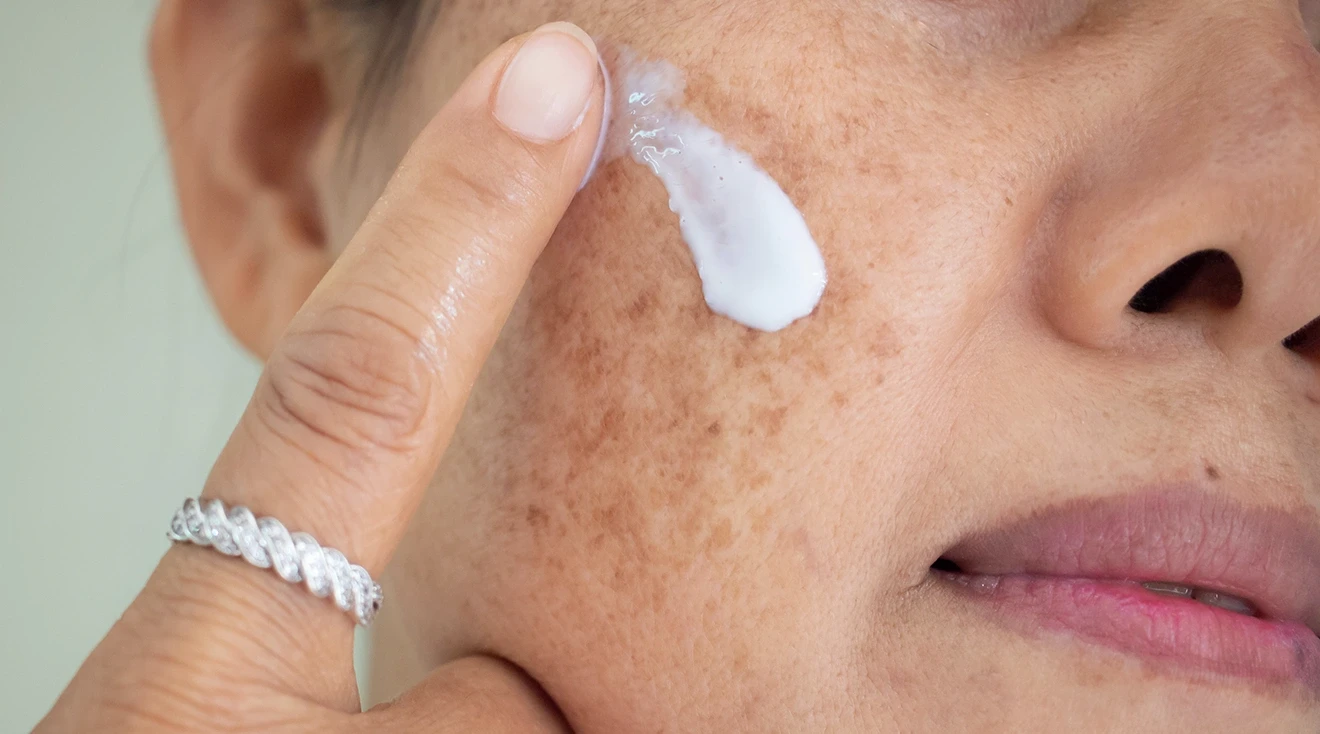
The Mask of Pregnancy: Everything You Need to Know About Melasma
You may have heard about the so-called pregnancy glow, but not everyone has perfect skin during this hormone-infused stage of life. Breakouts and sensitivities are normal and common. Some women even experience a condition called melasma in pregnancy.
While melasma isn’t harmful, it can cause aesthetic changes to your skin that you may find bothersome. It’s essentially a hyperpigmentation of the skin, and it often affects the complexion—which is why it’s been aptly nicknamed the mask of pregnancy. But what causes melasma during pregnancy and how can you lower the risk of developing it? Here, dermatologists and OBs break down the facts.
Melasma in pregnancy is also sometimes referred to as chloasma; it’s essentially a skin discoloration that tends to happen during pregnancy, says Ife J. Rodney, MD, founding director of Eternal Dermatology and Aesthetics and professor of dermatology at Howard University and George Washington University. “It usually causes brown, irregular [pigmentation] on the cheeks or around the eyes,” she adds. This is why some people refer to it as the mask of pregnancy.
Melasma is similar to the linea nigra, a brown line that can form on a pregnant person’s stomach. That said, while the linea nigra is caused by hormones during pregnancy, it’s less affected by sun exposure, explains Cindy Wassef, MD, assistant professor of dermatology at the Rutgers Robert Wood Johnson Medical School in New Jersey.
Melasma is common in pregnancy, says Jennifer Lew, MD, an ob-gyn at Northwestern Medicine Kishwaukee Hospital in Illinois. “Most pregnant patients have some increase in skin pigmentation,” she says. In fact, one study notes that melasma can happen in up to 70 percent of pregnant people.
Melasma is most often linked to hormonal changes associated with pregnancy, says Rodney. That said, it’s possible to get melasma because of sun or heat exposure, even when you’re not expecting.
Lew says that some people seem to be more at risk for developing melasma during pregnancy than others, including those with a family history of melasma and those who sit out in the sun without protection. “The darkening occurs with exposure to sun, so sunscreen and hats will lessen the amount,” Lew says.
Your skin tone may be a risk factor for melasma too. “Melasma is more commonly seen in those with darker skin types,” Wassef adds.
Melasma can appear at any point in pregnancy. “It could be early on, toward the end or in the postpartum period,” Rodney says. “Most often, it occurs during the second or third trimester, as hormone levels start to rise,” Wassef adds.
There are several treatment options for melasma, but not all are considered safe during pregnancy, says Joshua Zeichner, MD, director of cosmetic and clinical research in dermatology at Mount Sinai Hospital in New York City. During pregnancy, topical treatments containing vitamin C or azelaic acid “are helpful to lighten the patches,” he says. Glycolic acid peels may also work to lighten melasma patches. But bleaching creams such as hydroquinone, salicylic acid peels, and lasers are reserved for after pregnancy, Wassef emphasizes.
Home remedies for melasma during pregnancy
Experts say melasma is tough to address on your own at home. “Melasma is difficult to treat, and it does tend to recur,” Rodney says. “It’s even more difficult to treat during pregnancy because we’re limited in terms of what treatments and procedures can be done.”
If you come across some home remedies to combat melasma in pregnancy, proceed with caution, and talk to your doctor before starting any DIY routine. Research has found some degree of success with the use of aloe vera and turmeric, but other ingredients may exacerbate skin issues. Suffice it to say, stick with the advice of a dermatologist or ob-gyn.
While there are some things you can do to lower your risk of developing melasma during pregnancy, they won’t definitively prevent it. “You may not be able to avoid it entirely,” Rodney says.
Of course, because sun exposure can worsen or trigger melasma, doctors stress the importance of sun protection. This includes taking the following steps to protect your skin:
- Wear sunscreen. “Sunscreen daily is a must,” Zeichner says. “One minute of unprotected sun exposure can undo one year of skin-brightening efforts.” Tinted mineral sunscreens are ideal because they also provide visible light protection, another factor known to worsen facial hyperpigmentation,” he adds.
- Stick to the shade. “Staying out of the sun can certainly decrease your risk,” Wassef says. If you’ll be outside for an extended period, try to find yourself a shady spot.
- Wear a hat. This can help shade your face—an area that’s especially prone to melasma. “Everyone will have sun exposure, so to avoid it entirely may not be possible,” Lew says.
Melasma can go away after pregnancy, but it’s not a guarantee. It may begin to fade a few months to a year postpartum, and reducing your sun exposure can certainly help expedite the process. That said, Wassef says that you may continue to experience some flare-ups.
If you’ve developed melasma in pregnancy, and it doesn’t fade fast enough for your liking after birth, Lew recommends consulting a dermatologist. They’ll likely recommend topical skin-lightening agents, along with more targeted treatments to help.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Jennifer Lew, MD, is an ob-gyn at Northwestern Medicine Kishwaukee Hospital in DeKalb, Illinois. She earned her medical degree from the University of Illinois at Chicago College of Medicine.
Ife J. Rodney, MD, is the founding director of Eternal Dermatology + Aesthetics and a professor of dermatology at Howard University and George Washington University. She earned her medical degree from Howard University.
Cindy Wassef, MD, is an assistant professor of dermatology at the Rutgers Robert Wood Johnson Medical School in New Jersey, where she also received her medical degree.
Joshua Zeichner, MD, is the director of cosmetic and clinical research in dermatology at Mount Sinai Hospital in New York City. He received his medical degree from the Johns Hopkins School of Medicine.
Collegium Antropologicum, Chloasma--the mask of pregnancy, October 2008
The Journal of Clinical and Aesthetic Dermatology, Are Natural Ingredients Effective in the Management of Hyperpigmentation? A Systematic Review, February 2018
Learn how we ensure the accuracy of our content through our editorial and medical review process.
Navigate forward to interact with the calendar and select a date. Press the question mark key to get the keyboard shortcuts for changing dates.