A Comprehensive Guide to NIPT (Non-Invasive Prenatal Testing)
Parenthood is chock-full of surprises—that’s what makes it so exciting! And there’s much about your unborn baby’s future that’s unknown: The color of their eyes, whether they’ll have your dimples or your partner’s smile and what their first words will be. When it comes to your child’s health, however, surprises aren’t as welcome. But thanks to a screening method known as non-invasive prenatal testing (NIPT), doctors can give you a better idea of what the future holds for baby’s wellbeing. Plus, it can also determine baby’s sex with pretty high accuracy. “I had the test done, but it wasn’t to find out the sex. It was to give me some peace of mind and make sure baby was healthy. Finding out the sex was a perk though,” shares The Bump community member, tgortney.
Read on to learn from experts what the NIPT test looks at and whether it’s right for you and your family.
- There are several different prenatal genetic screening tests, including non-invasive prenatal testing (NIPT). NIPT helps identify the chances of baby having a chromosomal abnormality, such as Down syndrome, Edwards syndrome or Patau syndrome. This is a screening test and is not diagnostic.
- The screening looks for baby’s DNA in Mom’s bloodstream. Because there isn’t enough DNA until around week 10, for the most accurate results, it’s best to test after 10 weeks of pregnancy.
- Since it’s a blood test that looks at baby’s chromosomes, it can also reveal baby’s sex with 99 percent accuracy.
- The best candidates for NIPT are those who are 35 or older, have already had abnormal prenatal screenings or have a family history of genetic disorders.
- While your insurance may cover part of the NIPT if it’s deemed medically necessary, how much you’ll pay out of pocket will depend on your policy and individual risk factors.
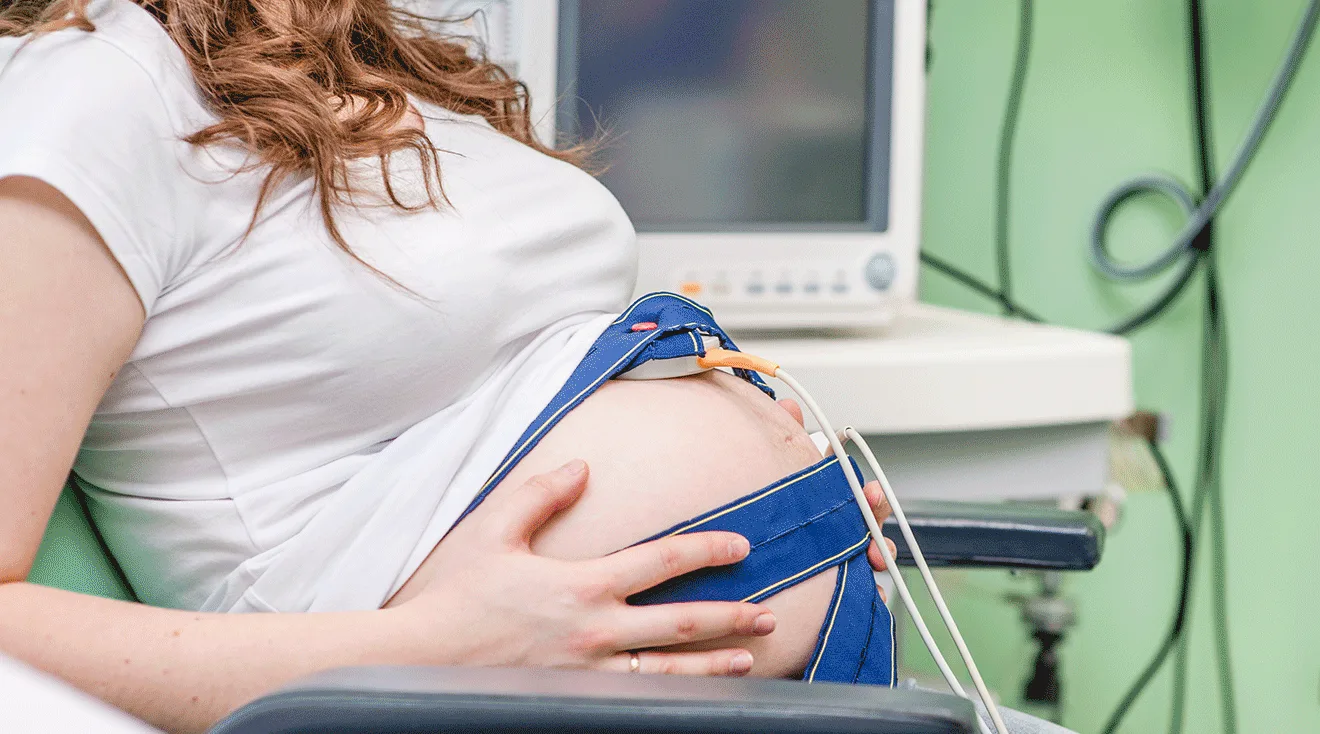
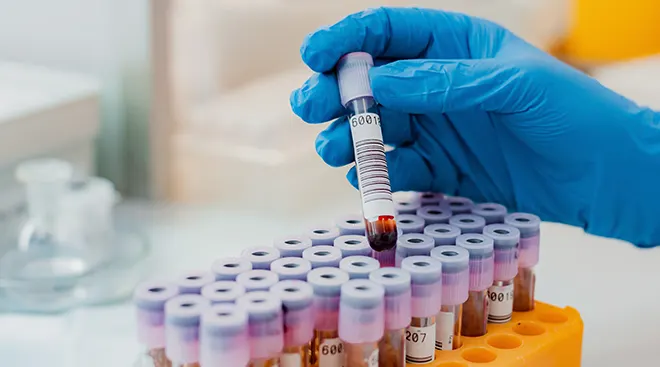
Non-invasive prenatal testing screens for chromosomal abnormalities in your developing baby. Unlike chorionic villus sampling (CVS) and amniocentesis (amnio)—which are prenatal tests that evaluate samples extracted from the uterus or placenta—NIPT is performed using a blood sample taken from the pregnant mother, per the American College of Obstetricians and Gynecologists (ACOG). Basically, it’s a simple blood test; this is why it’s considered “non-invasive;” NIPT poses no risk to Mom or baby.
NIPT analyzes tiny fragments of baby’s DNA in the blood, called cell-free DNA (cfDNA). Because Mom’s bloodstream contains a mix of cfDNA from her own cells as well as cells shed from the placenta, the screening is able to detect possible genetic abnormalities in baby’s cfDNA.
First, it’s important to emphasize that NIPT is a screening test—meaning it can tell you the chances of your child having a chromosomal abnormality. It can’t tell you definitively whether or not baby has an abnormality, per ACOG. (For that, you’d need to have a CVS or amnio.)
Different NIPT tests can screen for different chromosomal disorders, but most screen for trisomy 21 (Down syndrome), trisomy 13 (Patau syndrome) and trisomy 18 (Edwards syndrome), says Rachel Danis, MD, a reproductive endocrinologist and infertility specialist with RMA of New York, adding, “Trisomy is having three copies of a chromosome,” as opposed to the normal two copies most people have.
Additionally, some tests might screen for:
- Trisomy 16
- Trisomy 22
- Triploid syndrome—this occurs when baby is born with an extra set of chromosomes in their cells
- Sex chromosome aneuploidies—this occurs when baby is born with an abnormal number of sex chromosomes, which can lead to disorders such as Turner syndrome and Klinefelter syndrome
- Disorders caused by chromosomal deletion, like Prader-Willi syndrome
- Single gene disorders
Doctors typically recommend NIPT testing for women whose pregnancies are considered high-risk for a chromosomal abnormality, says Katelynn Sagaser, MS, CGC, a certified genetic counselor and genomic health education manager with 23andme.
She notes the pregnancy might be considered high-risk if:
- The mother (or egg donor) is 35 or older
- The woman has already had an abnormal prenatal screening result
- A fetal abnormality was detected on a sonogram
- One parent has a chromosomal abnormality
- The mother has had a previous pregnancy with a chromosomal abnormality
That said, all women at any age have a chance of having a baby with a birth defect or abnormality, which is why many moms-to-be who don’t fall into these buckets say yes to non-invasive prenatal testing.
On the flip side, women with high-risk pregnancies may decide against the screening test if they feel the results won’t help them. “As parents-to-be consider the option of NIPT, they may want to first spend some time reflecting on what kind of information is helpful and empowering to them during their pregnancy,” Sagaser says. “The term ‘healthy baby’ has different meanings to different people, and NIPT may give parents more or less information than they want regarding the health of their little one.”
Typically, the test isn’t performed until at least week 10 of pregnancy. That’s because before that point, there may not be enough cfDNA from the placenta in the mother’s bloodstream to identify fetal chromosomal abnormalities, explains the Cleveland Clinic. Results are usually available in 8 to 14 days.
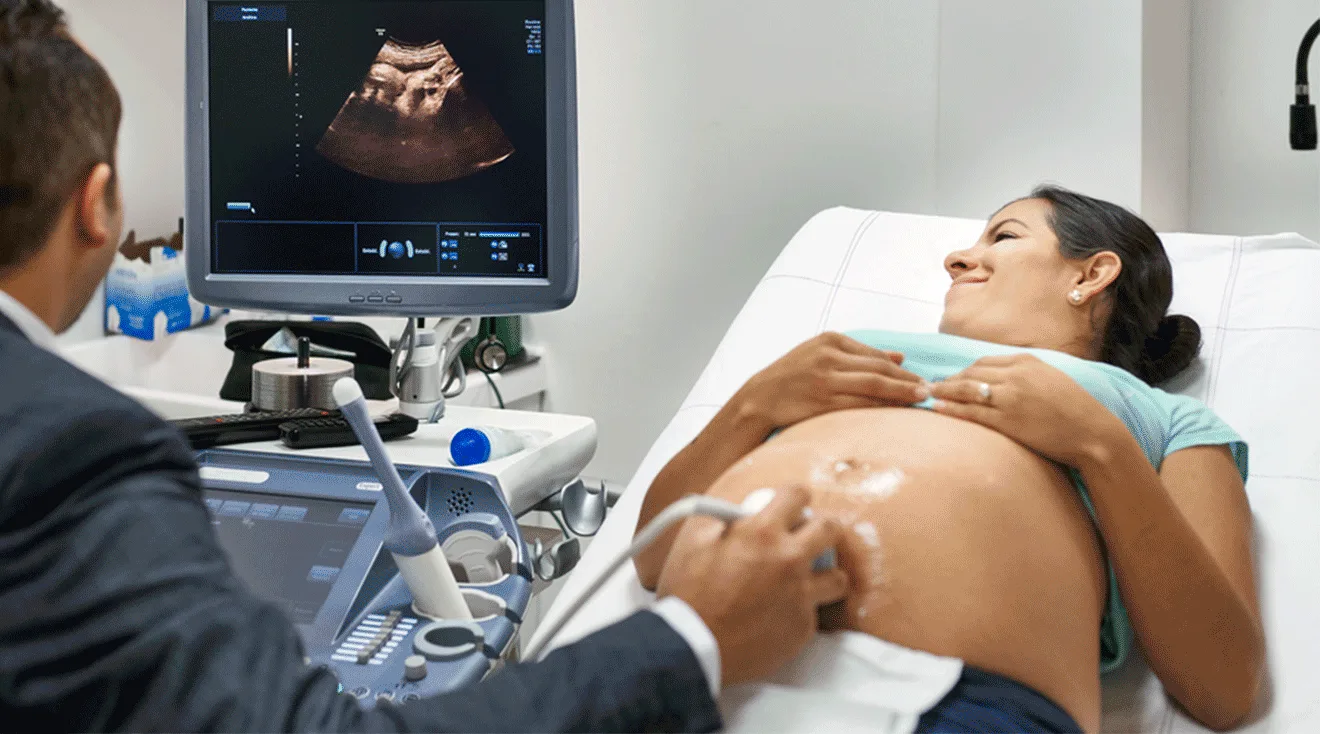
While it’s not the primary purpose of NIPT, because the test analyzes baby’s DNA, your NIPT test results can also tell you the sex of your child. That means parents who choose to do NIPT testing can find out if they’re expecting a boy or girl around 11 or 12 weeks of pregnancy, instead of waiting for the 20-week ultrasound. “I’m very anxious to know what I’m having and am too impatient to wait for the anatomy scan,” says knottie920aa1de8b27319b, a community member on The Bump.
NIPT test accuracy depends on what you want to learn from the test. There’s a 99 percent chance that Down syndrome will be detected by NIPT. “While NIPT is a very good screening test for trisomy 21 (Down syndrome) and trisomy 18, it’s not nearly as good for trisomy 13 and sex chromosome abnormalities,” says John Williams, MD, director of reproductive genetics service at Cedars-Sinai Medical Center in Los Angeles. Some studies, however, have shown the detection rate for trisomy 18 and 13 to be around 99.3 percent and 97.4 percent, respectively.
“It’s important to understand that NIPT is not a diagnostic test, and can have false positive results, false negative results and possibly more confusing results,” Sagaser says. The false positive rate (when the test incorrectly detects a condition) for trisomy 21, 18 and 13 is small—less than 1 percent—but parents-to-be should be aware that the test has limitations, and that certain factors can increase the chance of an inaccurate or failed reading.
NIPT testing may be less effective if you:
- Are pregnant with twins or multiples
- Are obese
- Used a donor egg to get pregnant
- Are less than 10 weeks pregnant
- Are taking certain blood thinners
I'm really glad we did the NIPT (followed by the nuchal translucency test soon after), as this early testing gave me a lot of peace of mind. It also allowed us to find out the sex of our baby at 10 weeks—and as far as I'm concerned, when it comes to pregnancy, the earlier you have the information, the better!
Because non-invasive prenatal testing is generally very effective, a normal result can be a massive relief for parents-to-be. They may decide to opt out of future CVS and amnio diagnostic testing, since both tests carry a slight risk of miscarriage. “If a parent receives normal results from NIPT, there’s a very low chance—usually less than one percent—that their baby would later be diagnosed with one of the conditions included on the NIPT,” Sagaser says.
A positive result, on the other hand, can also be empowering for moms- and dads-to-be. Some parents might benefit from learning more about the condition, preparing to raise a child with a health issue or disability, making different plans for the pregnancy or starting possible treatment sooner after birth, Sagaser says.
NIPT testing is non-invasive, so there are no physical risks for Mom or baby, but it’s possible for NIPT to cause emotional anxiety. “Some people may feel the chance of a false positive result—or even the wait for the screening result can cause significant stress and worry,” Sagaser says. It’s something to consider when deciding if the NIPT test is right for you and your family. If you’re unsure, talk to your doctor or genetic counselor.
Remember: NIPT is a screening test, not a diagnostic test. A positive result doesn’t mean baby will 100 percent be born without a chromosomal disorder, and a negative result isn’t a guarantee your child will be born without a genetic or chromosomal abnormality. That’s why it’s important for expectant parents to avoid making big decisions based on NIPT results alone. “If you get a positive NIPT screening, you should definitely have diagnostic testing to confirm the findings,” such as CVS or amnio, Williams says. Plus, reach out to your doctor to get more information on your results and the best next steps to take.
NIPT has become more readily available to pregnant women since it was first introduced, but the cost will ultimately depend on your insurance plan. “When a pregnant patient has a medical indication for NIPT, most insurance policies contribute to the cost of the test,” Sagaser says. But if your insurance company doesn’t cover NIPT, many laboratories have flexible programs that can help with the cost of NIPT, which can range from $800 to $3,000. If you have any questions about what you’d pay for an NIPT test, ask your doctor’s office to direct you to the NIPT billing team. They should be able to provide you with an estimate.
There’s no one right answer! You may have heard about certain branded NIPT tests, such as the Harmony test and Panorama test. When figuring out which is the best NIPT test for you, your doctor will take certain factors into account, including your age, weight, whether an egg donor was used, what the test screens for (different tests may screen for different abnormalities) and which tests are covered by your insurance. Together, you and your doctor—or your genetic counselor—can determine which NIPT test is best for you and your pregnancy plan.
Just had the NIPT draw yesterday. Hopefully this round isn't as slow as it was for our last pregnancy (16 days!). My OB doesn't do the NT scan in conjunction with the NIPT. I thought this was fairly normal, but I’m seeing many more people saying they had both. Anyone else only have the NIPT? I kind of would like another ultrasound!
Frequently Asked Questions
How do you prepare for NIPT?
The first step in preparing for the NIPT is understanding what it actually does and that it’s a screening rather than diagnostic test. It’s critical to understand what exactly it screens for and the factors that may affect the results’ accuracy, such as maternal obesity or a multiples pregnancy, says Danis. “It’s also important to counsel patients on the pros and cons of getting this screening test,” as well as preparing them for the possibility of a positive result signaling a chromosomal abnormality. Preparing for something like this can be hard—and there’s no one right way to do it—but the best thing you can do for yourself, baby and your family is to get all the facts straight and arm yourself with the knowledge of what could be coming your way. In terms of physical preparation, there’s nothing you need to do.
What conditions does NIPT screen for?
As noted, NIPT tests screen for chromosomal abnormalities, such as Down, Edwards, Patau and triploid syndromes, as well as genetic abnormalities, such as trisomies 16 and 22, among other conditions.
Do I need to do both NIPT and NT?
The nuchal translucency screening (aka NT Scan) is another prenatal genetic screening test that offers complementary information on baby’s risk of chromosomal abnormalities. It looks at the folds on the back of baby’s neck via ultrasound. When combined with an additional blood test, the NT becomes part of the first trimester screening.”
All this to say, there are a few different options for prenatal genetic screening tests, but NIPT is usually the standard protocol, says Kendra Segura, MD, a a California-based ob-gyn. That said, if the results of your NIPT are abnormal, it may be followed by an NT. It also depends on your specific practice; some ob-gyns order both NIPT and NT for all patients.
Can NIPT tell me baby’s sex?
NIPT can accurately tell you baby’s sex. In fact, studies have found a 99 percent accuracy rate when it comes to fetal sex determination, particularly closer to 10 weeks pregnant.
Can NIPT detect the wrong sex?
While NIPT detects baby’s sex with 99 percent accuracy, as is true with any test, there’s always a small chance it could be wrong.
Is NIPT covered by insurance?
Unfortunately, there isn’t one answer here, as it’ll depend on your individual insurance plan, Danis says. In cases where it’s medically necessary (i.e. for people over 35, with a history of a trisomy, etc.), your insurance may cover it but require prior authorization, ACOG notes.
How much does NIPT cost without insurance?
Unfortunately, there’s no clear answer here either, as it will depend on various factors, including any partial coverage costs, the medical necessity of the test and more. While ACOG believes that insurance policies shouldn’t be a barrier to prenatal care, there’s more work to be done. Based on your policy and circumstances, NIPT without insurance may cost anywhere from a few hundred to over a thousand dollars.
Is exactly 10 weeks too early for NIPT?
Exactly 10 weeks isn’t too early for NIPT. Per the Cleveland Clinic, by 10 weeks of pregnancy, there is enough fetal DNA in your blood to provide accurate NIPT results.
What happens if my NIPT test is too early?
If your NIPT test is too early, there may not be enough fetal DNA in your blood, resulting in an inaccurate NIPT result that could be a false positive or a false negative. For this reason, it’s best to wait until at least 10 weeks to test.
What is a good fetal fraction for NIPT?
According to studies, the fetal fraction represents how much of baby’s DNA (cfDNA) is in Mom’s bloodstream. The fraction can range anywhere from 4 percent to over 30 percent, the study notes. It will increase with gestational age, but can also be affected by factors such as maternal BMI, a multiples pregnancy and more. While there’s no specific number, a good fetal fraction will be on the higher end, as this provides more confidence in the accuracy of the final result, experts note.
What does a low fetal fraction mean?
A low fetal fraction could mean many things. According to Medline Plus, it could mean that it was too soon to test, there was a sampling error, a factor such as maternal obesity is affecting the result or there’s a fetal abnormality present.
What is considered a high risk of Down syndrome?
Per UT Southwestern Medical Center, baby is at a greater risk of Down syndrome if Mom is older than 35 years old during the pregnancy or if there’s a genetic history of it in the family. A low fetal fraction on your NIPT may indicate a higher risk of baby having Down syndrome or another chromosomal abnormality.
Facing prenatal genetic screening tests—whether it’s the NIPT or another one—can be scary. Many people opt for the NIPT due to its non-invasive nature, but it’s important to prepare yourself for the results. The best way to do this is to talk to your healthcare provider or genetic counselor on your goals for the NIPT. They can help you assess whether the test is right for you or whether it would be better skipped.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Rachel Danis, MD, is a reproductive endocrinologist and infertility specialist with RMA of New York. She also serves as an assistant clinical professor in the Department of Obstetrics, Gynecology and Reproductive Science at Icahn School Medicine at Mount Sinai. She earned her medical degree from Drexel University College of Medicine and completed her residency at Hahnemann University Hospital at Drexel University.
Katelynn Sagaser, MS, CGC, is a certified genetic counselor and genomic health education manager with 23andMe. Previously, she specialized in prenatal and preconception genetics at the Johns Hopkins Hospital in Baltimore, Maryland, as well as served as an assistant professor of gynecology & obstetrics in the Division of Maternal-Fetal Medicine.
Kendra Segura, MD, MPH, FACOG, is a Los Angeles-based board-certified ob-gyn, as well as an entrepreneur, author, motivational speaker and cast member of Bravo’s hit TV series Married to Medicine: Los Angeles. She earned her medical degree at Ross University School of Medicine in 2011 and completed her residency at Rochester General Hospital in Rochester, New York.
John Williams, MD, is the director of reproductive genetics service at Cedars-Sinai Medical Center in Los Angeles. He earned his medical degree from UCLA and completed his residency at University of California, Los Angeles.
American College of Obstetricians and Gynecologists, Cell-Free DNA Prenatal Screening Test, 2025
American College of Obstetricians and Gynecologists, Non-Invasive Prenatal Testing, 2025
Cleveland Clinic, NIPT Test, October 2022
BMJ Open, Accuracy of non-invasive prenatal testing using cell-free DNA for detection of Down, Edwards and Patau syndromes: a systematic review and meta-analysis, January 2016
Knowledge Centre for the Health Services at The Norwegian Institute of Public Health, Non‐Invasive Prenatal Testing (NIPT) for Fetal Sex Determination. Health Technology Assessment, December 2016
Norwegian Institute of Public Health, Non-invasive prenatal testing (NIPT) for foetal sex determination, December 2016
American College of Obstetricians and Gynecologists, Payer Coverage Overview, 2025
Current Genomics, Non-invasive Prenatal Testing in Pregnancies Following Assisted Reproduction, November 2022
Prenatal Diagnosis, Fetal fraction and noninvasive prenatal testing: What clinicians need to know, March 2023
Medline Plus, What is noninvasive prenatal testing (NIPT) and what disorders can it screen for?, July 2021
UT Southwestern Medical Center, How the Down syndrome test works and tips for making your decision, March 2015
Learn how we ensure the accuracy of our content through our editorial and medical review process.
Target Baby Registry
Free $100+ Value Welcome KitFree $100+ Value Welcome Kit
15% Completion Discount15% Completion Discount
Free 1-Year ReturnsFree 1-Year Returns
20+ Exclusive 20% Off
Deals For Mom & Baby20+ Exclusive 20% Off Deals For Mom & Baby1:1 Concierge With
Baby Gear Specialists1:1 Concierge With Baby Gear Specialists

*Subject to availability and Retailer's terms.
We earn commissions from these links.