Rh Incompatibility: What to Know if You’re Rh Negative and Pregnant
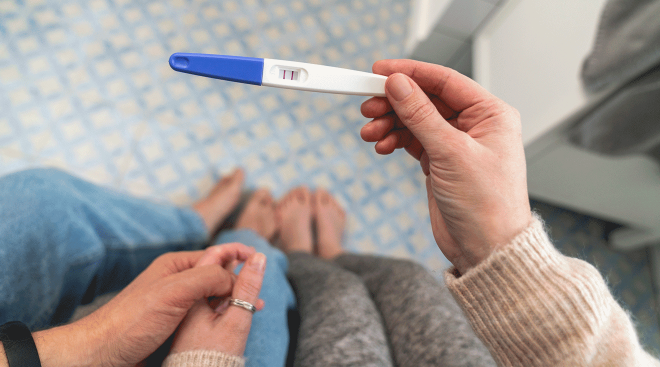
Unless you’re a frequent blood donor, you may have never given your blood type much thought. But if you have an Rh negative blood type, during pregnancy you may run into what’s known as Rh incompatibility, which is where you and baby have different Rh factors. What does all that mean, and how can it affect the healthy of your child? Keep reading to learn why you should pay attention to Rh factor in pregnancy and what precautions your doctor will want to take to keep you and baby safe.
Each person falls into one of four blood groups (A, B, AB or O) and also has an Rh factor designation (either positive or negative). These two combine to create a total of eight possible blood types: A+, A-, B+, AB+, B-, AB-, O+ and O-. So when we say someone’s blood is “negative,” we really mean it’s Rh negative.
Rh factor, or Rhesus factor, refers to a protein that can be found on the surface of red blood cells. Fun fact: “Rhesus” refers to rhesus monkeys, who also have the Rh factor gene.
“If your blood has the protein, you’re Rh positive, and if your blood lacks the protein, you’re Rh negative,” says Enchanta Jenkins, MD, an ob-gyn in private practice at Ellehcal OBGYN in Fallbrook, California. If your blood type is positive, Rh incompatibility won’t be an issue during your pregnancy. But about 15 percent of the total general population is Rh negative.
Your genetics determine your Rh factor status, and you inherit one gene from each parent. The gene for being Rh-positive is dominant, so it will prevail even when paired with an Rh-negative one. (The Children’s Hospital of Philadelphia has a helpful chart explaining when a baby will be definitely Rh positive, definitely Rh negative or has a chance of being either.) There’s a good chance that even if you’re Rh negative, baby may be Rh positive. And that’s when Rh incompatibility comes into play.
Rh incompatibility refers to the scenario where the mother is Rh negative and the baby is Rh positive. “Our bodies are programmed to reject foreign proteins, so if I was going to give someone a blood transfusion, I would make sure the blood is matched up to them,” says Victor A. Rosenberg, MD, an ob-gyn and maternal-fetal medicine specialist in private practice in Valley Stream, New York. During pregnancy, he explains, the mother is always going to have “fifty percent foreign material in her body,” due to the fact that half of the baby’s genes come from the father.
Most of the time, this isn’t an issue—but it can be when it comes to Rh factor. “This is one of the things that can get us into trouble during pregnancy, because if a mother is Rh negative and the baby is Rh positive, her body can recognize that D protein as foreign and react to it by making antibodies,” Rosenberg says. The process of making antibodies is known as developing Rh sensitization.
If both mom and baby are Rh negative, there won’t be any incompatibility. And mothers who are Rh positive also won’t experience problems, even if their baby is Rh negative.
There are no noticeable physical symptoms of Rh incompatibility, but if you’re Rh negative and your baby’s father is not, your doctor will want to perform titer tests to see if you’re making antibodies against potential Rh protein in baby’s blood. And if you’ve gotten pregnant using donated sperm, you will already know your donor’s blood type.
Rh incompatibility can pose a risk for your pregnancy if your body begins developing antibodies in response to baby’s Rh factor. Unfortunately, the antibodies that are designed to protect us can actually harm a developing baby. “Because fetal and maternal blood can mix during pregnancy, in some cases the maternal blood can develop antibodies that will cross the placental barrier and attack the fetal Rh positive red blood cells, leading to severe anemia in the baby and even death in some cases,” says Jenkins.
As Rosenberg says, “In order for a baby to function and thrive in utero, it needs blood in its body to nourish its organs and brain development. And if the baby has a low blood count, that can sometimes lead to significant complications.”
As a mom-to-be, you only need to be concerned about Rh incompatibility if you yourself are Rh negative. And even if baby’s father is Rh positive, that doesn’t mean baby will definitely be positive as well.
As Rosenberg explains, “This is where the genetics gets a little bit complicated in terms of whether Dad has one or two Rh positive copies. Because if he only has one Rh-positive copy, there’s only a 50 percent chance that he’s going to give it to the fetus.”
If he does have one of each, the other scenario would be that he passes on the Rh-negative gene, causing the baby to be Rh negative as well. (Remember, there is already an Rh-negative gene coming from Mom’s side.) But if he has two Rh positive copies, he is certain to pass one on, and since the Rh-positive gene is dominant, baby will be Rh positive. “There are blood tests we can do on Dad to figure out which one it is,” says Rosenberg.
Your risk for Rh sensitization increases during the pregnancies that follow your first one, usually because the potential for maternal and fetal blood mixing is highest during delivery. “With Rh antibodies, the body’s reaction to baby’s red blood cells can actually stay in the mother’s blood and then affect a subsequent pregnancy,” says Rosenberg. “Your body remembers those foreign red blood cells and now knows how to attack them.”
Other risk factors for Rh sensitization include:
- Vaginal bleeding
- Abdominal injury during pregnancy (such as from a fall)
- Chorionic villi sampling (CVS)
- Amniocentesis
- Miscarriage
- External version to turn a breech baby
There are a few different steps to determining Rh incompatibility and what level of risk it actually poses for your pregnancy.
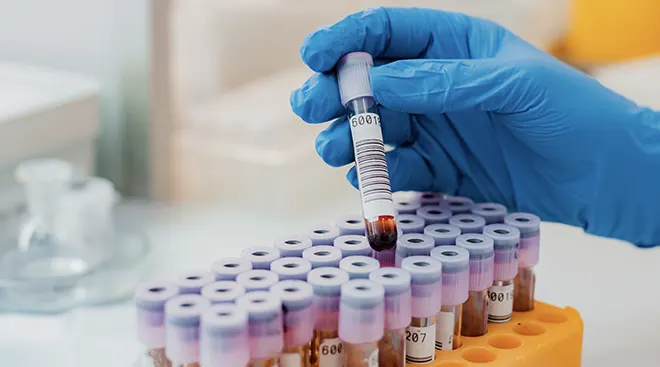
1. Your doctor will confirm your blood type. Many women begin pregnancy knowing their blood type, but if you don’t, your provider can tell you with a blood test.
2. Titer testing can determine if you’re making Rh antibodies, and how high the levels are. “If the levels are very low, the risk to baby is usually very small,” says Rosenberg.
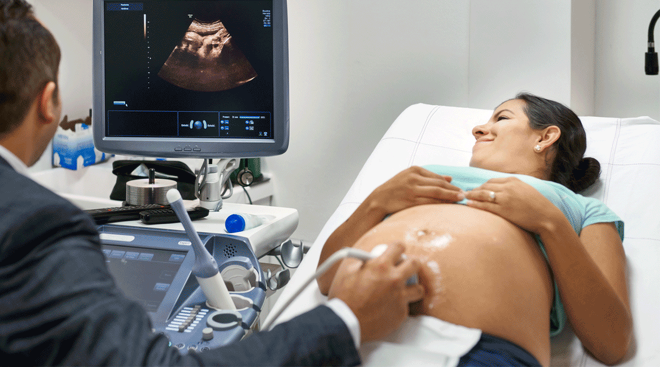
3. Fetal imaging can offer more information. If your doctor suspects an issue with your baby, perhaps because antibody titer levels have increased, a sophisticated ultrasound can be performed. “A high-level ultrasound with a maternal-fetal medicine specialist can measure baby’s blood flow to see if they’re becoming anemic or not,” says Rosenberg.
4. Baby’s blood type is confirmed. This can be done if you choose to have non-invasive prenatal testing (NIPT), otherwise it’s checked after delivery.
Doctors focus on preventing Rh sensitization from occurring in women who are Rh negative, and this is done by giving an injection of a medication called RhoGAM, which helps prevent your blood from making the antibodies that attack baby’s Rh-positive red blood cells. “In the United States, women who are Rh negative are routinely given RhoGAM,” says Rosenberg.
Jenkins calls RhoGAM “very effective” in preventing Rh sensitization. “It works by coating the fetal blood cells and essentially hiding them from the mom’s blood system,” she says.
Rh-negative women can usually expect to get their first RhoGAM shot during their third trimester, although this can vary depending on your specific situation. “Most physicians will treat all Rh negative moms with RhoGAM between 28 and 32 weeks of pregnancy, within 72 hours of delivery and anytime there is vaginal bleeding during pregnancy,” says Jenkins.
RhoGAM is also sometimes given to Rh-negative women when there’s a risk of blood mixing, such as after chorionic villi sampling (CVS), amniocentesis, miscarriage or an external version.
Although both doctors emphasized that treatment with RhoGAM is almost always effective, if fetal anemia is suspected, Rosenberg says that a blood transfusion can be given in utero. “We can do this with a needle through Mom’s belly and into baby’s umbilical cord using ultrasound guidance, and babies do extremely well with this,” he says.
Thanks to modern medicine, though, complications with Rh incompatibility are rarely an issue. “Patients should know that the RhoGAM really does work, Rosenberg says, “and even if they are Rh negative, they should rest assured that for the most part, pregnancies proceed normally.”
About the experts:
Enchanta Jenkins, MD, is an ob-gyn in private practice at Ellehcal OBGYN in Fallbrook, California, and is affiliated with Scripps Mercy Hospital in San Diego. She graduated from the Medical University of South Carolina and is a veteran of the United States Navy, where her 20 years of service included residency training at the Naval Medical Center.
Victor A. Rosenberg, MD, FACOG, is an ob-gyn and maternal-fetal medicine specialist. A graduate of Weill Medical College of Cornell University, he completed residency training in obstetrics and gynecology at New York Presbyterian Hospital-Weill Cornell Medical Center, followed by fellowship training in Maternal-Fetal Medicine at Yale University School of Medicine. Prior to launching his private practice, he was associate director of the Division of Maternal-Fetal Medicine at North Shore University Hospital.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Target Baby Registry
Free $100+ Value Welcome KitFree $100+ Value Welcome Kit
15% Completion Discount15% Completion Discount
Free 1-Year ReturnsFree 1-Year Returns
20+ Exclusive 20% Off
Deals For Mom & Baby20+ Exclusive 20% Off Deals For Mom & Baby1:1 Concierge With
Baby Gear Specialists1:1 Concierge With Baby Gear Specialists

*Subject to availability and Retailer's terms.
We earn commissions from these links.