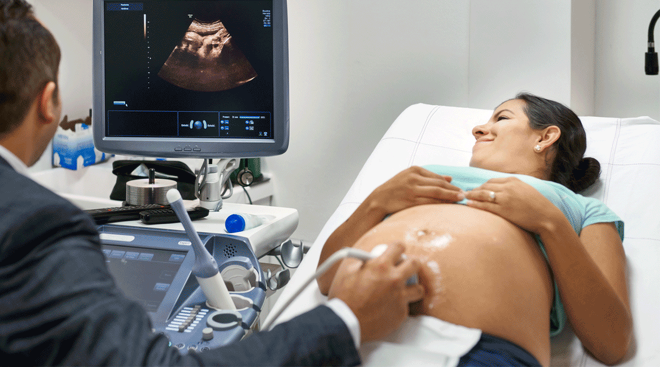
How to Prepare Your Health History for Your OB Visit
At your very first prenatal exam, your doctor may throw a million questions your way, about your health, your partner’s health and your family’s history of things like genetic disorders and diseases (or you may get a talk from a genetic counselor). And it’s pretty common find yourself going, “Uh… I don’t know… maybe?” But this is serious stuff. Knowing about a genetic problem or pregnancy health condition that runs in your family can alert you and your doctor that you might need to be monitored extra closely, or it might make you decide to get special genetic testing to ensure baby’s doing okay. So it’s a good idea to get prepared. Here’s how.
The number one thing your doctor will likely ask is your health history and age, since the chance of certain genetic issues (like Down syndrome) increases with maternal age. The second? Your family’s health history. “I ask about the patient’s mother’s pregnancies, if she had problems or if she had any babies with congenital malformations,” says Laura Riley, MD, ob-gyn and medical director of Labor and Delivery at Massachusetts General Hospital. “Then, I move on to the other sides of the families.” And while you may think you know your family well, you may not realize that your mom had preeclampsia, or your partner may have heard there was a baby with health problems in the family but may not have ever asked for the details. Now’s the time to ask. “Sometimes it’s really obvious stuff,” Riley says. “But there are some things that aren’t that obvious, like if there are males in your family with intellectual disabilities that are unexplained. It could be Fragile X (a genetic condition).”
“Most people give us their family’s medical history, like if a grandparent has a heart condition,” Riley says. “That’s important in general, but not as important as fetal issues and maternal issues.” So think about whether any babies in your family were born prematurely or had birth defects, or if anyone has had genetic conditions like cystic fibrosis, Tay-Sachs disease or sickle cell anemia. But don’t be scared that you might bring up the wrong thing. “It’s okay to mention everything you think of,” Riley says. “Sometimes talking about one thing will bring up another that’s really important.”
The doctor will likely ask about your ethnic background as well, since certain conditions run in specific cultural lineages.
As for medical history, prenatal conditions that run in your family—like preeclampsia, gestational diabetes, hypertension and preterm labor—are definitely important to bring up. But surprisingly, miscarriage is not. “Miscarriage is actually very common, and the vast majority are them are because of chromosomal problems that are a one-time thing, so I usually don’t make a big deal about that,” Riley says.
It’s okay to go to other prenatal appointments solo, but this is one your partner should definitely come along to. That’s because, while your family history is what affects your health, your partner’s family history can affect baby’s health. And even if you talk it over in advance, you might not be able to predict all the doctor’s questions prior to the visit.
Know this: If either you or your partner were adopted, or you used donor egg or sperm, you’ll have to accept that you may not have all the information other couples do in this case. That’s okay. Share what you know with the doctor and listen carefully to make the best informed decisions you can.
Discussing your and your partner’s health history with your doctor can help you figure out whether you should do genetic testing to evaluate baby’s risk of certain genetic problems. But if baby has a birth defect or genetic disorder, know that it can’t be “healed.” Some parents-to-be choose to test because they want peace of mind that baby is healthy. Others want to have advanced warning of certain issues so medical specialists can be there at birth. And others might want to end the pregnancy, depending on baby’s risk factor. “It’s worth talking with your partner about what you’re going to do with the information,” Riley says. “Would you want to do the genetic testing, and why do you want the results?” It’s not that you two have to know all the answers before the visit. Just have a general discussion about how you expect things to go. Your doctor or specialist can walk you through the decisions you’ll later make.
Armed with your health histories, your doctor can explain the different genetic tests available to you and your partner. And together, you’ll make a decision about what tests you might want to get.
If your doctor doesn’t take an extensive family history, or doesn’t do genetic counseling, you may want to find someone else to talk you through the process. Usually, your hospital has a staff that can do this. If not, check out the American Congress of Medical Genetics website, where you can search for a counselor near you.
Want a preview? Here are some genetic screening questions you can expect:
-
Will you be 35 years old or older on your due date?
-
Do any of these conditions run in your family or the baby’s father’s family?
Thalassemia (most common in Italian, Greek, Mediterranean and Asian backgrounds)
Neural tube defect
Congenital heart defect
Down syndrome
Tay-Sachs (most common in Ashkenazi Jewish, Cajun and French Canadian backgrounds)
Canavan disease (most common in Ashkenazi Jewish)
Familial dysautonomia (most common in Ashkenazi Jewish)
Sickle cell disease or trait (most common in African backgrounds)
Hemophilia or other blood disorders
Muscular dystrophy
Cystic fibrosis
Huntington’s chorea
Mental retardation/autism (if yes, was the person tested for Fragile X?) -
Are there other inherited genetic or chromosomal disorders in your family?
-
Do you have a maternal metabolic disorder (e.g., type 1 diabetes, PKU)
-
Have you or the baby’s father had a child with birth defects?
-
Have you had recurrent pregnancy loss or a stillbirth?
-
Have you taken any medications, supplements, vitamins, herbs, alcohol or drugs since your last menstrual period? (If yes, what kind and how much?)
Expert Source: American College of Obstetricians and Gynecologists
Please note: The Bump and the materials and information it contains are not intended to, and do not constitute, medical or other health advice or diagnosis and should not be used as such. You should always consult with a qualified physician or health professional about your specific circumstances.
Plus, more from The Bump:
Navigate forward to interact with the calendar and select a date. Press the question mark key to get the keyboard shortcuts for changing dates.