
As for the Pitocin dosage used, it depends on the hospital you’re in and its protocols, but across the board, best practice is to start slowly—typically with 2 milliunits, Rosenn says. Sometimes, that initial dose is all it takes to induce labor. Generally, doctors will wait to see how you react and go from there, increasing the Pitocin dosage every half hour or so until you’re experiencing contractions that are about two to three minutes apart.
Wondering what the highest dose of Pitocin during labor is? Unfortunately, there isn’t a clear answer—it’ll vary for each person. “The highest dose of Pitocin that can be safely given varies for each individual and is determined by the healthcare provider based on factors such as the person’s medical history, the progress of labor and baby’s well-being,” notes Meleen Chuang, MD, an ob-gyn and medical director of women’s health at the Family Health Centers at NYU Langone.
Pitocin contractions
Like many other things, the pain level or contractions induced by Pitocin will vary from person to person. But you may have heard that a Pitocin induction leads to more intense labor contractions. While true labor contractions start in the back and move to the front, Pitocin contractions may feel more concentrated in the abdomen, Chuang explains. And though it’s difficult to assess objectively, many women do report more painful contractions with Pitocin. “It’s a common theme among [laboring people] as a drawback,” Rosenn says. “For someone who wanted to go into labor without regional anesthesia (or an epidural), Pitocin can make that more difficult.”
“Usually a person will feel mild contractions within the first hour, and then it varies from person to person in terms of when they become more intense,” says Geeta Sharma, MD, an ob-gyn and high-risk obstetrics specialist at Carnegie Hill ob-gyn practice in New York City. But another key factor in determining how successfully the Pitocin induction is working is how much the cervix is dilated—and how quickly dilation will occur after a dose of Pitocin varies. “It’s dependent on whether or not the mother has had previous deliveries and what the cervix is like—is it soft, has it begun to dilate? There’s a whole range of possibilities,” Rosenn says. “How long that takes depends entirely on the situation and on the person.”
Similarly, how quickly baby comes after a Pitocin induction can also vary widely. “It depends on various factors, including the body’s response to the medication, the stage of labor before starting Pitocin and other individual factors,” Chuang adds. “It’s important to note that labor induction with Pitocin can take several hours or even longer in some cases.”
“Pitocin can be beneficial in situations where there’s a medical need for labor induction or augmentation,” Chuang says, adding it may also reduce the need for a c-section. “However, it’s always important to discuss the potential risks and benefits of any medical intervention with your healthcare provider to make an informed decision based on your specific situation.”
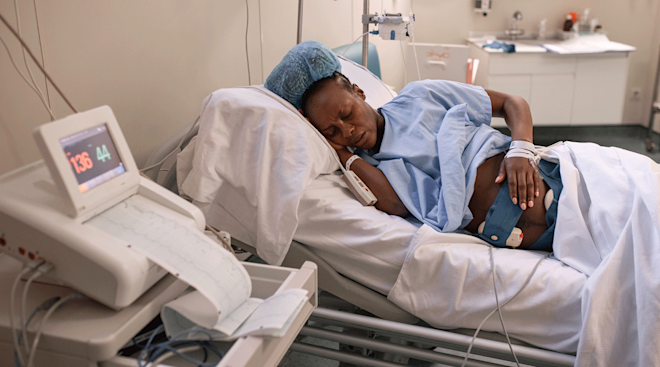
As with most medications, Pitocin may have side effects and can be dangerous if it’s not administered correctly. Pitocin brings on contractions, which are necessary for childbirth—but too many contractions in quick succession can actually harm baby. “Every time you contract, it squeezes the blood vessels, thereby decreasing the blood supply to the placenta,” Rosenn says, adding that “baby’s oxygenation is dependent on a good flow of maternal blood to the placenta.” So if you contract too often, the baby could be in danger—which is why you don’t want the contractions to be too frequent or too long. When baby’s oxygen supply is reduced, their heart rate may also begin to drop. This is why your medical team will watch you (and baby) closely during an induction. You’ll likely need to wear a fetal heart monitor throughout labor.
Other potential side effects and risks of Pitocin include:
- Uterine rupture. While extremely rare, Pitocin can lead to a rupture of the uterus or a tear in the uterine wall if the contractions are too intense. This can be dangerous for mom and baby. For those who’ve had a previous c-section and are trying to deliver vaginally, the risk of rupture is about 0.5 percent—but the use of Pitocin increases that risk to about 1.5 percent, Rosenn says. A person who has had a previous c-section can still receive Pitocin—they just need to recognize the risk and be in a hospital setting, so a doctor can monitor the situation and react to any changes. First-time moms and those who have had previous vaginal births need not worry: “The risk of rupture in those who never had a c-section is extremely low, even with use of Pitocin,” Rosenn says.
- Retention of fluid. “Another potential side effect is water intoxication,” Sharma says. “Pitocin is similar in its structure to ADH, an antidiuretic hormone, and in excess, Pitocin can cause water intoxication or retention of fluid.” Fortunately, this Pitocin side effect can be managed in a hospital setting.
- Increased chance of needing a c-section. Some research has indicated that an induction increases the risk of ultimately needing a c-section. On the other hand, though, a 2014 study found that c-section rate was actually lower among women who had full- or post-term inductions than those who were monitored by doctors and went into labor spontaneously at term or after their due dates. The reality is that a c-section may be necessary regardless of whether labor starts on its own or with an induction.
Over the years, Pitocin has developed a bit of a bad rap, and many may ask the question: Is Pitocin safe? “It’s one of the most feared medications among many [pregnant patients], because they often hear a lot of bad things about it—how it can increase the pain of contractions, how it can lead to c-sections, how it can be dangerous, etc.,” Rosenn says. “But what we have to remember is that it’s a naturally occurring hormone that has a role in labor itself. Without this hormone, women wouldn’t be in labor or progress with their labor.”
There are only two synthetic forms of oxytocin, Pitocin and Syntocinon, with Pitocin being more commonly used in the US. However, it’s not the only labor induction method that can be used. As mentioned, cervical ripening agents may also be used to help labor progress, as well as a procedure called an amniotomy, during which a provider artificially breaks the amniotic sac, notes ACOG. “Your healthcare provider will determine the most appropriate method based on your individual circumstances and the progress of your pregnancy,” Chuang says.
There have been several contradictory studies on whether a link exists between Pitocin and autism. According to research findings outlined in a 2016 report, people who received Pitocin during labor were 2.32 times more likely to have a child diagnosed with autism later in life. [However], the fact that not all children exposed to [Pitocin] later developed an autism phenotype suggests that there are other factors at play. The study also acknowledged that other publications have refuted these findings, and that, ultimately, more research is needed. In fact, a 2016 report in JAMA Pediatrics analyzed more than one million births, and found no link between the use of Pitocin and autism. Further, ACOG asserts there’s no evidence of a causal relationship between the two. “When considering Pitocin, it’s the last thing I would want someone to worry about,” Rosenn adds.
Pitocin induction might not sound ideal. But the truth is that the best laid labor plans—well, they might go awry. “Waiting for spontaneous labor may often be the best choice, but individualized, careful consideration and discussion with your obstetrician is always strongly recommended,” says Sharma. “You have to be willing to go with the flow. If baby is overdue, if you have a medical condition or if labor has come to a standstill, Pitocin might just be the catalyst your body needs to kick things into gear.”
The good news is that Pitocin is widely regarded as a safe and effective drug, and countless people receive it in the delivery room every day—even if some do lament its effects. If you have questions or concerns, speak with your doctor. Pitocin induction isn’t the only option, so you can always discuss other methods and weigh the alternatives together. And if you and your medical team determine that a Pitocin induction is necessary, you can feel empowered by your knowledge. There’s no one way to labor—and, with or without an induction, the end prize is a baby in your arms. You’ve got this.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, More From the Bump:
Heather Bartos, MD, is an ob-gyn and the medical director of Be. Women’s Health and Wellness in Frisco, Texas. A navy veteran, she spent 12 years serving the women and spouses of the armed forces, and was an associate professor at the Uniformed Services University of Health Sciences in Bethesda, Maryland. She completed her residency at Baylor College of Medicine, and earned her medical degree at The University of Texas.
Meleen Chuang, MD, is an ob-gyn and medical director of women’s health at the Family Health Centers at NYU Langone. She earned her medical degree from SUNY Stony Brook.
Barak M. Rosenn, MD, is the director of maternal-fetal medicine at the Jersey City Medical Center, a part of RWJBarnabas Health. Previously, Rosenn served as the director of obstetrics and maternal-fetal medicine at Mount Sinai West in New York City and a professor of obstetrics, gynecology and reproductive science at the Icahn School of Medicine at Mount Sinai. He received his medical degree from Hebrew University Hadassah School of Medicine.
Geeta Sharma, MD, is a board-certified ob-gyn and high-risk obstetrics specialist at Carnegie Hill ob-gyn practice in New York City. Previously, she was an assistant attending ob-gyn at New York Presbyterian/Weill Cornell Medical Center in New York City. She also completed her residency and fellowship there. Sharma earned her medical degree from Weill Cornell Medical College.
American Pregnancy Association, Inducing Labor, 2023
American College of Obstetricians and Gynecologists, Labor Induction, June 2022
Mayo Clinic, Labor Induction, May 2022
Canadian Medical Association Journal, Use of labour induction and risk of cesarean delivery: a systematic review and meta-analysis, June 2014
SAGE Publications Inc (American Society for Neurochemistry), Increased Risk of Autism Development in Children Whose Mothers Experienced Birth Complications or Received Labor and Delivery Drugs, August 2016
JAMA Pediatrics, Association of Labor Induction With Offspring Risk of Autism Spectrum Disorders, September 2016
American College of Obstetricians and Gynecologists, Labor Induction or Augmentation and Autism, 2021
Learn how we ensure the accuracy of our content through our editorial and medical review process.
Target Baby Registry
Free $100+ Value Welcome KitFree $100+ Value Welcome Kit
15% Completion Discount15% Completion Discount
Free 1-Year ReturnsFree 1-Year Returns
20+ Exclusive 20% Off
Deals For Mom & Baby20+ Exclusive 20% Off Deals For Mom & Baby1:1 Concierge With
Baby Gear Specialists1:1 Concierge With Baby Gear Specialists

*Subject to availability and Retailer's terms.
We earn commissions from these links.