Take It From Me: Here’s What Midwifery Is Really All About
Whenever I’m out at a party and meet someone new, the instant they learn I’m a midwife, their birth stories come pouring forth. There’s a sort of automatic trust there, like I’ve given them permission to share something intimate. I love it. But I also occasionally get confused reactions: Some people think what I do is more like a doula or lactation consultant. Others don’t realize that Certified Nurse Midwives (CNMs), like myself, can work in hospitals and birth centers, in addition to doing home birth. But I can’t blame them: I honestly wasn’t aware of CNMs until I met one and saw for myself the amazing relationship she had with her patients.
While taking pre-med courses in college, I had the opportunity to shadow an OB. I was so excited at the start of it, but wound up being disappointed by what I saw: So much of her day revolved around surgeries insteading of spending time with her patients. I left feeling distraught. That’s not what I wanted to do—so I dropped my dream of becoming a women’s health provider. But then about four years later I met a nurse-midwife, and my whole life changed. (The vast majority of midwives in the US are Certified Nurse Midwives, who are trained nurses with a Master’s degree in nurse-midwifery and function much like nurse practitioners.) She described the work she did—spending one-on-one time with patients and tailoring her care to their individual needs—and I realized this was a career that really spoke to me.
What I learned—from her, from midwifery school and from attending over 500 births—is that a midwife’s job goes beyond ensuring a healthy birth. It’s about nurturing and respecting all of the medical and emotional aspects of pregnancy, birth and the postpartum experience. Our role is instrumental in helping women feeling good about their whole experience. And our care doesn’t stop after birth: We support women through menopause, offering everything from STD screenings to birth control to pap smears.
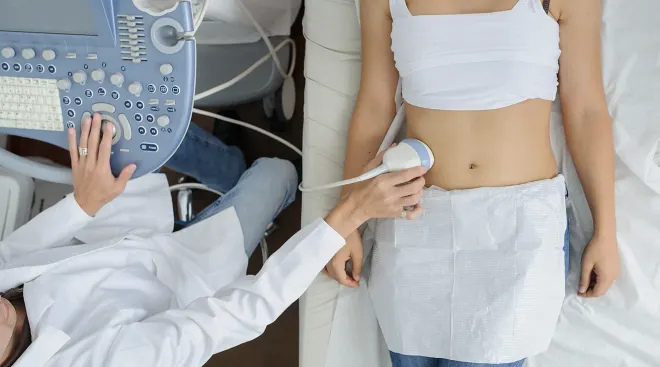
I certainly have days similar to those of an OB, where I’m in the clinic seeing lots of patients and doing prenatal check-ups, ultrasounds and women’s health exams. I clock overnight shifts at the hospital, where I sometimes attend back-to-back births. But what makes midwifery so special is what happens when I sit down with patients and have real, connective conversations. I spend an hour with my new patients and a solid 20 minutes with them during each subsequent visit. And we talk. In prenatal visits, I ask how they’re feeling about being pregnant, since you can never assume that, say, married women are excited and single women are not—it’s not that simple. I ask what kind of support they’re getting. We delve into how sleep is going and if they’re feeling anxious. I find out where they’re at and answer each and every question they have about pregnancy, using the latest evidence to support her and help her feel as stress-free and confident about the process as possible. I take the time to explain what my patients can expect, to figure out what they want and need and to help them make their own decisions. It’s shocking how many patients wind up at my door in their third trimester, deeply disappointed by the way their OB reacted to their birth plan. They were met with “we’ll see,” rather than a respectful discussion. Many other women come to me because their first birth experience was not at all what they wanted, so they asked friends who had a good birth experience about who they went to—and often, the response is “a midwife.”
It’s not that midwives are anti-intervention or anti-labor drugs. We know that about 10 to 15 percent of all births require a c-section (according to the World Health Organization), and we work with OBs who can offer any necessary interventions. And we know that getting an epidural—delivered by an anesthesiologist—doesn’t make you any less of a badass. Rather, midwifery is about making sure you have a good birth experience, even if the birth doesn’t go exactly how you first envisioned. My favorite part of my job is helping parents-to-be adapt to changes, offering them control over those changes and acknowledging that birth is one wild ride.
One of the most memorable births I’ve attended was actually a home birth transfer. She was in labor for a very, very long time and wasn’t dilating. She was exhausted by the time she got to the hopsital. I asked her how she was feeling about being there, and of course, she was not happy. She had wanted a home birth. But I assured her that her birth at the hospital could be good too, and honored her emotional and physical experience. We talked about her options and she decided on an epidural and Pitocin. It wasn’t a situation where someone barked at her, “We need to do this!” She was empowered to be fully present throughout her experience, allowing her to surrender to the moment and embrace this very different birth. She ended up having a beautiful birth and sobbed when the baby was born, thanking all of us for helping her to find her way through such a huge adjustment and to feel safe in the moment. It made the hairs on the back of my arms stand up. Those are the big wins: Having a positive experience during birth, even when it’s not at all what you expected.
There’s a saying that goes something like: “Everyone needs a midwife, and some people also need an OB.” While an OB is an unparalleled expert in pregnancy complications, that’s what they’re predominantly trained in—complications. And most women don’t have any. If you’re a normal, relatively healthy person, I truly believe you’ll be better served by a midwife. You can’t always predict what problems might arise—that’s why there are systems are in place for OBs to support midwives. CNMs work on teams with OBs so that if you need an assisted birth or c-section, they’re available to you no matter what. And midwives are here to support you. At the outset of my training, I was planning to be an international midwife, helping women in need across the globe. But then it hit me: There isn’t a high need and a low need. All women need midwifery. We all deserve it.
Rebekah Wheeler, RN, CNM, MPH, works as a nurse-midwife in California’s Bay Area. She is the founder of the Malawi Women’s Health Collective, a small non-profit that trains traditional birth attendants in rural Malawi how to detect and respond to obstetric emergencies, and has served on the boards of the California Nurse-Midwifery Association, Planned Parenthood of Rhode Island and the Women’s Health and Education Fund of Southeastern Massachusetts. She is now a proud mama of a 15-month-old and has found pregnancy, birth and motherhood to be the most humbling experiences of her life.
Published September 2017
Target Baby Registry
Free $100+ Value Welcome KitFree $100+ Value Welcome Kit
15% Completion Discount15% Completion Discount
Free 1-Year ReturnsFree 1-Year Returns
20+ Exclusive 20% Off
Deals For Mom & Baby20+ Exclusive 20% Off Deals For Mom & Baby1:1 Concierge With
Baby Gear Specialists1:1 Concierge With Baby Gear Specialists

*Subject to availability and Retailer's terms.
We earn commissions from these links.