I Got a Positive Pregnancy Test—Now What?
Some of us dream for months (and sometimes years) of that telltale plus sign. For others, pregnancy is a complete surprise. Either way, you’re definitely not alone if you find yourself wondering, “I got a positive pregnancy test—now what?”
Finding out you’re pregnant is a life-changing moment that comes with its fair share of surging emotions: excitement, joy, relief, panic and maybe an extra dose of confusion over what to do next. But before you start deciding between an epidural or a medication-free birth, pause for a second. You’ve got 40 weeks to find all the answers, so take it one trimester at a time.
The best way to make sense of a positive pregnancy test is with, well, baby steps. “You don’t have to figure it all out the second you’re pregnant,” says Rebekah Wheeler, CNM, MPH, a midwife based in Sonoma County, California. “Pregnancy is a process, and asking yourself if you’ll be a good mother, learning to trust your instincts, is all part of it.” So what are the important steps to take—and when?
Focusing on all the big and small to-dos on your ever-growing list (not to mention the changes happening in your ever-growing body) can be daunting, to say the least. Fortunately, we’re here to help you streamline and simplify. We’ve created a comprehensive guide to break down exactly what to do after a positive pregnancy test, from scheduling your first prenatal visit to making healthy changes to your current lifestyle. Follow along so you can feel informed and prepared in the early stages of pregnancy.
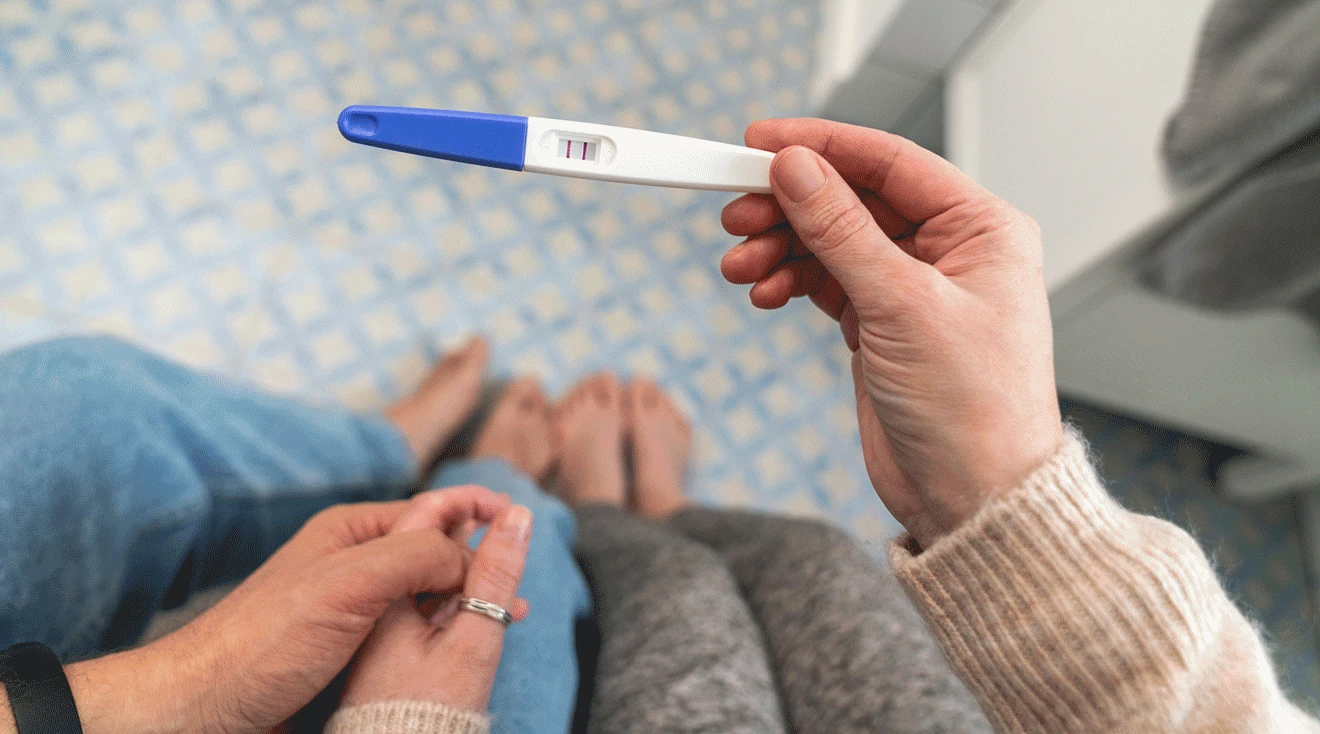
If your first instinct is to run to the pharmacy and buy all the different pregnancy test options, take a deep breath and slow down. Certainly, there’s no harm in taking a second test. Human error and misreadings can occur—so a little validation can give you some peace of mind.
It’s true that an expired pregnancy test or, more commonly, user error can result in a false positive. This is why it’s important to read labels and carefully follow all included instructions when taking a pregnancy test. Wait too long to check the result, and you may note the appearance of a faint evaporation line and misread the results—meaning you interpret it as positive when it’s actually negative.
Keep in mind that while false positives are very uncommon with pregnancy tests, there’s a small chance that an at-home test can pick up the pregnancy hormone hCG, even if you’ve miscarried shortly after conception—something that doctors refer to as a chemical pregnancy. “You probably wouldn’t even know that you were pregnant, if you didn’t take the pregnancy test,” says Mary Jane Minkin, MD, a clinical professor of obstetrics, gynecology and reproductive sciences at Yale School of Medicine in New Haven, Connecticut. If you did have a chemical pregnancy, you’ll likely get your period a little late.
According to the Mayo Clinic, a positive pregnancy test could also happen if you’re taking certain medications, including fertility drugs, and in the event of an ectopic pregnancy. For this reason (and others), it’s important to schedule a doctor’s appointment after getting a positive pregnancy test result.
With so much to think about, it’s hard to know what to do when you find out you’re pregnant. But one thing you’ll likely be itching to know is baby’s due date. Conception typically happens between 11 and 21 days after the first day of your last period, but since it’s tricky to know when conception actually occurs, doctors instead base it on the first day of your last period. Check out The Bump due date calculator to get an estimated date. This will also help you gauge how far you are in your pregnancy. Farther along than you expected? Remember, your progress is tallied from the first day of your last period, so the two or three weeks before you ovulated are still counted, even though you technically weren’t pregnant yet.
You’ve received a positive pregnancy test—now, what you can and should do is take a beat to let the monumental news sink in. Even if you’ve been looking forward to this day, it’s not uncommon to feel a bit overwhelmed. Give yourself time and grace—and then celebrate!
Bask in this joyful moment, perhaps together with your partner, before well-meaning grandparents and friends accost you with a million questions: “Are you going to find out the sex? Do you want a boy or a girl? Have you picked out a name?” Finding out you’re pregnant is the first sign your life is about to change in a million ways. Add a surge of pregnancy hormones to the mix and you’ve got yourself a kaleidoscope of emotions. “You’re basically flooded with progesterone, which causes you to feel much more vulnerable,” Wheeler says. This means you might be prone to crying and panicking about the future and your career—and that’s completely normal. “Most of the time these moods will pass if you rest. Don’t take on unnecessary tasks that you can avoid,” adds Minkin.
After you see that positive home pregnancy test, you’ll want to confirm it with a professional. And even if you may not see the doctor right away, calling to schedule an appointment is one of the first steps to take after finding out you’re pregnant—depending on the practice, wait times can be long.
When to visit doctor after positive pregnancy test
Your first prenatal visit usually happens around your eighth week of pregnancy. If you have an existing medical condition, had previous miscarriages or are experiencing abnormal pain or other atypical symptoms, your doctor may want to see you sooner. In the meantime, don’t hesitate to reach out to them with any and all questions or concerns.
How to decide on the type of care provider
As you prepare to make your first prenatal appointment, you can decide to seek prenatal care from either an ob-gyn or a midwife. The decision between the two depends on what you’re hoping for during pregnancy and delivery. If you’re interested in a vaginal delivery with an epidural or a planned C-section, or if you think you may have a higher-risk pregnancy (perhaps because of diabetes or high blood pressure), then an ob-gyn is likely the best choice since they’re equipped to offer medication and perform surgery. On the other hand, those hoping for a low-intervention vaginal delivery (maybe even at home) can look for a midwife. Oftentimes, nurse midwives can request the same labs and ultrasounds as an ob-gyn. But guess what: You don’t necessarily have to pick one or the other. A lot of hospital practices work with midwives who spearhead prenatal care and labor with an ob-gyn backing them up.
How to find the right doctor for you
Once you decide on the type of care for you, start scouting for an awesome provider. If you already have a great ob-gyn and want to stick with them, great! If not, there are many ways to find one you’ll feel comfortable with. “Yelp.com is actually a pretty good way to find an OB or midwife,” says Wheeler, who suggests cross-referencing well-rated providers with those recommended in prenatal yoga classes and childbirth centers. Zocdoc.com, Healthgrades.com and RateMDs.com are some other sites you can explore to find provider ratings.
If you already know which hospital suits you best, try Minkin’s trick to find an ob-gyn: Call the head nurse at labor and delivery and ask for a recommendation—the nurses see doctors during the most stressful times and know who takes good care of their patients. And don’t worry if you don’t love the first doctor you meet with; it’s more than okay to try out different midwives and ob-gyns before you commit. “You can transfer up until the moment you’re in labor,” says Wheeler. (Of course, be sure to ask your insurance if they’ll cover it.) “People feel embarrassed leaving, but you never have to tell the provider and have a confrontation. The new office will request all your medical records.” The important thing is that you find someone trustworthy who makes you feel comfortable.
After your first visit, and if everything is progressing smoothly, you’ll see your doctor once a month for the first two trimesters. After 32 weeks, the visits are twice a month, then once a week after 36 weeks.
You might be tempted to shout “Just found out I’m pregnant!” from the rooftops. And, sure, snapping a picture of your positive pregnancy test and sharing it on social media will do the job, but announcing that you’re expecting a baby is a bit different than Instagramming your lunch. Many couples wait until after 13 or 14 weeks to make the news public, since that’s when the risk of miscarriage goes down significantly. When it comes to close family and friends, you may decide it makes sense to spill the beans around six to eight weeks. As one expectant mom put it, “even if we did lose the baby, I would need my parents and close friends for support, so I’d be telling them either way.” Plus, you might want to loop in close family and friends not only so they can celebrate, but so they can also be understanding if you bewilderingly break down in a waterworks of emotions.
Friends and loved ones can help you find your footing in this exciting new role of a lifetime. It takes a village, and creating that community can start now if you choose. At the end of the day, it’s completely up to you and your partner when and how you want to share the happy news.
The one group of people who can wait for your announcement is employers and coworkers. “It’s no one’s business in the first trimester,” says Christine Romans, senior business correspondent for NBC News and the author of Smart is the New Rich: Money Guide for Millennials. “Later, say at 20 weeks when you’re going to start showing, let your boss and human resources know. Together, you’ll want to start plotting through how long you will take off for maternity leave and how to delegate your work in your absence.”
Among the things to know when expecting baby? Understanding what’s in store for you for the next nine+ months. One of the coolest things after finding out you’re pregnant is tracking baby’s growth—from the size of an apple seed to a watermelon!—and the many changes in your own body via The Bump Pregnancy Week-By-Week guide (and if you haven’t already, download The Bump app.)
While everyone’s body reacts differently, you’re bound to have at least some of the standard early pregnancy symptoms: nausea, cramping and spotting, sore breasts, acne, mood swings, frequent urination, headaches and food cravings and/or aversions, to name a few. You’ll also likely experience a level of exhaustion that rivals all the all-nighters you may have pulled. This please-let-me-lie-down kind of tiredness, courtesy of an uptick in progesterone, peaks between 8 to 12 weeks and then starts to ease up.
If these physical changes come as a surprise—or if this is baby number one—you may find yourself facing a steep learning curve. Of course, instinct may kick into gear and some things will come naturally. Other parts of pregnancy and early parenting will require a bit more time, patience and practice. The good news is that there are plenty of resources available to help you navigate this new stage of life, from books to podcasts and apps. You can also sign up for expert-led classes to gain a deeper understanding of labor and delivery issues, breastfeeding and newborn care; these sessions are often hosted at local hospitals or community centers. Our advice? Do your due diligence, and slowly start your research as soon as you receive that positive pregnancy test—there’s a lot to cover.
You probably already know that smoking and drinking alcohol are no-nos during pregnancy, but there are a bunch of other ways you’ll need to get your body into tip-top shape for a healthy pregnancy. If you’re not already taking prenatal vitamins, now is the time to start—as baby develops, they’re going to need calcium to build bones and iron to make red blood cells, plus folic acid to prevent neural tube defects and loads of other important nutrients. And baby gets all this from what you’ve got stored in your body. “The kid’s going to steal from you,” Minkin says. “You want to make sure your body doesn’t get depleted.”
In terms of changing up your daily menu, a pregnancy diet isn’t all that different from a typical healthy diet—think: lots of fruits, veggies, whole grains and lean proteins. But there are a few foods that should be avoided: Steer clear of cold cuts, deli salads, unpasteurized cheeses and refrigerated smoked seafood, since these can house listeria, a bacteria that can cause pregnancy complications. You’ll also want to avoid raw fish (sushi) and those that are high in mercury (swordfish, tilefish and king mackerel), since the heavy metal is toxic to baby’s nervous system. You should also limit your caffeine intake to no more than 200 mg a day.
While nut butters, salmon and green veggies are great kitchen staples for the next 40 weeks, if you’re battling with morning sickness, you may be living on a diet of applesauce and crackers at first. “Go easy on yourself,” Wheeler says. “Forget the nutrition component until you feel better.” She also recommends high-protein foods, like chicken and eggs, before bed to keep you satiated longer and minimize nausea in the morning.
After finding out you’re pregnant, you’ll also want to drink plenty of liquids. Staying hydrated allows your body to produce more blood volume, build new tissue, carry nutrients through your body and flush out your (and baby’s) waste. Tired of chugging plain water? Sparkling water, fruit-infused H20 and even watermelon smoothies (just blend watermelon with a bit of frozen berries) are excellent alternatives to not-so-appetizing flat water.
You may feel pressure to act happy and grateful during pregnancy, and not express doubt or worry. Rest assured that any feelings you have about being pregnant or having a baby are perfectly valid—and, yes, that means it’s normal if you’re more “uh oh, what now?” than “yippee!” about your positive pregnancy test.
If persistent worries creep up or if you lose interest in daily activities, be sure to see a mental health professional. It’s important to tackle your mental health concerns during pregnancy in order to help prevent or lessen issues like postpartum anxiety and postpartum depression. Research shows that treating depression during pregnancy can help prevent preterm birth and other health complications, as well as lead to better bonding and breastfeeding outcomes.
In addition to healthy pregnancy snacks, you’ll want to continue exercising. According to the Centers for Disease Control and Prevention (CDC), you should aim to gain between 25 and 35 pounds during your pregnancy if you’re of normal BMI. If you’re underweight or overweight, the recommended weight gain should fluctuate by about five to 10 pounds, respectively.
Exercising throughout your pregnancy not only helps you manage a healthy pregnancy weight gain—it also prepares your body for the strain of carrying and delivering a baby and builds the stamina you’ll need after childbirth, when you’re constantly lifting and cradling your (often not-so-light) newborn.
So what workouts are pregnancy-friendly? There are plenty of ways to stay fit safely—from prenatal yoga classes to walking, swimming and more. Anja Pierre, a personal trainer in New York City, recommends focusing on exercises like planks and squats that utilize the core and the pelvic floor. Try moves that engage the glutes and shoulders and work on the proper alignment of the spine, which in turn preps you for carrying your growing frontal load. “You’ll rely on total-body strength to perform tasks you never thought twice about, like opening a door, getting out of a cab or getting out of bed,” Pierre says. “Start working those arms if you haven’t already!”
You’ll want to avoid contact sports and activities where you’re more likely to fall, like skiing and horseback riding, and steer away from exercises in a poorly ventilated space, like hot yoga and even spinning. “The fetus is vulnerable, so you don’t want to be in a situation where you can quickly overheat,” Pierre says. “Stay hydrated and maintain your body temperature at a normal level.” She also nixes crunches, since “they’re really not as effective as people think, and they can lead to abdominal separation.” Above all else, listen to your body; if any type of exercise or movement causes pain, stop immediately.
Once you see those parallel lines on your positive pregnancy test, it’s time to take a closer look at your bottom line. “Congratulations! You’re going to have a baby! Now start saving for college,” Romans says. “I’m not kidding even a little bit. You have just 18 years to squirrel away the money for a college education (and they go by quickly!).” Sure, thinking about a 529 plan instead of muslin blankets isn’t super-exciting, but it’s the responsible thing to do—and it doesn’t mean you can’t also enjoy indulging your nesting instinct with cute crib sheets, tiny onesies and other registry goodies.
Of course, it’s not just college you’ll have to start saving for: The first few years of baby’s life can be shockingly expensive. Want to guess how much? According to a 2019 survey, most people thought baby’s first year typically costs around $9,400. Sorry, but not even close—that survey found it’s more like $13,200, and others say it can be even more. But don’t freak out: There are plenty of ways to shop smart and save like a savvy parent-to-be.
What else is on the list of what to do after a positive pregnancy test? Head to the benefits department. Once you’ve shared the news with your employer, learn about maternity leave and insurance perks. “Depending on your policies, there could be lactation consultant home visits, a free nutritionist, prenatal vitamins, even a free breast milk pump,” Romans says. At a minimum, the Family and Medical Leave Act allows you to take up to 12 weeks of unpaid leave (as long as you’ve been with the company for at least a year and your employer meets certain federal requirements). Make sure to ask when and how to add baby to your health insurance, since a newborn is only eligible for enrollment within the first 30 days after birth and won’t be subject to any preexisting conditions, even if they have one.
Frequently Asked Questions
When’s the best time to tell people you’re pregnant?
There’s no one-size-fits-all answer to when to announce your pregnancy. It depends on your personal preferences, and factors such as your family and work situation. Some people choose to share the news when they first hear baby’s heartbeat, typically around week 7 or 8. Some may wait until the first trimester is over, as that’s when miscarriage risk substantially decreases. Others opt to have genetic testing done first or wait until after the 20-week ultrasound, a big milestone when your technician will perform a full anatomy scan. Ultimately, it’s completely up to you who to tell and when to tell them! Check out some unique ways to tell your partner you’re pregnant here.
I’m a first-time parent. What’s the best way to learn how to take care of baby?
Taking care of a freshly minted human being may seem like a daunting task at first. There are many places to learn how to take care of baby, from parenting books to Instagram accounts to friends and family. To keep from getting overwhelmed, start with the basics for your newborn baby: feeding (hint: on demand’s usually best), sleep (around 20 hours a day, and it’s normal for them to have their days and nights confused), diapers (they should be filling five to eight a day), and plenty of cuddles.
What prenatal appointments do I need to attend?
You’ll likely have prenatal appointments once a month or so between your first prenatal visit and 28 weeks of pregnancy. Between 28 and 36 weeks, you’ll likely see your doctor twice a month. At 36 weeks, as you get closer to delivery, you’ll start weekly appointments. If you’re over 35, your provider may suggest extra appointments and prenatal testing. See a detailed breakdown of the typical prenatal OB appointment schedule here.
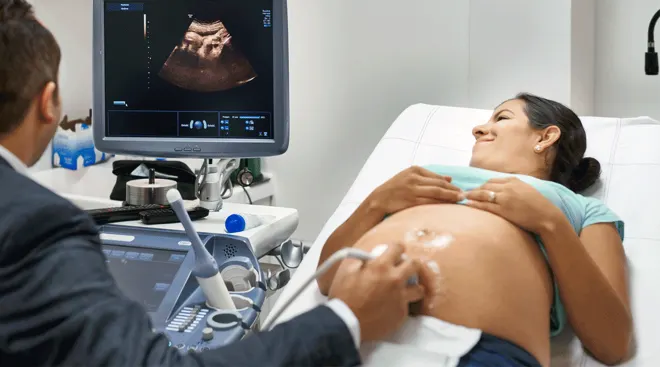
When do you get your first ultrasound?
Your first ultrasound will typically be between 6 and 10 weeks. This test will establish your estimated due date and confirm fetal viability.
How can I figure out the best birth plan for me?
A birth plan is an important tool to communicate with your healthcare provider and nursing team during labor and delivery. You can start by checking out our birth plan template.
Now that you know what to do after a positive pregnancy test, you can feel a little less panicked and a lot more empowered. You have time, so be kind to yourself and take it milestone by milestone. Prioritize your health and happiness, and everything else will fall into place. You’ve got this.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Mary Jane Minkin, MD, is a clinical professor of obstetrics, gynecology and reproductive sciences at Yale School of Medicine in New Haven, Connecticut. She also received her medical degree there.
Anja Pierre is a personal trainer in New York City.
Christine Romans is a senior business correspondent for NBC News and the author of Smart is the New Rich: Money Guide for Millennials.
Rebekah Wheeler, RN, CNM, MPH, is a midwife, birth trauma specialist and trauma healing coach based in Sonoma County, California. She received a Master’s of Public Health and a Master’s of Science in nursing from Yale University in New Haven, Connecticut.
Centers for Disease Control and Prevention, Weight Gain During Pregnancy, June 2022
March of Dimes, Take Care of Your Mental Health During Pregnancy, July 2022
Mayo Clinic, Home Pregnancy Tests: Can You Trust the Results?, December 2022
University of Denver, New Research Shows Positive Impact of Prenatal Mental Healthcare on Babies, August 2024
Learn how we ensure the accuracy of our content through our editorial and medical review process.
Navigate forward to interact with the calendar and select a date. Press the question mark key to get the keyboard shortcuts for changing dates.