Your Complete Guide to Prenatal Testing
From the moment you find out you’re pregnant until the day you give birth, there will be plenty of milestone moments (baby’s first kick! Your first maternity bra!). There will also be many, many doctor visits, since keeping up with your prenatal testing schedule is crucial to the health of you and your growing baby. Fortunately, the vast majority of tests are quick and painless.
Start by talking with your OB about a prenatal testing schedule that fits your needs. Some tests are a routine part of your prenatal checkups; others are voluntary, available only if the doctor thinks they’re helpful in your particular circumstance and only if you want them. “There are lots of different options, so you should discuss with your provider which ones to go by,” says BreAnne N. Huss, a certified nurse midwife and women’s health nurse practitioner at Kootenai Health in Coeur d’Alene, Idaho. Before you do, familiarize yourself with what’s in store for the next nine months, so you can come prepared with questions.
Prenatal testing refers to the series of assessments performed over the course of your pregnancy. Your provider performs these tests through a variety of methods, says Julie A. Romero, MD, a maternal-fetal medicine specialist at Maternal Fetal Medicine Associates in New York City. They can include blood work, vaginal swabs, invasive genetic testing, ultrasounds and electronic fetal heart monitoring.
Some prenatal tests are considered routine and are typically performed in every pregnancy. These tests monitor baby’s progress and make sure you’re healthy and in good shape for carrying baby until she’s ready to come out; they also let you know if your doctor needs to adjust your care to accommodate for any special conditions.
Other tests are optional, depending on the parents’ preferences, or offered only to high-risk women. Voluntary tests often include those that predict or determine whether baby will have any birth defects or genetic disorders.
Prenatal tests are often categorized as either “diagnostic” or “screening.” A diagnostic test will provide a diagnosis of a condition with at least 99 percent certainty. A prenatal screening test will merely let you know if you’re “high risk” or “low risk” for a condition.
Thanks to advancements in medicine and technology, you have more choices for prenatal testing than ever before—and the menu of options changes quickly, notes Mary Norton, MD, professor of obstetric gynecology and reproductive sciences at University of California San Francisco. For instance, cell-free DNA—a noninvasive method of prenatal genetic testing that’s more accurate for certain conditions than earlier screens—started being offered to moms-to-be only a few years ago. That said, it’s always smart to stay up to date; here are the latest prenatal testing options available.
Prenatal testing in the first trimester confirms the viability of your pregnancy and makes sure it’s off to a healthy start.
Carrier testing
This type of prenatal testing involves a blood test that evaluates the parents—not the baby—to determine whether you and your partner may be carriers of any hereditary diseases. For the baby to be at risk, both Mom and Dad would need to test positive for a genetic disorder. If prenatal DNA testing determines that the mother is a carrier, then a prenatal paternity test may be recommended. While carrier testing is offered early in pregnancy, you can have the tests done even before you get pregnant. “You can have pre-conception counseling to discuss age-based and genetic risk with a certified genetic counselor,” says Jennifer Wright-Bennion, a certified midwife and advanced practice registered nurse at Banner Medical Group in Queen Creek, Arizona. If you and your partner are already aware of hereditary diseases, you can discuss those too.
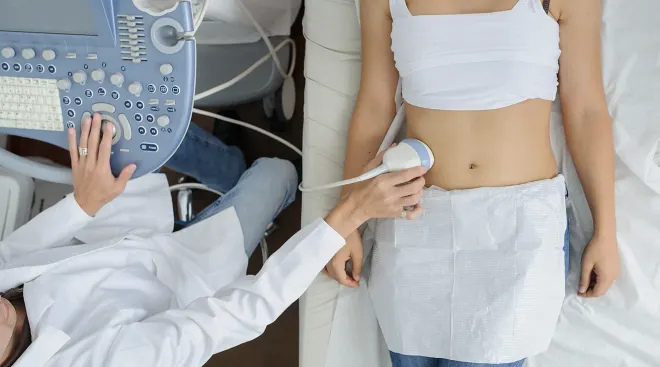
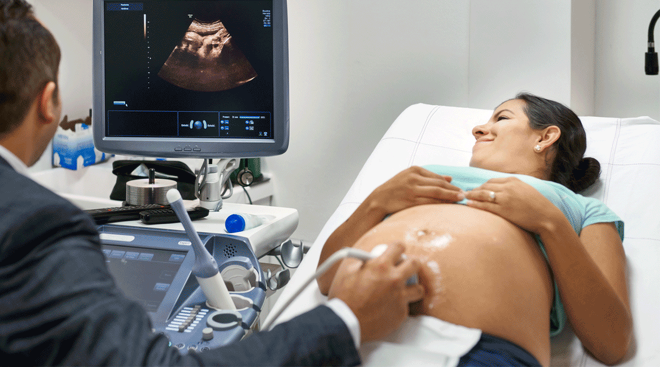
Your first ultrasound
This is your chance to see your little bean! At the same time, your doctor will take some measurements to make sure baby is growing nicely. The length between crown and rump is typically noted to get an idea of gestational age—which is crucial for figuring out when to time your prenatal screenings in the coming months. Your provider will also measure the gestational sac and make sure it’s an intrauterine pregnancy [as opposed to an ectopic one, which isn’t viable].
Urine test
Your urine will be tested at every visit during your pregnancy because it gives a good indication of your health. Urine can be tested for infections or diseases of the mother’s urinary tract, and high levels of glucose could be a sign of diabetes. Doctors also like to measure the amount of protein in urine early in the pregnancy so it can be compared to levels later on. High levels may be a sign of preeclampsia, a pregnancy-induced hypertension, which can be dangerous for both mom and baby.
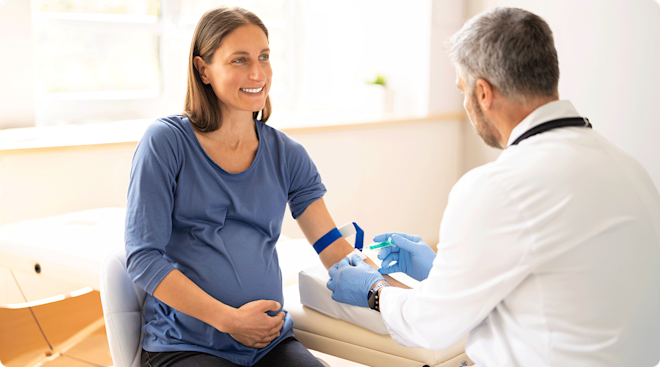
Diagnostic blood tests
The doctor will draw your blood and send it to a lab to get a read on both the characteristics of the blood itself, as well as to find out whether you have any medical conditions that could affect the general health of baby and the pregnancy. This type of prenatal testing looks for:
• A complete blood count (CBC), which tallies up the numbers of all the different types of cells in your blood. A red blood cell count will flag doctors if you have anemia, a white blood cell count reflects the health of your immune system, and a platelet count indicates any trouble with clotting.
• Blood type, which refers to your Rh factor. Most people are Rh positive. If you’re Rh negative and baby is Rh positive, you may be given an injection later in your pregnancy to prevent you from making antibodies against the Rh antigen in baby’s blood.
• Rubella (aka German measles), which can cause birth defects.
• Hepatitis B and hepatitis C, which are viruses that infect the liver and can be passed on to baby.
• Sexually transmitted infections (STI), including syphilis, gonorrhea and chlamydia, which need to be treated if found or else they could cause pregnancy complications.
• Human immunodeficiency virus (HIV), which is a disease of the immune system and causes AIDS. If you’re HIV-positive, medications will be given to prevent you from passing the virus to baby.
• Tuberculosis, which can cause pregnancy complications. If you’re in close contact with someone who has it or if you’re HIV-positive, your doctor will test for it.
Pap smear
If you’ve had one in the last year, you can skip this one. If not (or if you’re not sure), it’s included in the first-trimester prenatal screening. This way, your doctor can make sure there aren’t any abnormal cell changes of the cervix or signs of cancer, says Huss.
First trimester prenatal genetic testing
These prenatal screening tests assess a woman’s risk for delivering a baby with chromosomal disorders, such as Down syndrome. They’re performed sometime between weeks 10 to 13 and are offered to all women, but, as with all genetic tests, it’s your choice to take them or not. Your doctor will discuss your options at your first visit, take note of your preferences and plot out your schedule of prenatal genetic testings—including screens and if appropriate, diagnostic tests—for the rest of your pregnancy. The first trimester screens include:
• Maternal serum (blood) tests, which measure the level of a protein (PAPP-A) as well as the level of a hormone (hCG), both produced by the placenta.
• Ultrasound test for fetal nuchal translucency (NT) looks at the thickness of the gap that occurs in back of the fetus’s neck.
The measurements from these prenatal tests will be analyzed with your age and any other relevant conditions, and you’ll receive a result that expresses baby’s risk for having a certain condition.
Prenatal cell-free DNA screening
The cell-free fetal DNA test (aka noninvasive prenatal testing, or NIPT) is, as you’d expect, a genetic test. It’s best done after 9 weeks, and while it’s available for all women, it’s most appropriate for those with a high risk for delivering a baby with Down syndrome, trisomy 13, trisomy 18 and other conditions related to a chromosome abnormality. Risk may be determined based on the mother’s age or on abnormal results from the earlier first-trimester prenatal genetic testing. The “cell-free DNA” refers to the tiny bit of placental DNA that ends up in mom’s bloodstream; results take about a week. It has a 99 percent accurate-detection rate for Down syndrome and a low rate of false positives, but it’s still a screening, not a diagnostic test, and only determines likelihood. So if you want a definitive answer, you’ll need CVS or an amniocentesis (see below).
Chorionic villus sampling (aka CVS)
This is your first chance to opt for a prenatal genetic diagnostic test. Essentially, “CVS is a biopsy of the placenta,” Norton says. Because it’s an invasive process—involving inserting a needle through the maternal abdomen or a catheter through the cervix in order to sample cells from the placenta—with a small risk for miscarriage and other complications, it’s typically performed only in women who are considered high-risk based on earlier noninvasive screens. The cells are then analyzed by a lab to confirm the number of chromosomes. CVS also works as prenatal testing for cystic fibrosis and Tay-Sachs. As an alternative to an amnio (see below), it has the advantage of being done at 10 to 15 weeks, as opposed to only after 15 weeks. Results come back in about seven to 10 days.
Next up on your prenatal testing schedule? More opportunities to glean how baby is coming along.
Quad test
The quad (quadruple) test, also known as a multiple marker screen, is the first part of the second trimester set of prenatal genetic testing. (The second part is the mid-pregnancy ultrasound; see below.) The quad test measures levels of:
- alpha-fetoprotein (AFP), a protein baby makes
- hCG (same as in the first-semester screen)
- estriol, a hormone from the placenta and baby’s liver
- inhibin A, another placental hormone
Because this prenatal screening test detects four instead of three markers, it has essentially replaced the triple screen. Patients who didn’t undergo a first trimester genetic screening have the option of taking it, ideally, between 15 and 18 weeks. The results from the first trimester prenatal genetic blood test can also be combined with the quad test to provide more accurate results. Abnormal levels of these substances affect baby’s risks of a chromosomal disorder; if this is the case, you may want to discuss your results with a genetic counselor and consider an amniocentesis for a more definitive assessment.
Amniocentesis
Amniocentesis is a diagnostic test that’s typically performed between 15 and 24 weeks and is 99 percent accurate in determining chromosomal abnormalities. This type of prenatal testing is offered to women at high risk (because of age or earlier genetic screening results) who want to know for sure whether baby has a genetic disease. Like CVS, it’s an invasive procedure and carries with it a small chance of miscarriage. During the procedure, a needle is inserted through your abdomen and into the amniotic cavity to collect a small amount of the fluid. That fluid is then sent to the genetic lab, where cells are grown and the chromosomes are analyzed. The results, which return in about 10 days, can then be discussed with your doctor and a genetic counselor.
Glucose challenge screening test
At 24 to 28 weeks, you’ll be screened for gestational diabetes. (If you had the condition in an earlier pregnancy, you can take the test in the first trimester.) Your doctor will have you drink a glucose liquid and then draw your blood an hour later. If high levels of sugar are detected in the blood, it’s an indication that your body isn’t processing sugar effectively and you may need a glucose tolerance test to confirm whether or not you have gestational diabetes. This is important to know because high levels of sugar can cross over to baby and cause him to become too big. This, in turn, can lead to pregnancy complications (such as preeclampsia) as well as lifelong health problems.
Glucose tolerance test
This test is offered to women with a high risk of gestational diabetes. It’s similar to the earlier screening, except you’re asked to eat a certain amount of carbohydrates days before and fast for eight to 14 hours before gulping down that sugar liquid. Blood will be drawn several times: the first time to provide a base-level reading of sugar levels, and then over the course of the next few hours to get a read on how your body processes sugar over time. If you test positive for gestational diabetes, your doctor will provide lifestyle adjustments, such as a high-protein diet and exercise regimen.
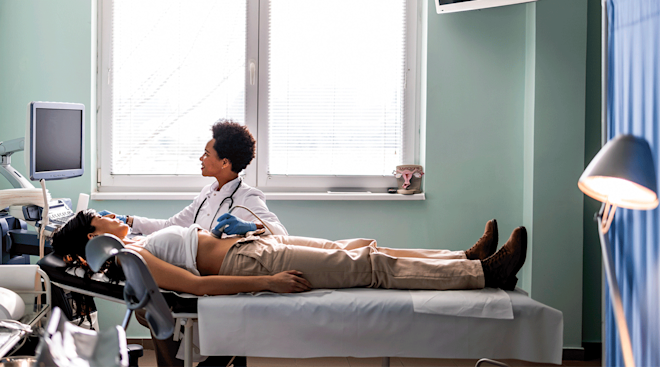
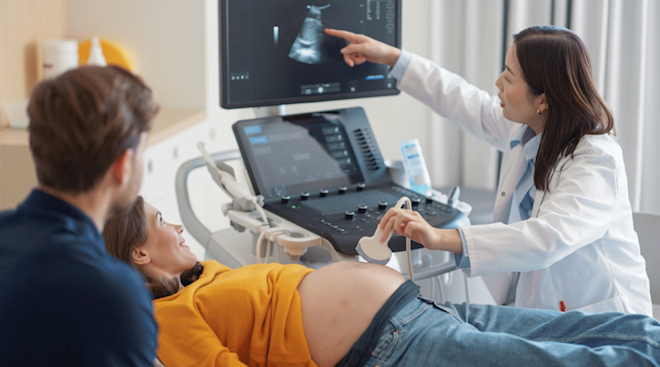
Mid-pregnancy ultrasound
Also known as the anatomy scan or 20-week ultrasound, this exam is standard procedure and part two of your second-trimester prenatal genetic testing. Performed between 18 to 20 weeks, it checks for baby’s internal measurements and confirms that baby’s growth is on target for the due date. If you didn’t find out baby’s sex from the first trimester genetic tests, this is your opportunity to see baby’s anatomy and learn whether you’re having a boy or girl. The ultrasound is also used to examine the amniotic fluid and the location of the placenta. Finally, the doctor can assess the risk that the pregnancy may be affected by trisomy 13, 18 or 21; depending on the results, you may want to follow up with an amniocentesis for an actual diagnosis.
You’re in the home stretch! By now, you should have a good idea as to how baby is doing, but your provider has just a few more tests up her sleeve, just to make sure baby arrives in the best of conditions.
Group B strep test
This test, done at approximately 36 to 37 weeks, screens for the presence of group B streptococcus, a type of bacteria present in about 25 percent of women. It’s done by inserting a swab into the vagina and then into the rectum. “The only time it needs to be treated or detected is during pregnancy,” Wright-Bennion says. “Some women are normally colonizers of the strain. We treat it during labor with an antibiotic so that babies don’t pick up that strain of bacteria during childbirth.” That bacteria is very aggressive in newborns and can lead to a serious infection that can even result in death.
Nonstress test
This special prenatal testing is done in high-risk pregnancies that could end up with complications or a stillbirth. It’s also done if you sense decreased movement of the fetus or if your pregnancy goes past 40 weeks. A nonstress test measures baby’s heart rate in response of fetal movement over a period of time. (The “nonstress” refers to the fact that this test doesn’t place any stress on baby.) You might have it done in the doctor’s office or she may refer you to the hospital. It takes at least 20 minutes, and you’re asked to lie down with a sensor strapped around your belly to measure baby’s heart rate. If two or more heart-rate “accelerations” happen within a 20-minute period, the result is considered reactive or “reassuring.” (That’s a good thing!) If not, the test may go on for 20 more minutes (baby may have been sleeping). If the heart rate does not accelerate, baby may not be getting enough oxygen and your doctor will determine next steps (which may include delivering baby early or right away).
Biophysical profile
This weekly or semi-weekly prenatal test is typically performed after 32 weeks. As with the nonstress test, it’s performed on women at risk for pregnancy complications and entails both monitoring of the fetal heart rate as well as an ultrasound. Various aspects are scored, including fetal heart rate, breathing movements, body movements, muscle tone and the amount of amniotic fluid. Depending on the score and your situation, the doctor may also decide to deliver baby early or right away.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
BreAnne N. Huss, CNM, is a certified nurse midwife and women’s health nurse practitioner at Kootenai Health in Coeur d’Alene, Idaho. She obtained her Bachelor’s degree in Nursing from Grand Canyon University in Arizona and completed her certified nurse midwife and nurse practitioner training at Georgetown University.
Julie A. Romero, MD, is a maternal-fetal medicine specialist based in California. She earned her medical degree from and completed her ob-gyn residency with Mount Sinai.
Jennifer Wright-Bennion, CNM, is a certified midwife and advanced practice registered nurse at Banner Medical Group in Queen Creek, Arizona. She earned her master’s degree as a nurse practitioner from the University of Utah and has worked in the field for over 20 years.
Learn how we ensure the accuracy of our content through our editorial and medical review process.
Target Baby Registry
Free $100+ Value Welcome KitFree $100+ Value Welcome Kit
15% Completion Discount15% Completion Discount
Free 1-Year ReturnsFree 1-Year Returns
20+ Exclusive 20% Off
Deals For Mom & Baby20+ Exclusive 20% Off Deals For Mom & Baby1:1 Concierge With
Baby Gear Specialists1:1 Concierge With Baby Gear Specialists

*Subject to availability and Retailer's terms.
We earn commissions from these links.