3D Ultrasound: Why It’s Used and What You Can Expect to See
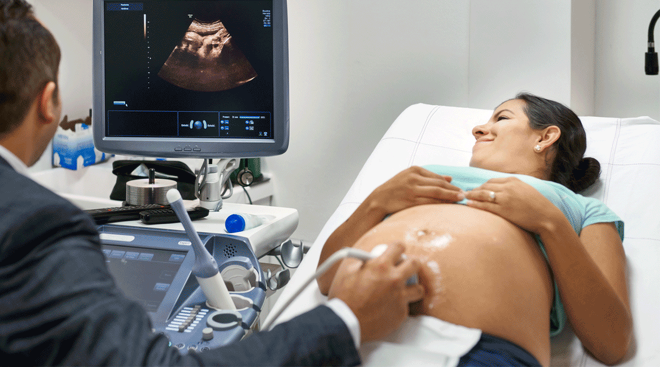
Perhaps the most exciting thing about a prenatal checkup is the ultrasound—after all, it lets you see with your own eyes that the pregnancy is real, and, as your pregnancy progresses, it allows you to watch your baby grow. Typically, the ultrasound will be of the 2D variety, but at times, your doctor may offer a 3D ultrasound. (And soon enough, you may be hit with ads advertising non-medical 3D scans.) So what is a 3D baby ultrasound, and how does it compare to a 2D ultrasound? We talked to experts to provide the lowdown.
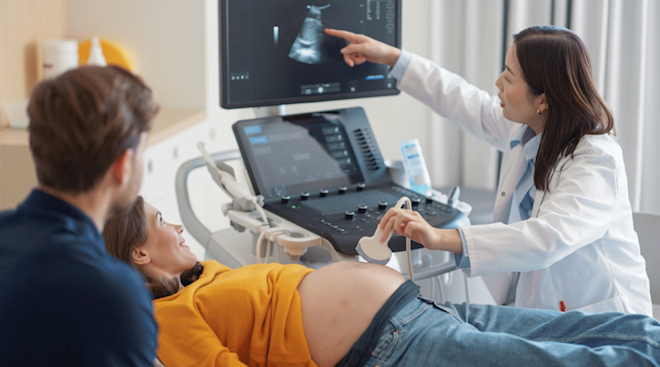
Fetal ultrasounds are tools for monitoring baby’s development and tracking your pregnancy. These ultrasounds, including 3D ultrasounds, work fundamentally the same way. During the exam, your doctor or technician moves an ultrasound transducer along your skin. This sends high-frequency sound waves into your body, putting them into contact with tissues, bodily fluids and bones (yours and baby’s). The waves then bounce back like an echo, and the transducer turns them into images. How those images appear on the screen is, in large part, what distinguishes a 3D baby ultrasound from a 2D or 4D ultrasound.
2D vs. 3D ultrasound
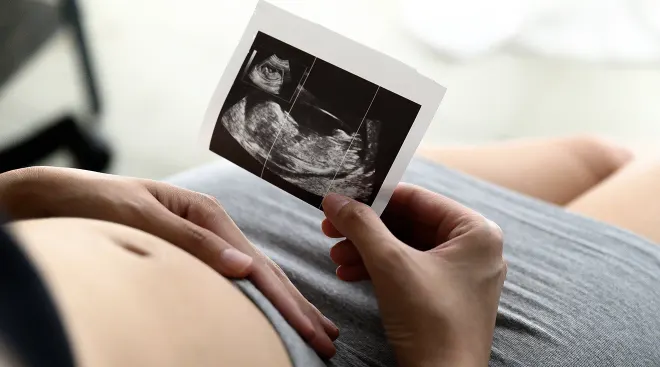
As its name suggests, a 2D ultrasound produces images that appear in two dimensions, while a 3D ultrasound creates those in three dimensions. A 3D baby ultrasound captures multiple 2D images and assembles them together. 3D ultrasounds build volume, says Gloria A. Bachmann, MD, associate dean for women’s health at the Rutgers Robert Wood Johnson Medical School in New Jersey—and in doing so, it breathes life into flat images. So, for example, instead of that classic sonogram profile shot of baby, 3D ultrasound pictures can offer a look at baby’s full, smooshy little face. (How amazing is that?)
A 2D ultrasound is typically standard practice and, under usual circumstances, it could be all you need, at least from an imaging standpoint, to track a healthy pregnancy. For instance, in the first trimester, a scan can confirm the pregnancy, show whether you’re carrying multiples and provide an estimation of your due date. In the second trimester, when baby is further along, a 2D ultrasound can reveal more anatomical detail and therefore the gender, position in the womb and whether something doesn’t seem right.
In contrast, a 3D ultrasound is not typical protocol and isn’t as widely covered by insurance as the 2D scan, especially if it’s not medically necessary. Often, doctors order a 3D ultrasound to take a closer look at why a pregnancy may not be progressing as expected. By showing more depth, dimension and contour, the scan can help them confirm the existence of a suspected condition, such as a birth defect, and evaluate the extent of it. Because three-dimensional images are easier to interpret for expectant parents than two-dimensional ones, 3D ultrasounds also help support patients in attaining a better understanding of any such issues affecting their pregnancy.
3D vs. 4D ultrasound
A 4D ultrasound is a 3D ultrasound with movement—in other words, a video of your baby, kicking, stretching, thumb-sucking and doing all sorts of other adorable things. “It generates the image in real time,” says Priya Rajan, MD, medical director of ultrasound in the division of maternal-fetal medicine at the Northwestern University Feinberg School of Medicine in Chicago.
Doctors are then able to, for instance, look at how the heart is beating and how the blood is flowing. However, in the vast majority of cases, these 4D ultrasounds are not medically necessary—doctors can find what they need with a 2D or 3D scan. As a result, you’ll more likely find 4D ultrasounds being offered at keepsake-type imaging centers than your typical medical practice.
More often than not, the 2D ultrasound is the only kind of scan a doctor needs to track your pregnancy. But a 3D ultrasound can come in handy in certain situations. Think of it as a supplemental tool in your doctor’s prenatal-care kit when:
• Your 2D ultrasound raises questions. If doctors see something suspicious on the 2D ultrasound, such a facial abnormality, they may perform a 3D ultrasound. By zeroing in on an area in question and seeing it with more depth and dimension, they can then better evaluate a particular condition. For instance, Rajan says, in the case of a cleft lip, you see the surface of the face and the nature of a split. In addition, since 2D scans are usually difficult to understand, a 3D scan can serve as a way to better explain the situation with the patient. (3D ultrasounds, however, are not normally used for a gender reveal. The sex of the baby can usually be discerned with a 2D ultrasound.)
• You have a high-risk pregnancy. Women with pre-existing health conditions, such as heart disease or diabetes, older moms or those who had complications in an earlier pregnancy may get more ultrasounds; in some cases, one of those scans may be a 3D ultrasound, which provides more information on spatial orientation. This can be helpful in assessing, for instance, the position of the placenta and planning any appropriate interventions if need be. (A 3D ultrasound shouldn’t be known as a “Down Syndrome ultrasound”; this condition is better assessed with a blood test or an amniocentesis—tools that are “far superior,” says Rajan).
With multi-dimensional imaging, doctors can more fully understand the spatial relationships of the anatomical parts they’re looking at and better evaluate a particular condition, such as:
• Facial anomalies. Cleft lip is one example. In this condition, the tissue from each side of the head doesn’t join completely at the lip, leaving a gap. While a 2D scan may indicate the issue, a 3D scan offers a better view of the extent of the split.
• Congenital heart disease. A 3D ultrasound makes it easier for doctors to interpret scans of the fetal heart anatomy. Depending on the technology used, a 3D baby ultrasound can even explore how the heart correlates with the vessels and structures around it.
• Neural tube defects. The neural tube eventually becomes a baby’s brain and spinal cord. A defect occurs when it doesn’t close up or when it develops outside the body. With 3D ultrasounds, doctors can take a closer look at the brain and body from different planes and evaluate the extent of the defect.
• Placental issues. 3D ultrasounds not only provide an image of the placenta, but, depending on the technology used, they can also help assess its vascularization, volume and blood flow. A 3D scan can also look at the placenta’s placement with respect to the womb, particularly in conditions like placenta accreta, where the placenta grows too deeply into the uterine wall.
In the hands of a trained medical professional, 3D ultrasounds are generally safe. Because it’s based on non-ionizing radiation as opposed to the ionizing sort found in X-rays, you and baby won’t be exposed to the same dangers as you might with an X-ray.
Still, Rajan points out, “there can be risks.” Namely, the ultrasounds do generate heat and can cause the tissues to subtly warm up. This can sometimes cause small pockets of gas in tissues and body fluids. Whether this is harmful or not in the long term is unknown. That’s why, Rajan says, it’s so crucial to get your ultrasound from someone who is medically trained in the field. Medical professionals should adhere to the ALARA principle: As Low As Reasonably Achievable. This means using the lowest level of power on the machine as possible, and taking as little time as possible, to attain the necessary images.
The best time for a 3D ultrasound depends on your particular circumstances and when your doctor feels that it’s necessary. In general, 3D baby ultrasounds produce the best images between 28 and 30 weeks, “when you can see fat on baby’s cheeks,” explains Michael Cackovic, MD, a maternal-fetal medicine physician at The Ohio State University Wexner Medical Center, in Columbus. Before then, baby is usually not developed enough to take full advantage of the 3D technology. For instance, there may not be enough soft tissue and the baby could look skeletal. At the same time, past the 30 week mark isn’t ideal either. As baby grows larger, it can be difficult to get a good 3D image.
Keepsake 3D ultrasounds are “entertainment” ultrasound procedures performed outside the doctor’s office. Often touting the latest technology in a “relaxed” atmosphere, these commercial ventures promise amazing images and video footage of your unborn child.
Don’t be tempted. Medical professionals are wary of them, and the Food and Drug Administration warns against them. Connecticut has even banned their use, and California requires that people getting keepsake ultrasounds be provided a written warning about the risks.
“Any ultrasound—including 3D ultrasound—is a medical procedure, plain and simple,” Cackovic says. “It should be used only in the hands of trained professionals.” Medical providers understand the unknown risks of heat exposure via ultrasound, and therefore keep the session as short as possible. But as the FDA points out, because the primary goal of these commercial places is to provide “good pictures,” they may expose you and baby to unnecessary heat for extended periods of time. “When you’re putting it in the hands of someone who is selling a product, they don’t know when to say enough,” Cackovic says. “There’s no organizing body to make sure they’re using the right settings.”
Unlike ultrasounds performed in a medical office for a medical reason, keepsake ultrasounds are not covered by insurance. If you have questions about 3D ultrasounds, talk to your doctor, who can then offer guidance that’s best for you and baby.
About the experts:
Gloria Bachmann, MD, is a professor in the department of obstetrics, gynecology and reproductive sciences. She also serves as associate dean of women’s health at Rutgers Robert Wood Johnson Medical School and director of the Rutger’s RWJMS Women’s Health Institute.
Priya Rajan, MD, is the medical director of ultrasound in the division of maternal-fetal medicine at the Northwestern University Feinberg School of Medicine in Chicago. She is a double board-certified ob-gyn and maternal fetal health specialist. Rajan earned her medical degree from the University of North Carolina School of Medicine in 2001.
Michael Cackovic, MD, is an ob-gyn specializing in maternal fetal medicine at the Ohio State University Wexner Medical Center in Columbus. He earned his medical degree from Hahnemann University College of Medicine in 1997.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Navigate forward to interact with the calendar and select a date. Press the question mark key to get the keyboard shortcuts for changing dates.