What Causes Stomach Pain in Pregnancy?
Stomach pain in pregnancy is one of those symptoms that can be hard to pinpoint. First of all, there are so many potential causes of it. Plus, sometimes it’s hard to tell whether the culprit is something innocent—like early-pregnancy bloating—or something more serious to check in with your doc about. Fortunately, more often than not, the cause is totally benign.
“I get aches and pains in my stomach all the time,” says The Bump community member Tigerlilym15. “It’s not a constant pain, but I get little pangs here and there pretty much every day. I think it’s just your uterus growing and stretching.”
So how can you differentiate between normal abdominal discomfort and something more serious? Read on to learn about the causes of abdominal pain while pregnant, symptoms to look for and what you can do to get relief.
- Stomach pain in pregnancy is very normal and can be caused by plenty of conditions, most of them benign. A growing uterus, round ligament pain and digestive issues can often contribute to abdominal pain during pregnancy.
- More serious causes of stomach pain in pregnancy include ectopic pregnancy, preeclampsia and preterm labor.
- If your stomach pain is severe, persistent and comes with vaginal bleeding or a fever above 100.4, you should see your healthcare provider.
When you feel any type of abdominal pain while pregnant, it’s natural to wonder whether it’s normal. Take comfort knowing that most women do experience some kind of abdominal discomfort during pregnancy, most commonly categorized as cramping and round ligament pain, says Rebekah Mustaleski, CPM, a midwife in Knoxville, Tennessee.
That said, it’s important to be able to differentiate between general discomfort and acute, severe pain, says Cynthia Flynn, MD, an ob-gyn in Daytona Beach, Florida. Listen to your body, and get checked out if “any pain is new, severe, persistent or deviates from your baseline threshold,” adds Alison Cowan, MD, an ob-gyn at Boulder Medical Center in Louisville, Colorado.
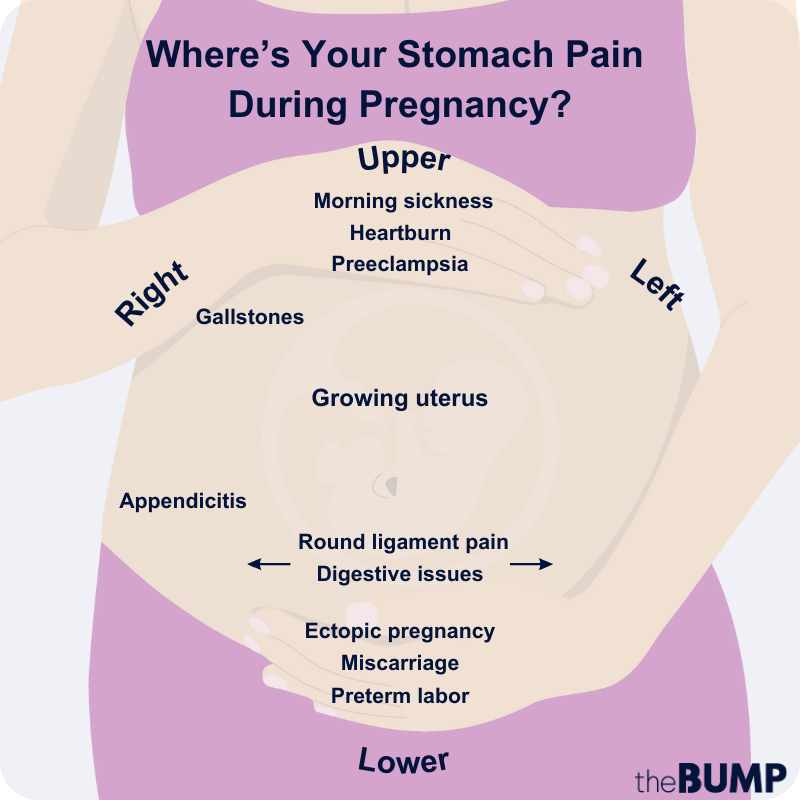
Where you feel stomach pain during pregnancy depends on the root cause. For example, you might feel round ligament pain “along the crease where your leg meets your torso,” explains Mustaleski, Below, a few common areas for experiencing abdominal pain:
Lower abdominal pain during pregnancy
Lower abdominal pain while pregnant is pretty common and can be related to a variety of causes, both benign and serious. Kecia Gaither, MD, MPH, associate professor of clinical obstetrics and gynecology at Weill Cornell Medicine and director of perinatal services at NYC Health + Hospitals/Lincoln, says it’s often caused by round ligament pain, which can feel like sharp, stabbing sensations as ligaments stretch to support your growing uterus. Increased blood flow and pressure in the pelvic area throughout pregnancy can also cause lower abdominal discomfort, she adds. Pregnancy constipation can lead to this type of pain too.
Meleen Chuang, MD, chief of Obstetrics and Gynecology at NYU Langone Hospital Brooklyn, adds that lower abdominal pain during pregnancy can also occasionally be a sign of ectopic pregnancy, miscarriage or, later on, preterm labor. Again, the reason is most likely benign—but always check in with your doctor if you’re concerned.
Upper abdominal pain during pregnancy
Chuang says that upper abdominal pain during pregnancy can be associated with morning sickness or a growing uterus. In more serious cases, it can occasionally be caused by gallstones or preeclampsia. Gaither adds that pregnancy heartburn “often occurs as the uterus presses on the abdomen,” which can cause upper abdominal pain.
Right side stomach pain in pregnancy
Cowan says right-side stomach pain while pregnant could be due to baby growing and repositioning (such as with round ligament pain), or it may potentially be a sign of something more serious, such as gallstones. Chuang says it can sometimes indicate appendicitis. (More about appendicitis in pregnancy later.)
Left side stomach pain in pregnancy
Cowan says that left-side stomach pain during pregnancy doesn’t usually point to a specific cause; it may be due to a number of factors, especially as the internal organs move to accommodate a growing uterus. “It can be associated with the body stretching and adjusting to the growing uterus or digestive issues like bloating,” says Chuang.
Ultimately, pain can manifest anywhere in the abdomen—or even a different area of the body entirely, Cowan says. This is another reason why it’s important to understand your baseline when it comes to discomfort, and let your doctor know if anything feels out of the ordinary.
With my last pregnancy, I had such bad gas and constipation at some points that it hurt to touch my belly or lay down. But if I could manage to pass it even just a little, then it eased the pain a fair bit.
Experiencing stomach pain while pregnant can be alarming, but there are plenty of harmless causes. (Of course, you’ll still want to flag these with your provider so they’re in the loop.) Some of the most common causes of stomach pain in pregnancy include:
- Baby’s growth: Your uterus and baby grow rapidly during pregnancy, which can cause abdominal pain in pregnant women, particularly in the right upper quadrant. In Cowan’s experience, most pregnant people are able to tell the difference between a serious complication and discomfort from baby’s positioning.
- Round ligament pain: Round ligaments connect the front of the uterus to the groin—and they stretch considerably during pregnancy, causing sharp pain in your abdomen, hips and groin, usually during the second trimester. This is one of the most common causes of abdominal pain in pregnancy, and it can be absolutely excruciating, sometimes made worse with prolonged sitting or standing. “Your uterus goes from being the size of a lemon to the size of a watermelon—that hurts,” says Meredith Alston, MD, a professor of obstetrics and gynecology at the University of Colorado School of Medicine and ob-gyn at Denver Health Medical Center.
- Constipation: Due to the way that progesterone slows down your GI tract, constipation can be made worse by pregnancy, says Alston. You’ll probably recognize the symptoms: stomach cramps, heaviness in your lower abdomen and having fewer than three bowel movements a week.
- Heartburn: Oftentimes, stomach pain in pregnancy may be due to GERD or gastroesophageal reflux disease. It’s also caused by your system slowing down and your growing uterus pushing on the stomach, especially in the third trimester. Your stomach might feel sour and you’ll have telltale pain as acid is pushed up into your esophagus. You’ll feel this pain in the midline, Cowan says, adding that, while common, it’s still important to mention this type of stomach pain in pregnancy to your provider, as it could be a symptom of a more serious issue, such as HELLP syndrome (more on this below).
- Gastroenteritis: Pregnancy doesn’t make you immune to stomach bugs. If you get one, you’re bound to feel some stomach pain while pregnant. “Your typical stomach bug in pregnancy usually feels pretty similar to one outside of pregnancy,” Cowan says. Most aren’t an issue as long as you’re able to take in liquids—but if your symptoms persist, it’s important to let your provider know. This is especially true if nausea, vomiting and/or diarrhea accompanies your stomach pain, as these could all lead to dehydration, and, consequently, “an increase in contractions or uterine irritability,” Cowan explains.
- Contractions: Braxton-Hicks contractions feel like a tightening and relaxing sensation in the abdomen rather than stomach pain during pregnancy. “A lot of patients describe it as feeling like their baby is balling up,” Cowan says; or, it may feel similar to menstrual cramps. “A contraction is not worrisome, especially if it’s not painful,” she adds. Of course, you may also experience contractions due to preterm or term labor; these will likely be more intense and accompanied by back pain. “The important distinction is whether those contractions lead to changes in the cervix or dilation of the cervix,” Cowan adds. “From a patient perspective, if you’re noticing an increase in the intensity and frequency of your normal contractions—whatever those may be—then it’s a good time to get checked out.”
My round ligament pains were very low in my tummy, a lot of tightening and some sharper and pinching pains. This is my second baby and I never felt that way with the first. I honestly thought I was having contractions. They did a quick ultrasound and the baby looked great. Round ligament pain can vary a lot from one pregnancy to another. If it comes down to it, my doctor said it's much better to call and go in for a quick checkup as opposed to worrying about it!
More serious conditions that show up with stomach pain in pregnancy are scary to learn and think about, but it’s important to know what to look for and to be prepared. Keep in mind that this worrisome pain may be “different from the normal cramping that one can experience during pregnancy,” Mustaleski explains. “If you have sharp, intense abdominal pain that makes you stop your activities or takes your breath away—or if it doesn’t improve with position changes, you’re bleeding with it or you’re also experiencing a severe headache or nausea, you need to contact your healthcare provider right away to be evaluated.” Some of the more serious causes of abdominal pain during pregnancy include:
- Ectopic pregnancy: Ectopic pregnancies are those that occur outside the uterus, usually in the fallopian tube. According to Alston, ectopic pregnancies are marked by pelvic pain and increasing abdominal pain with light or heavy vaginal bleeding. This is one reason why an early pregnancy ultrasound is so important, Cowan says, to ensure the pregnancy is intrauterine.
- Miscarriage: Abdominal cramping or pain in your lower abdomen during pregnancy with spotting and bleeding could signal a miscarriage, which typically occurs before the 20th week of pregnancy. If you have these symptoms or feel like something’s wrong, call your provider or go to the emergency room.
- Placental abruption: This occurs when the placenta pulls away from the side of the uterus. It can happen because of trauma—like falling down or a car accident—but it can also just spontaneously occur, Alston says. Placental abruption can prompt sudden back and abdominal pain in pregnancy, uterine tenderness and uterine contractions, notes the Mayo Clinic.
- Preterm labor: Sudden and intense abdominal pain during pregnancy could be the start of contractions. “You’ll get a waxing and waning pain—that’s what contractions do,” says Alston. “We worry when patients are having a feeling like their uterus is getting hard, coming and going, if they’re before 37 weeks.” You may also have bleeding or experience your water breaking.
- Preeclampsia: Preeclampsia is a disorder characterized by high blood pressure that typically occurs after the 20th week of pregnancy. It can cause upper right side pain during pregnancy due to resulting liver issues. However, both Alston and Cowan warn that sudden, severe indigestion that mimics reflux or stomach pain around the midline of the abdomen may also signal preeclampsia. According to the Mayo Clinic, other symptoms include severe headaches, changes in vision and shortness of breath.
- HELLP syndrome: The Cleveland Clinic notes that HELLP syndrome is a type of preeclampsia that most commonly occurs in the third trimester. It can cause upper right side pain during pregnancy due to liver inflammation, as well as heartburn-like symptoms.
- Chorioamnionitis: This an intrauterine infection that occurs when bacteria make its way from the vagina to the uterus and infects the membranes around the fetus, notes Carrie Terrell, MD, ob-gyn and division director for obstetrics, gynecology, midwifery and family planning at the University of Minnesota. Symptoms include fever, a tender-to-the-touch stomach and rapid heartbeat.
- Appendicitis: According to a 2022 review, appendicitis can occur in pregnancy. However, Cowan notes that appendicitis during pregnancy is less common than outside of it. Usually the abdominal pain is felt on the right lower quadrant, but, again, this may vary as the appendix can become displaced as the uterus grows. Symptoms include sudden lower abdominal pain on the right side or around your navel, loss of appetite, nausea and a low-grade fever.
- Gallstones: This occurs when digestive fluid hardens to create small stones in the gallbladder, notes the Mayo Clinic. They can cause sudden and sharp pain in the stomach while pregnant, particularly in the upper right quadrant of the abdomen or along the midline.
- Urinary tract infection (UTI): Symptoms include frequent urination (beyond the usual increase in pregnancy), pain with urination and cloudy or foul-smelling urine. “Most women will have at least one episode of a UTI in their lifetime, so it’s very likely that women who are pregnant have already experienced one and know what it feels like. It feels the same in pregnancy as it does outside of pregnancy,” Cowan says. When left untreated, UTIs can cause kidney infections, which occur more commonly in pregnancy than outside of it, she adds. While the most common symptom is a fever, you may also experience back pain. “Kidney infections are very treatable in pregnancy, but it’s crucial to get treatment, because if they’re untreated or not treated soon enough, they can progress to sepsis for moms, which is like a full-body infection and can also cause preterm labor,” she says.
- Ovarian torsion: Ovarian torsion occurs when an ovary twists over onto itself and cuts off its own blood supply, Cowan says. Ovarian torsions involve high-level abdominal pain—which may or may not be on the affected side—that can radiate to the groin or the back. The pain may even stop and start as the ovary torses and reverses repeatedly. According to a 2017 review, ovarian torsion is relatively uncommon during pregnancy, but occurs more frequently in people who have an ovarian cyst present.
There are some red-flag symptoms your provider should know about immediately, including if your abdominal pain is severe, persistent and comes with any vaginal bleeding or fever above 100.4, says Rhonia Gordon, MD, an ob-gyn at Mount Sinai in New York City. But for the most part, some abdominal discomfort and mild stomach pain is par for the course with all the musculoskeletal growing and stretching your body does during pregnancy.
For the more common causes of stomach pain in pregnancy, like heartburn and round ligament pain, there may not be much a visit to your doctor’s office will do to bring about relief. Still, experts say you should never hesitate to call your provider about any abdominal pain during pregnancy—it’s important information for them to have. “Generally, in all trimesters, we take abdominal pain pretty seriously,” says Terrell. “It can be a sign of something underlying or other ongoing issues, and we want to get people evaluated.”
The right relief for stomach and abdominal pain during pregnancy will depend on the cause. According to Alston and Mustaleski, for run-of-the-mill growing pains (usually occurring in the second or third trimester when your bump is bigger), you may find some relief from:
- Taking a warm bath or shower
- Taking an Epsom salt bath
- Applying a heating pad to your belly or sides
- Taking Tylenol (if it’s been cleared by your provider)
- Using abdominal compression or pregnancy support bands
- Staying active by walking or doing other light exercises, like yoga and gentle stretching
“Overall body movement will also help release muscle tension and prevent cramps and round ligament pains,” Mustaleski says. After all, “you’re carrying around this watermelon, and your back and abs tend to not like it all that much,” Alston adds.
Frequently Asked Questions
Is abdominal pain a sign of pregnancy?
Yes, sometimes abdominal pain can be a sign of pregnancy, says Chuang. It can happen very early on for some people: "Before I knew I was pregnant, I was having mild but perpetual aching in my abdominal area,” says Lauren Barth, associate director at The Bump and mom of three. “It felt similar to period cramps, but I kept not getting my period! It wasn't the first clue to tip me off, but eventually I put two and two together."
That said, abdominal pain alone doesn’t mean you’re pregnant—you should always take a pregnancy test to be sure.
What causes abdominal pain during pregnancy?
Everything from baby’s growth to constipation to preeclampsia can cause abdominal pain during pregnancy—if you’re unsure, your healthcare provider can help you pinpoint the cause based on its location, how far along you are and other factors. Gaither says that in general, hormonal changes and a growing uterus are major causes of abdominal pain during pregnancy. In the second trimester, says Chuang, round ligament pain can play a large role. “The growth of the uterus may cause stretching of ligaments supporting the uterus starting between 18 and 24 weeks,” she explains. “The pain typically occurs on one side of the belly and may radiate into the groin, feeling sharp, stabbing, dull or achy. It’s triggered by movements like coughing, sneezing, laughing or suddenly getting up.” In the third trimester, Braxton-Hicks contractions can cause abdominal discomfort.
What do the stomach pains feel like in early pregnancy?
“In early pregnancy, stomach pains can feel like stabbing pains, similar to menstrual cramps,” says Chuang. “Cramping as the uterus stretches feels achy and sore, often sharp and pulling with sudden movements.”
Can gas cause stomach pain in pregnancy?
Yes, gas can cause stomach pain during pregnancy, says Chuang. “Increased progesterone levels slow down the digestive tract, leading to gas and bloating,” she explains. “Constipation is another big issue in pregnancy, and this can also lead to stomach pain, which is more left-sided.”
Can stress cause stomach pain in pregnancy?
Chuang says that stress can exacerbate digestive issues like gas and ulcers. Adds Gaither, “Stress can contribute to stomach pain through muscle tension and its effect on the GI system. Anxiety and stress may lead to increased sensitivity to pain and may exacerbate conditions like IBS, which can worsen during pregnancy.”
Can a yeast infection cause abdominal pain during pregnancy?
While a yeast infection during pregnancy can cause vaginal discomfort and worsening vaginal discharge, it shouldn’t cause abdominal discomfort, says Chuang. If you’re concerned, it’s worth seeing your healthcare provider.
Abdominal pain in pregnancy can be exhausting and downright scary at times. Ensure your provider has a clear understanding of your pain level and what’s going on, and they’ll work with you to come up with a treatment plan. Hang in there—it’ll all be worth it once baby’s placed into your loving arms.
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Meredith Alston, MD, is a professor of obstetrics and gynecology at the University of Colorado School of Medicine and ob-gyn at Denver Health Medical Center. She earned her medical degree from Emory University School of Medicine.
Meleen Chuang, MD, is the chief of Obstetrics and Gynecology at NYU Langone Hospital Brooklyn and a clinical associate professor of obstetrics and gynecology at the NYU Grossman School of Medicine. She earned her medical degree from Stony Brook University School of Medicine in Stony Brook, New York.
Alison Cowan, MD, is an ob-gyn at Boulder Medical Center in Louisville, Colorado. She obtained her master’s and medical degree from Emory University and completed her residency at Northwestern University.
Cynthia Flynn, MD, is an ob-gyn in Daytona Beach, Florida, with over 20 years of experience. She received her medical degree from the Michigan State University College of Human Medicine.
Kecia Gaither, MD, MPH, MS, MBA, FACOG, is a double board-certified physician in ob-gyn and maternal-fetal medicine specialist and the director of perinatal services and maternal-fetal medicine at NYC Health + Hospitals/Lincoln. She also serves as an associate professor of clinical obstetrics and gynecology at Weill Cornell Medicine. She earned her medical degree from SUNY Health Science Center in Syracuse, New York, and holds a master’s degree in public health.
Rhonia Gordon, MD, is an ob-gyn at Mount Sinai in New York City. She earned her medical degree from Ohio State University College of Medicine.
Rebekah Mustaleski, CPM-TN, IBCLC, MPH, is a certified professional midwife and lactation consultant specializing in evidence-based maternity care. She co-founded Roots & Wings Midwifery in Knoxville, Tennessee. Mustaleski received her bachelor’s degree in psychology from Centre College, and worked as a doula and birth photographer prior to establishing Roots & Wings.
Carrie Terrell, MD, is an ob-gyn and the division director for obstetrics, gynecology, midwifery and family planning at the University of Minnesota. She earned her medical degree from University of Minnesota Medical School.
American Pregnancy Association, Round Ligament Pain During Pregnancy, 2023
American Pregnancy Association, Sharp Pain During Pregnancy, 2023
Cleveland Clinic, HELLP Syndrome, May 2021
CPE Emergency Medicine, Intermittent Ovarian Torsion in Pregnancy, May 2017
Mayo Clinic, Gallstones, August 2021
Mayo Clinic, Placental Abruption, February 2022.
Mayo Clinic, Preeclampsia, April 2022
STATPearls Publishing, Appendicitis in Pregnancy, August 2022
Real-parent perspectives:
- Lauren Barth, associate content director at The Bump and mom of three
- babybelugaco
- scbonnell04
- Tigerlilym15
Learn how we ensure the accuracy of our content through our editorial and medical review process
Navigate forward to interact with the calendar and select a date. Press the question mark key to get the keyboard shortcuts for changing dates.